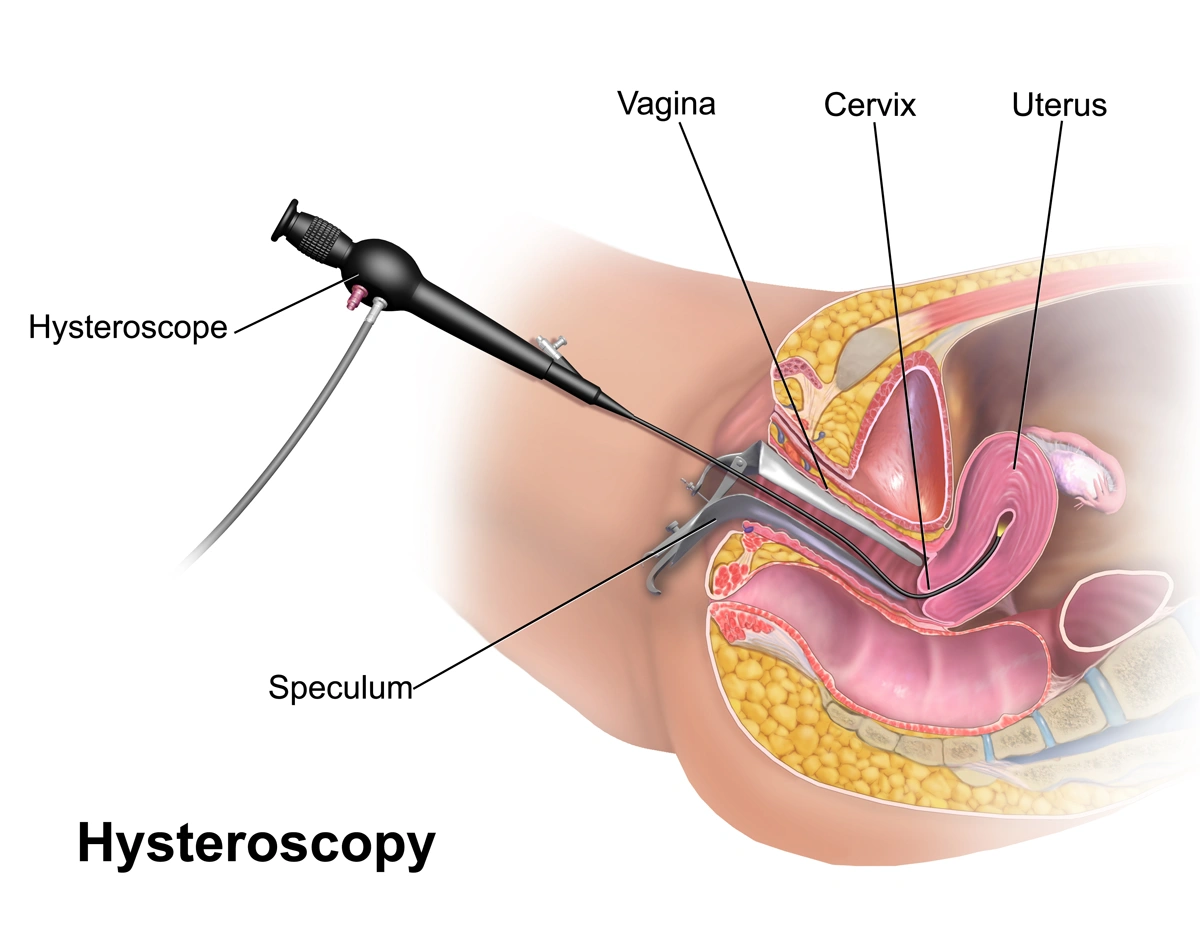
Hysteroscopy for Infertility in India: IVF Preparation, Diagnostic Evaluation & Tubal Recanalization
Hysteroscopy for infertility in India costs ₹15,000–₹1,00,000 ($180–$1,200; £140–£980). That is 60–80% less than the same procedure at private clinics in the UK. UK private clinics charge £900–£2,500 for the same test. For patients from Nigeria and the UK, this difference is large. It matters most when hysteroscopy is a step before or after a failed IVF cycle.
This guide covers four procedures that Divinheal patients commonly use in India. These are: diagnostic hysteroscopy, hysteroscopy in IVF, uterine prolapse evaluation, and tubal recanalization. You will find cost comparisons for India vs Nigeria vs the UK. You will also find outcome data, recovery times, and a clear explanation of when each procedure applies.
Reviewed by: [Name, Specialty, credentials - to be completed by Divinheal medical team before publish]. Last updated: April 2026.
What Is Diagnostic Hysteroscopy and What Can It Detect?
Diagnostic hysteroscopy is a 15–30 minute outpatient procedure. A thin, lighted telescope - called a hysteroscope - is passed through the vagina and cervix. This gives the doctor a direct view of the inside of the uterus. It is done under local or light general anaesthesia at NABH-accredited fertility hospitals in India. Patients go home the same day.
The procedure detects conditions that ultrasound and MRI often miss, including:
Uterine polyps: small growths on the uterine lining that can block embryo implantation
Fibroids: non-cancerous muscle growths in the uterine cavity that change its shape
Intrauterine adhesions (Asherman’s Syndrome): scar tissue from past infection or surgery. This narrows the uterine cavity and reduces implantation success.
Uterine septum: a wall of tissue present from birth that divides the uterine cavity, strongly linked to recurrent miscarriage
Chronic endometritis: inflammation of the uterine lining. It is found in roughly 15% of IVF patients and 42% of patients with repeated implantation failure (Cicinelli et al., Fertility and Sterility, 2015)
What Is the Difference Between Diagnostic and Operative Hysteroscopy?
Diagnostic hysteroscopy looks at the uterus only. Operative hysteroscopy both looks and treats problems in the same session. If your surgeon finds a polyp or adhesion during a diagnostic hysteroscopy, they can often remove it right away. This turns the diagnostic into an operative procedure. This combined approach is standard at Indian fertility hospitals. It saves you from needing a second anaesthesia and admission.
How Painful Is a Diagnostic Hysteroscopy?
Most patients say the discomfort feels like period cramps - brief and manageable. The procedure takes 15–30 minutes under local anaesthesia or light intravenous sedation. Mild spotting and cramping for 1–2 days after are normal. Most patients return to desk work within 24 hours and light physical activity within 48 hours. Divinheal recommends a minimum 1-night stay after any hysteroscopy before long-haul return travel.
Are You Sedated for a Hysteroscopy?
Most diagnostic hysteroscopies in India are done under light intravenous sedation or local cervical anaesthesia. You stay conscious but comfortable. Operative hysteroscopies are typically done under general anaesthesia as day-care surgery. These are procedures where tissue is removed or the uterine structure is corrected. Your anaesthesia type depends on the procedure and your doctor’s protocol. Confirm this during your pre-procedure consultation.
How Long Does Recovery from a Hysteroscopy Take?
Recovery after a diagnostic hysteroscopy takes 1–2 days. Operative hysteroscopy may need 3–5 days of reduced activity. A full menstrual cycle (4–6 weeks) is usually recommended before starting IVF after an operative procedure. Avoid tampons, swimming, and intercourse for 5–7 days after the procedure to reduce infection risk. Serious complications are rare at accredited facilities. Your doctor will tell you what warning signs to watch for.
Hysteroscopy in IVF: Does It Actually Improve Success Rates?
Hysteroscopy before IVF can improve your chances of success. It helps most if you have had implantation failures before. The procedure finds and removes problems in the uterus that block embryo attachment. Research in Fertility and Sterility found that a corrective hysteroscopy improved live birth rates by 15–30% per cycle. This was in patients with uterine cavity defects. This makes it one of the most valuable steps you can take before IVF.
The best time for the procedure is days 6–10 of your cycle - after your period but before ovulation. At this point, the uterine lining is thin and easy to see clearly. Most fertility hospitals in Delhi and Mumbai follow ICMR protocols. They scheduled a hysteroscopy at this window. IVF ovarian stimulation then begins the next menstrual cycle, once healing is confirmed.
What Is the Success Rate of IVF After Hysteroscopy?
IVF live birth rates improve by 15–30% per cycle for patients who have corrective hysteroscopy before transfer. Doctors at major Indian fertility centres - Apollo Hospitals, Fortis, and Cloudnine Hospital - report the biggest benefit for a specific group. These are women with two or more failed IVF cycles. The cause is usually polyps, adhesions, or chronic endometritis. Your outcome depends on the type and severity of the uterine issue corrected, your age, and embryo quality. Your specialist will discuss your personal prognosis after reviewing your hysteroscopy findings.
When Should You Have a Hysteroscopy Before IVF?
Your fertility specialist will likely recommend a hysteroscopy before IVF. This is most common if you have had two or more failed IVF cycles with good-quality embryos. They may also recommend it if you have a history of recurrent miscarriage or abnormal uterine bleeding. An ultrasound suggesting polyps, fibroids, or a structural irregularity is another reason. Hysteroscopy before a first IVF cycle is not always recommended. Its value is highest when there is a specific reason to suspect a uterine problem. Discuss your history with your specialist to decide.
What Happens After Hysteroscopy When Starting IVF?
Recovery from hysteroscopy is fast. Most patients resume normal activities within 1–2 days. After diagnostic hysteroscopy alone, IVF preparation can begin in the next menstrual cycle - roughly 4–6 weeks later. After operative hysteroscopy, tissue has been removed or corrected. One full menstrual cycle of healing is needed before ovarian stimulation begins. For complex procedures like large fibroid removal, a 2–3 month waiting period may apply. Your team at the NABH-accredited clinic will confirm the timeline based on your case.
Uterine Prolapse: What It Is, Its Four Stages, and When Hysteroscopy Applies
Uterine prolapse is when the uterus drops from its normal position and starts coming down into the vaginal canal. This usually happens when the pelvic muscles and ligaments weaken over time. It affects about 3–11% of women, and is more common after multiple vaginal deliveries, during menopause, or with long-term strain like heavy lifting or chronic coughing. While planning treatment, doctors may use Hysteroscopy to check inside the uterus and rule out issues like polyps or fibroids before moving ahead with surgery if needed.
The Four Stages of Uterine Prolapse
Doctors classify uterine prolapse into four stages based on how far the uterus has dropped:
Stage 1: The uterus slightly drops into the upper vagina. Most women have no symptoms at this stage.
Stage 2: At this stage, the uterus has come down to the vaginal opening (introitus), and you may start feeling a noticeable heaviness or pressure in the pelvic area, especially when standing for long periods or doing daily activities.
Stage 3: At this stage, part of the uterus comes out beyond the vaginal opening. This can cause noticeable discomfort, along with bladder problems and difficulty during intercourse.
Stage 4: The uterus is completely outside the vaginal opening. This needs prompt medical evaluation and is typically managed surgically.
How Is Uterine Prolapse Diagnosed?
Uterine prolapse is usually diagnosed with a simple pelvic examination, not scans. During the exam, your doctor may ask you to cough or bear down so they can see how much the uterus moves or drops. Ultrasound or MRI may be used in some cases to look at pelvic structures in more detail, but they don’t usually change the diagnosis itself. Most JCI-certified hospitals in India follow international staging systems used for pelvic floor disorders, so the assessment is standardized and consistent.
When prolapse repair surgery is planned, a diagnostic hysteroscopy is often done first. This checks the uterine cavity for other problems - polyps, fibroids, or adhesions - before the structural repair proceeds.
Tubal Recanalization for Infertility: How It Works and Who It Helps
Tubal recanalization is a microsurgical procedure that reconnects blocked or severed fallopian tubes. It is also called fallopian tube reversal or tubal reconnection. It is most often recommended for women who want to conceive naturally after a tubal ligation (sterilisation procedure). It is also an option for women with proximal tubal blockage. This is a blockage near where the tube meets the uterus. It is used as an alternative to IVF.
Tubal Recanalization vs IVF: Which Option Is Right for You?
The best option really depends on your tube condition, age, and what you’re hoping for. Tubal recanalization can give you the chance to conceive naturally more than once after a single procedure. IVF, on the other hand, completely bypasses the tubes and is usually a better choice if there’s significant tube damage, low ovarian reserve, or male fertility issues are also involved.
Factor | Tubal Recanalization | IVF |
Best for | Proximal blockage; post-ligation reversal; women under 40 with good ovarian reserve | Extensive tubal damage; low ovarian reserve; multiple infertility factors |
Natural conception after? | Yes - if surgery succeeds, multiple natural conceptions possible | No - each pregnancy requires a separate embryo transfer cycle |
India cost (approx.) | ₹1,50,000–₹3,00,000 ($1,800–$3,600) | ₹1,00,000–₹2,50,000 per cycle ($1,200–$3,000) |
Hospital stay | 1–2 nights | Outpatient (egg retrieval day + transfer day) |
Recovery time | 4–6 weeks restricted activity | 3–5 days per cycle |
Who Is a Good Candidate for Tubal Recanalization?
Good candidates are women under 40 whose tubes were ligated with minimal structural damage. They should have good ovarian reserve (AMH above 1.0 ng/mL) and a partner with a normal semen analysis. The key surgical predictor of success is the length of the healthy tube remaining after ligation. Surgeons at hospitals like Medanta (Gurugram) and Apollo Hospitals (Delhi) typically need at least 4–5 cm of healthy remaining tube. Without this, the procedure is not advised. Women with extensive pelvic scarring, endometriosis affecting the tubes, or low ovarian reserve are generally better served by IVF.
Is Fallopian Tube Recanalization the Same as HSG?
No - they serve different purposes. A hysterosalpingography (HSG) is a diagnostic X-ray test. It checks whether the fallopian tubes are open. It does this by injecting contrast dye through the cervix and watching its flow on imaging. Tubal recanalization is a surgical procedure. It physically reopens or reconnects a blocked or severed tube. If an HSG identifies a proximal tubal blockage, a minimally invasive procedure using a thin guide wire may help. This is called selective salpingography with tubal cannulation. It can sometimes be done in the same session. Full tubal reversal surgery after ligation is a separate, more involved laparoscopic procedure requiring a 1–2 night hospital stay.
What Are the Signs of Pregnancy After Tubal Recanalization?
Early pregnancy signs after tubal recanalization are the same as those of any pregnancy. These include a missed period, nausea, breast tenderness, and a positive hCG test. However, the repaired fallopian tube carries a 2–10% risk of ectopic pregnancy. This is where the fertilised egg implants in the tube rather than the uterus. Because of this, every positive pregnancy test after this procedure needs an urgent ultrasound at 6–7 weeks. This confirms the pregnancy is in the right place. If you have one-sided abdominal pain, dizziness, or abnormal bleeding alongside a positive test, seek immediate medical care. Ectopic pregnancy is a medical emergency.
Hysteroscopy & Tubal Recanalization Costs: India vs Nigeria vs UK
India is usually much more affordable for procedures like Diagnostic hysteroscopy and Tubal recanalization-often about 60–80% less than private care in the UK. These are 2025–2026 estimates, and the exact cost can vary depending on the hospital, doctor, and individual case. With Divinheal, you usually get a clear cost estimate before you travel. Public options like the National Health Service or Nigerian government hospitals may cost less, but waiting times are often longer, and access can be limited.
Diagnostic Hysteroscopy Costs: India vs Nigeria vs UK
Procedure | India (Approx.) | Nigeria (Approx.) | UK (Approx.) |
Diagnostic hysteroscopy (procedure only) | ₹15,000–₹40,000 ($180–$480; £140–£380) | NGN 250,000–500,000 (~$190–$370) | £1,000–£3,000 (~$1,270–$3,790) |
Operative hysteroscopy (incl. polyp/fibroid removal) | ₹30,000–₹1,00,000 ($480–$1,440; £380–£1,140) | NGN 400,000–8,00,000 (~$296–$593) | £2,500–£4,000 (~$3,150–$6,300) |
Full pre-op package (consults + tests + procedure) | ₹75,000–₹1,50,000 ($900–$1,800; £700–£1,400) | NGN 800,000–₹1,500,000 (~$593–$1,113) | £3,000–£6,000 (~$3,780–$7,560) |
Uterine prolapse diagnostic evaluation | ₹15,000–₹35,000 ($180–$420; £140–£330) | NGN 60,000–2,50,000 (~$44.50–$186) | £700–£1,800 (~$880–$2,270) |
Sources: In India, people usually go to places like Max Healthcare, Fortis Healthcare, or Apollo Hospitals. For the UK, the numbers are mostly based on NHS Reference Costs and private hospitals like BMI Healthcare. In Nigeria, it’s taken from typical fertility clinic prices in Lagos and Abuja (2025). Of course, these are just rough estimates-actual costs depend on the hospital, doctor, and your specific case.
Note: The procedure-only and full-package costs above are different things. ₹15,000–₹40,000 is the hysteroscopy procedure cost alone at most Indian hospitals. ₹75,000–₹1,50,000 is a bundled package that includes pre-operative blood tests, anaesthesia fee, consultant consultation, procedure, and post-operative care.
Tubal Recanalization Costs: India vs Nigeria vs UK
Procedure | India (Approx.) | Nigeria (Approx.) | UK (Approx.) |
Tubal reversal surgery (microsurgical reconnection) | ₹1,00,000–₹3,00,000 ($1,205–$3,600; £960–£2,800) | NGN 2,000,000–₹7,000,000 (~$1,250–$4,375) - limited availability | £5,000–£9,000 (~$6,300–$11,350) |
Selective salpingography + cannulation (proximal block) | ₹25,000–₹90,000 ($300–$720; £235–£570) | NGN 400,000–1,200,000 (~$285–$857) | £2,000–£4,500 (~$2,520–$6,075) |
Sources: In India, people usually go to places like Max Healthcare, Fortis Healthcare, or Apollo Hospitals.
Tubal recanalization surgery is rarely available in Nigerian cities at the specialist volume needed. This makes India a strong option for Nigerian patients who need this procedure. Divinheal coordinates direct appointments at specialist fertility surgery units in Delhi, Chennai, and Hyderabad.
Hysteroscopy in IVF: Cost Comparison
Procedure | India (Approx.) | Nigeria (Approx.) | UK (Approx.) |
Hysteroscopy as IVF prep (diagnostic) | ₹15,000–₹40,000 ($180–$480; £140–£380) | NGN 250,000–800,000 (~$180–$570) | £900–£2,500 (~$1,130–$3,150) |
Hysteroscopy as IVF prep (operative) | ₹40,000–₹1,20,000 ($480–$1,440; £380–£1,140) | NGN 500,000–800,000 (~$700–$1,120) | £2,500–£5,000 (~$3,150–$6,300) |
Full IVF cycle (reference) | ₹1,00,000–₹2,50,000 per cycle ($1,200–$3,000) | NGN 2,000,000–7,000,000 (~$1,300–$519) | £5,000–£8,000 (~$6,300–$10,100) |
Success Rates for Tubal Recanalization at Indian Hospitals
Pregnancy rates after tubal recanalization depend mainly on age and the quality of the remaining fallopian tube. The rates below are reported by NABH-accredited Indian centres, including Medanta (Gurugram) and Apollo Hospitals (Delhi). They are measured over 12–24 months post-surgery. These are cumulative pregnancy rates - not per-cycle rates.
Age Group | Minimal Tubal Damage | Moderate Tubal Damage | Ectopic Pregnancy Risk |
Under 35 | 60–75% | 40–55% | 2–5% |
35–39 | 45–60% | 25–40% | 5–8% |
40 and above | 20–35% | 10–20% | 8–10% |
Sources: Medanta Hospital patient outcomes data; Apollo Hospitals, Delhi fertility surgery unit. These figures represent natural conception over 12–24 months of trying. Women aged 38 and above, or those with moderate-to-severe tubal damage, may do better through IVF. Your specialist will advise based on AMH testing and a hysterosalpingography review. The ectopic pregnancy risk is why early pregnancy ultrasound confirmation is mandatory after successful recanalization.
Recovery and Post-Procedure Care: What to Expect
After Diagnostic Hysteroscopy
Recovery is usually quite quick. You may feel mild cramps or notice light spotting for a day or two, but most people are able to return to desk work within 24 hours and resume light activities in about 48 hours. To reduce the chance of infection, it’s better to avoid tampons, swimming, and intercourse for around 5–7 days. NABH-accredited clinics usually give clear aftercare instructions, and Divinheal also helps with a short, nearby stay and a follow-up appointment within a week.
After Operative Hysteroscopy
After a procedure where tissue is removed or the uterus is corrected, mild to moderate cramping for a few days (around 3–5 days) is completely normal. Most patients are able to go home the same day or after staying one night. Recovery is usually quite simple and feels similar to a Diagnostic hysteroscopy, with just a short period of taking it easy and avoiding heavy activity. If IVF is the next step, it’s typically started after the next menstrual cycle (about 4–6 weeks), once your doctor confirms that everything has healed properly.
After Tubal Recanalization Surgery
Tubal recanalization is a slightly more involved laparoscopic procedure, so a 1–2 night hospital stay is usually expected. Mild abdominal soreness for about a week is common and can be managed with medication. You’ll need to avoid heavy activity and intercourse for around 4–6 weeks while healing. Ovulation typically returns within 1–2 cycles. After the procedure, doctors usually advise trying naturally for 12–18 months before considering IVF if needed. Planning your medical trip to India with Divinheal is fairly simple, with support for appointments, travel, and coordination throughout your stay.
Planning Your Medical Trip to India with Divinheal
Divinheal takes care of your entire treatment journey to India-from booking appointments at NABH-accredited clinics to handling visa support, accommodation, and airport transfers. A dedicated coordinator stays connected with you on WhatsApp throughout your trip for any help you need.
Amaka, a 34-year-old teacher from Lagos, needed a diagnostic hysteroscopy and adhesiolysis (scar tissue removal) before her next IVF attempt. With help from Divinheal, she got an appointment at Cloudnine Hospital within 9 days. Her stay near the clinic and visa paperwork were also arranged in advance. She spent 5 days in India and returned home with her reports ready to share with her doctor. [Illustrative composite based on typical patient journeys. Name changed for privacy.]
For UK patients, waiting times on the National Health Service for a diagnostic hysteroscopy can be around 3–6 months for non-urgent cases. With Divinheal in India, patients often get a specialist appointment within 1–2 weeks, at a much lower cost compared to private UK care (£900–£2,500).
Visa and Travel Support
Divinheal assists patients from Nigeria and the UK with the Indian medical visa, which is usually approved in about 7–10 working days for straightforward cases. It’s helpful to keep digital copies of your visa, appointment letters, and medical reports on your phone so they’re easy to access when needed. Most hospitals communicate in English, and interpreter support in Yoruba, Hausa, or Igbo can also be arranged at select hospitals in Delhi and Chennai if required.
Accommodation and Local Support
Divinheal arranges your stay close to the hospital, usually within 1–2 km. You’re typically placed in a serviced apartment with basic amenities and space for a companion. Their local team handles your transport to and from the hospital, and a dedicated coordinator stays in touch with you on WhatsApp for appointments, updates, and any help you may need during your stay.
What is the success rate of IVF after hysteroscopy?
According to data in Fertility and Sterility, corrective hysteroscopy before IVF improves live birth rates by 15–30% per cycle. This applies to patients with diagnosed uterine cavity abnormalities. The biggest benefit is for women with two or more failed IVF cycles caused by polyps, adhesions, or chronic endometritis. Your outcome depends on the specific finding corrected, your age, and embryo quality. Your specialist will advise after reviewing your hysteroscopy report.
Final Thoughts
Hysteroscopy for infertility in India is available at NABH-accredited fertility hospitals at 60–80% less than private UK costs. This applies whether the procedure is diagnostic, operative, or for IVF preparation. For Nigerian patients, India offers this procedure at a competitive overall travel cost. The procedure capability and specialist volume are not reliably available in Nigeria. Tubal recanalization at Indian specialist centres gives post-ligation patients a real chance at natural conception. They do not need to commit to multiple IVF cycles.
Have you had a failed IVF cycle, unexplained infertility, uterine prolapse, or a past tubal ligation? Divinheal will connect you with a verified fertility specialist. They will provide a written cost estimate and plan your medical trip from start to finish. Reach out to a Divinheal coordinator today.
Disclaimer: All cost figures are approximate 2025–2026 estimates for private healthcare. Individual costs depend on hospital tier, surgeon experience, and case complexity. Medical decisions should be made in consultation with a qualified specialist. Patient stories are illustrative composites based on typical journeys; names changed for privacy. Citations in this article should be verified by the Divinheal medical team before publication.
Related Links
Booking With DIVINHEAL
Get a free consultation to understand your treatment options
Related Links
DivinHeal's Journey

Latest Articles
Frequently Asked Questions
Get answers to common questions about medical tourism, treatment procedures, and our comprehensive healthcare services.
Ready To Start Your Healing Journey?
Get Personalized Medical Treatment Options From India's Top Hospitals. Our Medical Experts Are Ready To Assist You Every Step Of The Way.