Centres Of Excellence
Our Centres of Excellence bring together multidisciplinary teams to deliver precise diagnosis, advanced treatments, and superior outcomes across a wide spectrum of medical specialties.

OVERVIEW
Overview of Neuro Treatment Goals and Techniques
The primary goals of Neuro treatment are to alleviate symptoms, restore neurological function, improve quality of life, and prevent disease progression. Techniques vary widely depending on the condition:
- Neurosurgery: For conditions like brain tumors, aneurysms, spinal cord injuries, and epilepsy, involving delicate procedures to remove lesions, repair structures, or implant devices.
- Medical Neurology: Management of conditions such as multiple sclerosis, Parkinson's disease, Alzheimer's disease, and migraines through pharmacotherapy, lifestyle adjustments, and rehabilitative strategies.
- Interventional Neurology: Minimally invasive procedures for stroke, aneurysms, and vascular malformations using catheters.
- Rehabilitation Therapy: Physical, occupational, and speech therapy crucial for recovery from stroke, trauma, or neurodegenerative diseases.
DivinHeal facilitates access to integrated care pathways, ensuring comprehensive and personalized treatment plans.
PROCEDURE
BENEFITS
Benefits of Advanced Neuro Treatment with DivinHeal
Hope for a Healthier Future
Opting for Neuro treatment through DivinHeal brings a multitude of advantages, fostering hope and delivering tangible positive outcomes:
- Restored Neurological Function: Many Neuro treatments aim to reduce symptoms, alleviate pain, and restore vital functions, significantly improving daily living.
- Enhanced Quality of Life: By addressing underlying conditions, patients experience a better overall quality of life, greater independence, and renewed vitality.
- Access to Top Neuro Specialists: DivinHeal connects you with India's best neurologists/neurosurgeons, renowned for their experience and high Neuro success rate in complex cases.
- Cutting-Edge Technology: Benefit from state-of-the-art diagnostic tools and advanced surgical and non-surgical therapies, including robotic assistance, neuronavigation, and minimally invasive techniques.
- Significant Cost Savings: Achieve world-class care at a fraction of the cost compared to Western countries, making vital Neuro treatment affordable.
- Reduced Recovery Time: With advanced techniques and dedicated rehabilitation, many patients experience a smoother and faster Neuro recovery time and tips.
- Comprehensive End-to-End Support: From initial consultation to post-treatment follow-up, DivinHeal provides seamless care coordination, visa assistance, and transparent pricing.
RECOVERY
Neuro Recovery Time and Tips: Your Path to Wellness
A Guided Recovery Journey
The Neuro recovery time and process can vary significantly depending on the specific treatment, the patient's overall health, and the complexity of the neurological condition. However, with dedicated care and rehabilitation, a positive outcome is always the goal.
- Immediate Post-Operative Period: For surgical Neuro treatment, the first few days involve close monitoring in an ICU or specialized neurological ward. Pain management and early mobilization are key focuses.
- Hospital Stay: Typically, a hospital stay for complex Neuro treatment ranges from 5 to 10 days, but this can extend for more intricate procedures or if complications arise.
- Rehabilitation Phase: A crucial component of Neuro recovery, rehabilitation may include physical therapy to regain strength and mobility, occupational therapy for daily living skills, and speech therapy for communication issues. This can last weeks to months.
- Outpatient Follow-ups: Regular check-ups with your neurologist/neurosurgeon are essential to monitor progress, adjust medications, and address any long-term concerns.
- Lifestyle Adjustments: Adopting a healthy lifestyle with balanced nutrition, regular gentle exercise (as advised), and stress management techniques can significantly support long-term Neuro recovery. Emotional counseling is also available to support mental well-being.
DivinHeal ensures access to comprehensive rehabilitation services and provides Neuro recovery time and tips to empower patients throughout their healing journey.
WHAT WE TREAT
Conditions Treated by Neuro Specialists
Comprehensive Care for Neurological Disorders
Our network of top neurologists and neurosurgeons in India treats a vast spectrum of neurological conditions, including:
- Brain Tumors: Gliomas, Meningiomas, Pituitary Adenomas, Acoustic Neuromas.
- Spinal Disorders: Herniated Discs, Spinal Stenosis, Spinal Tumors, Scoliosis.
- Cerebrovascular Diseases: Aneurysms, Arteriovenous Malformations (AVMs), Stroke (ischemic and hemorrhagic).
- Movement Disorders: Parkinson's Disease, Essential Tremor, Dystonia (often treated with Deep Brain Stimulation).
- Epilepsy: Medically refractory epilepsy requiring surgical intervention.
- Hydrocephalus: Shunt placement for excess cerebrospinal fluid.
- Nerve Compression Syndromes: Carpal Tunnel Syndrome, Ulnar Neuropathy.
- Neurodegenerative Diseases: Alzheimer's, Multiple Sclerosis (management).
- Traumatic Brain Injury (TBI) & Spinal Cord Injury (SCI).
DivinHeal ensures you receive expert Neuro diagnosis and therapy options tailored to your specific condition.
PREPARATION
RISKS
JOURNEY
Your DivinHeal Patient Journey for Neuro Treatment
A Seamless Path to Recovery
Your journey with DivinHeal for Neuro treatment is meticulously coordinated, ensuring peace of mind at every step:
- Initial Consultation & Diagnosis: Secure online medical record submission, expert review by top neurologists/neurosurgeons, and a personalized diagnostic plan. We arrange virtual consultations to discuss your Neuro diagnosis and therapy options.
- Treatment Planning & Visa Assistance: Once a treatment plan is established, DivinHeal provides transparent cost breakdowns, helps select the best hospitals for Neuro in India, and assists with medical visa applications and travel arrangements.
- Arrival & In-Hospital Care: Seamless airport pick-up, accommodation arrangements, and a dedicated case manager to guide you through hospital admissions, pre-operative checks, and the Neuro treatment itself. You'll receive world-class care from experienced medical teams.
- Recovery & Rehabilitation: Post-procedure, our team coordinates your Neuro recovery time and tips, including rehabilitation therapies. We ensure you have all the support needed for a comfortable convalescence before returning home.
- Post-Treatment Follow-up: DivinHeal facilitates remote follow-up consultations to monitor your progress and ensure long-term well-being, reinforcing our commitment to end-to-end care.
OUTCOMES
Successful Neuro treatment aims to significantly reduce symptoms, improve motor function, alleviate pain, and enhance cognitive abilities. Patients often experience a renewed sense of independence and a vastly improved quality of life, with long-term prognosis often excellent, fostering lasting hope.
Related Links
Doctors For Treatment in Similar Locations
Best Hospital Near by for treatment
Related Links
- Neuro cost in India
- Neuro cost in Mumbai
- Neuro cost in New Delhi
- Neuro cost in Pune
- Neuro Success Rate in Bengaluru
- Neuro Success Rate in Chennai
- Neuro Success Rate in Haryana
- Neuro Success Rate in Hyderabad
- Neuro Success Rate in India
- Neuro Success Rate in Mumbai
- Neuro Success Rate in New Delhi
- Neuro Success Rate in Pune
Other Treatments Nearby
Treatments in India for Visitors
- Neuro Treatment in Bengaluru for Bangladesh
- Neuro Treatment in Bengaluru for Ethiopia
- Neuro Treatment in Bengaluru for Iraq
- Neuro Treatment in Bengaluru for Nigeria
- Neuro Treatment in Bengaluru for UAE
- Neuro Treatment in Chennai for Bangladesh
- Neuro Treatment in Chennai for Ethiopia
- Neuro Treatment in Chennai for Iraq
- Neuro Treatment in Chennai for Nigeria
- Neuro Treatment in Chennai for UAE
- Neuro Treatment in Gurugram for Bangladesh
- Neuro Treatment in Gurugram for Ethiopia
- Neuro Treatment in Gurugram for Iraq
- Neuro Treatment in Gurugram for Nigeria
- Neuro Treatment in Gurugram for UAE
- Neuro Treatment in Hyderabad for Bangladesh
- Neuro Treatment in Hyderabad for Ethiopia
- Neuro Treatment in Hyderabad for Iraq
- Neuro Treatment in Hyderabad for Nigeria
- Neuro Treatment in Hyderabad for UAE
- Neuro Treatment in India for Bangladesh
- Neuro Treatment in India for Ethiopia
- Neuro Treatment in India for Iraq
- Neuro Treatment in India for Nigeria
- Neuro Treatment in India for UAE
- Neuro Treatment in Mumbai for Bangladesh
- Neuro Treatment in Mumbai for Ethiopia
- Neuro Treatment in Mumbai for Iraq
- Neuro Treatment in Mumbai for Nigeria
- Neuro Treatment in Mumbai for UAE
- Neuro Treatment in New Delhi for Bangladesh
- Neuro Treatment in New Delhi for Ethiopia
- Neuro Treatment in New Delhi for Iraq
- Neuro Treatment in New Delhi for Nigeria
- Neuro Treatment in New Delhi for UAE
- Neuro Treatment in Pune for Bangladesh
- Neuro Treatment in Pune for Ethiopia
- Neuro Treatment in Pune for Iraq
- Neuro Treatment in Pune for Nigeria
- Neuro Treatment in Pune for UAE
Related Treatments

Disc Herniation Surgery (Discectomy)
Treatment Price
$3500.00 USDThe primary goal of disc herniation surgery is to decompress the affected spinal nerve, which is typically achieved by removing the portion of the disc that is impinging on the nerve. Techniques often include minimally invasive microdiscectomy, laminectomy, or discectomy, focusing on precision, reduced recovery time, and optimal outcomes.
The primary goal of disc herniation surgery is to decompress the affected spinal nerve, which is typically achieved by removing the portion of the disc that is impinging on the nerve. Techniques often include minimally invasive microdiscectomy, laminectomy, or discectomy, focusing on precision, reduced recovery time, and optimal outcomes.
Treatment Overview
The primary goal of disc herniation surgery is to decompress the affected spinal nerve, which is typically achieved by removing the portion of the disc that is impinging on the nerve. Techniques often include minimally invasive microdiscectomy, laminectomy, or discectomy, focusing on precision, reduced recovery time, and optimal outcomes.
Procedures
Disc herniation surgery, particularly microdiscectomy, typically involves the following steps: 1. Anesthesia: The patient is given general anesthesia, so they are asleep throughout the procedure. 2. Incision: A small incision, usually 1-2 inches, is made in the skin over the affected area of the spine. 3. Muscle Retraction: The surgeon carefully retracts (moves aside) the back muscles to expose the spinal column. This is often done using specialized minimally invasive retractors. 4. Bone Removal (Optional): In some cases, a tiny portion of the lamina (a bone arch of the vertebra) might be removed (laminotomy or hemilaminectomy) to create a window to access the spinal canal. 5. Nerve Decompression: Using a microscope or endoscope for enhanced visualization, the surgeon carefully identifies the compressed nerve root. 6. Disc Fragment Removal: The herniated disc fragment that is pressing on the nerve is precisely removed. Only the herniated portion is removed, leaving the healthy part of the disc intact. 7. Closure: The muscles are returned to their original position, and the incision is closed with sutures or staples. The procedure typically takes 1-2 hours.
Benefits
<h2>Benefits of Disc Herniation Surgery</h2><ul><li><h3>Significant Pain Relief</h3><p>Effective in alleviating chronic back/neck pain, sciatica, or radiculopathy that hasn't responded to conservative treatments.</p></li><li><h3>Restored Mobility & Function</h3><p>Allows patients to regain flexibility, strength, and return to normal daily activities without discomfort.</p></li><li><h3>Reduced Nerve Compression</h3><p>Directly addresses the cause of neurological symptoms, preventing further nerve damage and improving sensation/strength.</p></li><li><h3>Improved Quality of Life</h3><p>Freedom from debilitating pain enhances overall well-being, mood, and ability to engage in work and leisure activities.</p></li><li><h3>Minimally Invasive Options</h3><p>Many procedures, like microdiscectomy, offer smaller incisions, less tissue damage, shorter hospital stays, and quicker recovery.</p></li></ul>
Recovery Information
<h2>Recovery and Life After Disc Herniation Surgery</h2><h3>Immediate Post-Operative Period</h3><p>Most patients experience immediate relief from nerve pain after disc herniation surgery. You will typically stay in the hospital for 1-2 days. Pain medication will be provided, and nurses will assist with gentle movement shortly after surgery to prevent stiffness and promote circulation.</p><h3>First Few Weeks (1-4 Weeks)</h3><p>During this period, rest is crucial. Avoid heavy lifting, twisting, bending, and prolonged sitting. Walking is encouraged for short periods. Physical therapy usually begins within the first week or two, focusing on gentle exercises to improve mobility, strength, and core stability. You may experience some incisional pain and muscle soreness.</p><h3>Intermediate Recovery (1-3 Months)</h3><p>Physical therapy becomes more intensive, focusing on strengthening back and abdominal muscles. Most patients can return to light work within 2-4 weeks, and more physically demanding jobs may require 6-12 weeks. Gradual return to activities like swimming or cycling can begin, always under the guidance of your therapist.</p><h3>Long-Term Recovery (3-6 Months and Beyond)</h3><p>Full recovery, including return to all previous activities and sports, can take 3 to 6 months. Continued commitment to physical therapy exercises and adopting good posture and lifting mechanics are vital for preventing recurrence. DivinHeal emphasizes comprehensive rehabilitation plans, connecting you with top physiotherapists in India to ensure a robust and lasting recovery.</p>

Brain Aneurysm Treatment (Clipping / Coiling)
Treatment Price
$8000.00 USDOverview of Brain Aneurysm Treatment Goals
Restoring Vascular Integrity and Preventing Rupture
The primary goal of brain aneurysm treatment is to seal off the aneurysm, preventing it from rupturing or re-bleeding, thereby safeguarding brain function and patient life. Modern techniques like endovascular coiling and microsurgical clipping are highly effective.
Advanced Diagnostic and Therapeutic Approaches
Treatment begins with precise diagnosis using advanced imaging such as CT angiography (CTA) or magnetic resonance angiography (MRA). Therapeutic options, chosen based on aneurysm size, location, and patient health, include:
- Endovascular Coiling: A minimally invasive procedure where platinum coils are inserted into the aneurysm to block blood flow.
- Microsurgical Clipping: A traditional open surgery where a small clip is placed at the base of the aneurysm to isolate it from the blood vessel.
- Flow Diversion: Using a stent to redirect blood flow away from the aneurysm, allowing it to heal and scar off over time.
DivinHeal facilitates access to world-class neurosurgery centers in India, renowned for their expertise in these complex procedures.
Overview of Brain Aneurysm Treatment Goals
Restoring Vascular Integrity and Preventing Rupture
The primary goal of brain aneurysm treatment is to seal off the aneurysm, preventing it from rupturing or re-bleeding, thereby safeguarding brain function and patient life. Modern techniques like endovascular coiling and microsurgical clipping are highly effective.
Advanced Diagnostic and Therapeutic Approaches
Treatment begins with precise diagnosis using advanced imaging such as CT angiography (CTA) or magnetic resonance angiography (MRA). Therapeutic options, chosen based on aneurysm size, location, and patient health, include:
- Endovascular Coiling: A minimally invasive procedure where platinum coils are inserted into the aneurysm to block blood flow.
- Microsurgical Clipping: A traditional open surgery where a small clip is placed at the base of the aneurysm to isolate it from the blood vessel.
- Flow Diversion: Using a stent to redirect blood flow away from the aneurysm, allowing it to heal and scar off over time.
DivinHeal facilitates access to world-class neurosurgery centers in India, renowned for their expertise in these complex procedures.
Treatment Overview
<h2>Overview of Brain Aneurysm Treatment Goals</h2><h3>Restoring Vascular Integrity and Preventing Rupture</h3><p>The primary goal of brain aneurysm treatment is to seal off the aneurysm, preventing it from rupturing or re-bleeding, thereby safeguarding brain function and patient life. Modern techniques like endovascular coiling and microsurgical clipping are highly effective.</p><h3>Advanced Diagnostic and Therapeutic Approaches</h3><p>Treatment begins with precise diagnosis using advanced imaging such as CT angiography (CTA) or magnetic resonance angiography (MRA). Therapeutic options, chosen based on aneurysm size, location, and patient health, include:</p><ul><li><strong>Endovascular Coiling:</strong> A minimally invasive procedure where platinum coils are inserted into the aneurysm to block blood flow.</li><li><strong>Microsurgical Clipping:</strong> A traditional open surgery where a small clip is placed at the base of the aneurysm to isolate it from the blood vessel.</li><li><strong>Flow Diversion:</strong> Using a stent to redirect blood flow away from the aneurysm, allowing it to heal and scar off over time.</li></ul><p>DivinHeal facilitates access to world-class neurosurgery centers in India, renowned for their expertise in these complex procedures.</p>
Procedures
<h3>Endovascular Coiling Procedure Details:</h3><p>1. <strong>Access:</strong> A small incision is made, usually in the groin, to access the femoral artery. A catheter is then inserted.<br/>2. <strong>Navigation:</strong> The catheter is carefully guided through the blood vessels, using real-time X-ray imaging (fluoroscopy), up into the brain and specifically to the aneurysm.<br/>3. <strong>Coil Insertion:</strong> Very thin, soft platinum coils are advanced through the catheter into the aneurysm. These coils fill the aneurysm, promoting blood clot formation (thrombosis).<br/>4. <strong>Occlusion:</strong> The coils block blood flow into the aneurysm, effectively sealing it off from the main artery.<br/>5. <strong>Closure:</strong> Once the aneurysm is packed, the catheter is removed, and pressure is applied to the groin site or a closure device is used.</p><h3>Microsurgical Clipping Procedure Details:</h3><p>1. <strong>Anesthesia and Incision:</strong> General anesthesia is administered. An incision is made in the scalp, typically behind the hairline.<br/>2. <strong>Craniotomy:</strong> A small section of the skull bone (bone flap) is carefully removed to expose the brain.<br/>3. <strong>Access to Aneurysm:</strong> Using a high-powered operating microscope, the neurosurgeon navigates through brain tissue to locate the aneurysm.<br/>4. <strong>Clipping:</strong> A tiny metal clip is placed at the neck of the aneurysm, blocking blood flow into the bulging sac.<br/>5. <strong>Closure:</strong> The bone flap is replaced and secured, and the scalp incision is closed. The patient is then woken up from anesthesia.</p><h3>Flow Diversion Procedure Details:</h3><p>1. <strong>Catheterization:</strong> Similar to coiling, a catheter is advanced from the femoral artery to the parent artery containing the aneurysm.<br/>2. <strong>Stent Deployment:</strong> A specialized braided mesh tube (flow diverter stent) is deployed across the neck of the aneurysm within the parent artery.<br/>3. <strong>Blood Flow Redirection:</strong> The stent redirects blood flow away from the aneurysm, reducing blood turbulence within it and promoting thrombosis and endothelial growth over the aneurysm neck.<br/>4. <strong>Healing:</strong> Over several months, the aneurysm remodels and scars off, effectively healing.</p>
Benefits
<h2>Benefits of Modern Brain Aneurysm Treatment</h2><p>Undergoing brain aneurysm treatment offers profound benefits, restoring peace of mind and significantly improving quality of life:</p><ul><li><strong>Prevention of Rupture:</strong> For unruptured aneurysms, treatment eliminates the risk of a life-threatening hemorrhagic stroke.</li><li><strong>Prevention of Re-Bleeding:</strong> For ruptured aneurysms, treatment prevents the highly dangerous occurrence of a second bleed.</li><li><strong>Symptom Relief:</strong> Addresses symptoms like headaches, vision problems, or nerve compression caused by the aneurysm.</li><li><strong>Improved Neurological Outcome:</strong> Timely and effective intervention helps preserve neurological function and prevents severe disability.</li><li><strong>Minimally Invasive Options:</strong> Endovascular coiling offers a less invasive approach with faster recovery times compared to traditional open surgery for suitable cases.</li></ul><p>DivinHeal partners with hospitals equipped with advanced neuro-imaging and surgical technologies, ensuring optimal outcomes for brain aneurysm patients.</p>
Recovery Information
<h2>Brain Aneurysm Treatment Recovery and Post-Procedure Care</h2><p>Recovery from brain aneurysm treatment varies based on the procedure type (endovascular vs. open surgery), the aneurysm's status (ruptured vs. unruptured), and the patient's overall health. DivinHeal provides comprehensive guidance for a smooth recovery.</p><h3>Expected Recovery Timeline:</h3><ul><li><strong>Endovascular Coiling:</strong> Hospital stay typically 2-5 days for unruptured aneurysms, longer for ruptured cases. Full recovery can take a few weeks.</li><li><strong>Microsurgical Clipping:</strong> Hospital stay usually 5-10 days, with full recovery ranging from 4-8 weeks, sometimes longer depending on individual factors.</li></ul><h3>Key Aspects of Recovery:</h3><ul><li><strong>Pain Management:</strong> Mild to moderate headaches are common and managed with medication.</li><li><strong>Activity Restrictions:</strong> Avoiding heavy lifting, strenuous activities, and anything that increases blood pressure for several weeks.</li><li><strong>Follow-up Imaging:</strong> Regular imaging (angiograms, MRI/MRA) is crucial to monitor the treated aneurysm and ensure stability.</li><li><strong>Rehabilitation:</strong> For ruptured aneurysms, physical, occupational, or speech therapy may be necessary to recover lost functions.</li><li><strong>Emotional Support:</strong> Counseling can be beneficial for patients and families coping with the psychological impact of a brain aneurysm.</li></ul><p>DivinHeal ensures access to post-operative care, including rehabilitation services and follow-up consultations, facilitating your journey back to full health.</p>

Pituitary Tumor Surgery (Transsphenoidal)
Treatment Price
$7500.00 USDPituitary Tumor Surgery: Overview and Goals
Pituitary tumor surgery aims to safely remove or reduce the size of pituitary adenomas, which are typically benign, to relieve pressure on optic nerves, reduce hormone overproduction, and improve neurological or endocrine symptoms. The most common approach is transsphenoidal surgery, offering minimal invasiveness and quicker recovery. DivinHeal ensures access to world-class neurosurgical teams utilizing advanced techniques.
Pituitary Tumor Surgery: Overview and Goals
Pituitary tumor surgery aims to safely remove or reduce the size of pituitary adenomas, which are typically benign, to relieve pressure on optic nerves, reduce hormone overproduction, and improve neurological or endocrine symptoms. The most common approach is transsphenoidal surgery, offering minimal invasiveness and quicker recovery. DivinHeal ensures access to world-class neurosurgical teams utilizing advanced techniques.
Treatment Overview
<h2>Pituitary Tumor Surgery: Overview and Goals</h2><p>Pituitary tumor surgery aims to safely remove or reduce the size of pituitary adenomas, which are typically benign, to relieve pressure on optic nerves, reduce hormone overproduction, and improve neurological or endocrine symptoms. The most common approach is transsphenoidal surgery, offering minimal invasiveness and quicker recovery. DivinHeal ensures access to world-class neurosurgical teams utilizing advanced techniques.</p>
Procedures
Pituitary tumor surgery, most commonly transsphenoidal surgery, begins with general anesthesia. The surgeon accesses the pituitary gland through the nasal cavity and sphenoid sinus using either an endoscope (endoscopic transsphenoidal) or a microscope (microscopic transsphenoidal). A small opening is made in the sphenoid bone and then the dura mater to expose the tumor. Using specialized micro-surgical instruments, the tumor is carefully dissected and removed, often in fragments. Care is taken to preserve normal pituitary tissue and surrounding vital structures like the optic nerves. After tumor removal, the surgical cavity is typically filled with fat graft or synthetic material to prevent cerebrospinal fluid leakage. The nasal passage is then closed, sometimes with nasal packing. Craniotomy, if required, involves creating an opening in the skull, usually behind the hairline, to access larger or more complex tumors.
Benefits
<h2>Benefits of Pituitary Tumor Surgery</h2><ul><li><h3>Symptom Alleviation</h3><p>Effective in relieving pressure on the optic nerves, reducing headaches, and resolving visual disturbances, significantly improving quality of life.</p></li><li><h3>Hormonal Balance Restoration</h3><p>For functional tumors, surgery can normalize hormone levels, reversing symptoms of conditions like acromegaly, Cushing's disease, or hyperprolactinemia.</p></li><li><h3>Disease Control & Prevention</h3><p>Removes or debulks the tumor, preventing further growth and potential neurological damage, and in some cases, achieving a cure.</p></li><li><h3>Minimally Invasive Options</h3><p>Transsphenoidal surgery offers a less invasive alternative to traditional brain surgery, resulting in less pain, shorter hospital stays, and quicker recovery.</p></li><li><h3>Improved Quality of Life</h3><p>By addressing the underlying cause, patients often experience a profound improvement in their overall health, energy levels, and psychological well-being.</p></li></ul>
Recovery Information
<h2>Pituitary Tumor Surgery Recovery: What to Expect</h2><p>Recovery from pituitary tumor surgery typically involves a hospital stay of 3-7 days, primarily for monitoring and managing initial post-operative symptoms. For transsphenoidal surgery, patients can expect:</p><ul><li><h3>Immediate Post-Op</h3><p>Mild nasal congestion, headache, and fatigue are common. Nasal packing may be used temporarily. Close monitoring for complications like cerebrospinal fluid (CSF) leak or diabetes insipidus.</p></li><li><h3>First Few Weeks at Home</h3><p>Avoid strenuous activities, blowing your nose, or lifting heavy objects. Gradual return to light activities. Hormonal replacement therapy might be initiated or adjusted based on post-operative endocrine function.</p></li><li><h3>Full Recovery</h3><p>Most patients can return to work or normal activities within 3-6 weeks. Full recovery, including complete resolution of symptoms and stabilization of hormone levels, can take several months. Regular follow-up with an endocrinologist and neurosurgeon is crucial for monitoring and long-term management. DivinHeal assists in coordinating these essential follow-up appointments.</p></li></ul>

decompressive craniectomy
Treatment Price
$6500.00 USDDecompressive craniectomy is primarily performed to reduce life-threatening pressure within the skull (intracranial pressure or ICP) that can result from brain swelling due to various acute neurological insults. The goal is to create space for the swollen brain, thereby improving blood flow, preventing herniation, and preserving neurological function. It involves a neurosurgeon removing a part of the skull bone (craniectomy) to allow the brain to expand, followed by a later procedure (cranioplasty) to replace the bone.
Decompressive craniectomy is primarily performed to reduce life-threatening pressure within the skull (intracranial pressure or ICP) that can result from brain swelling due to various acute neurological insults. The goal is to create space for the swollen brain, thereby improving blood flow, preventing herniation, and preserving neurological function. It involves a neurosurgeon removing a part of the skull bone (craniectomy) to allow the brain to expand, followed by a later procedure (cranioplasty) to replace the bone.
Treatment Overview
Decompressive craniectomy is primarily performed to reduce life-threatening pressure within the skull (intracranial pressure or ICP) that can result from brain swelling due to various acute neurological insults. The goal is to create space for the swollen brain, thereby improving blood flow, preventing herniation, and preserving neurological function. It involves a neurosurgeon removing a part of the skull bone (craniectomy) to allow the brain to expand, followed by a later procedure (cranioplasty) to replace the bone.
Procedures
Decompressive craniectomy involves several key steps: 1. The patient is placed under general anesthesia. 2. A curvilinear incision is made in the scalp, typically over the temporal, parietal, or frontal regions, depending on the area of swelling. 3. The scalp and muscle are retracted to expose the skull. 4. Burr holes are drilled into the skull, and a craniotome is used to connect these holes, effectively removing a portion of the skull bone (bone flap). The size and shape of the craniectomy are determined by the extent of brain swelling. 5. The dura mater (outermost brain membrane) is typically opened to allow further expansion of the brain. Often, a dural graft is used to create a larger dural opening. 6. The scalp and muscle are then carefully closed over the exposed brain, leaving the bone defect. The bone flap is either preserved for later re-implantation (cranioplasty) or discarded if it's infected or damaged. 7. A drain may be placed to remove excess fluid. The patient is then transferred to intensive care for close monitoring.
Benefits
The primary benefits of decompressive craniectomy are life-saving and include:<ul><li>Significant reduction in dangerously high intracranial pressure (ICP).</li><li>Prevention of brain herniation, which can be fatal.</li><li>Improved cerebral blood flow and oxygenation to the brain.</li><li>Potential for improved neurological outcomes and functional recovery post-injury/stroke.</li><li>Increased survival rates in patients with severe brain swelling.</li><li>Opportunity for the brain to recover from acute swelling before skull closure (cranioplasty).</li></ul>
Recovery Information
<h2>Decompressive Craniectomy Recovery Time and Tips</h2><p>Recovery from a decompressive craniectomy is a complex and often prolonged process, highly dependent on the initial neurological injury and the patient's overall health.</p><h3>Immediate Post-Operative Period (ICU Stay)</h3><ul><li>Patients are typically monitored in the Intensive Care Unit (ICU) for several days to weeks.</li><li>Focus is on managing intracranial pressure, vital signs, pain, and preventing complications like infection.</li><li>Early mobilization and neurological assessments are crucial.</li></ul><h3>Hospital Stay and Rehabilitation</h3><ul><li>Following ICU, patients may move to a regular ward and then often to a specialized neuro-rehabilitation facility.</li><li>Rehabilitation can involve physical therapy to regain motor skills, occupational therapy for daily living activities, and speech therapy for communication or swallowing difficulties.</li><li>The recovery period at this stage can range from weeks to several months.</li></ul><h3>Long-Term Recovery and Cranioplasty</h3><ul><li>The skull defect (craniectomy site) will remain open until a cranioplasty is performed, usually 3-6 months after the initial surgery. This involves replacing the bone flap or using a synthetic implant.</li><li>Patients will need to wear a protective helmet to safeguard the brain until cranioplasty.</li><li>Long-term neurological recovery can continue for months to years, with ongoing therapy and support.</li></ul><p>DivinHeal supports patients throughout their entire recovery journey, connecting them with leading rehabilitation centers and providing guidance for optimal post-operative care and long-term wellness.</p>
Minimally Invasive Brain Tumor Surgery
Treatment Price
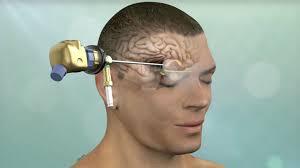
$6000.00 USDMinimally Invasive Brain Tumor Surgery focuses on precisely targeting and removing brain tumors while minimizing damage to surrounding healthy brain tissue. Techniques include neuro-endoscopy, keyhole craniotomy, and advanced stereotactic approaches, offering patients hope for effective treatment with improved safety and faster rehabilitation. DivinHeal connects you to world-class neurosurgeons and state-of-the-art facilities specializing in these advanced procedures.
Minimally Invasive Brain Tumor Surgery focuses on precisely targeting and removing brain tumors while minimizing damage to surrounding healthy brain tissue. Techniques include neuro-endoscopy, keyhole craniotomy, and advanced stereotactic approaches, offering patients hope for effective treatment with improved safety and faster rehabilitation. DivinHeal connects you to world-class neurosurgeons and state-of-the-art facilities specializing in these advanced procedures.
Treatment Overview
Minimally Invasive Brain Tumor Surgery focuses on precisely targeting and removing brain tumors while minimizing damage to surrounding healthy brain tissue. Techniques include neuro-endoscopy, keyhole craniotomy, and advanced stereotactic approaches, offering patients hope for effective treatment with improved safety and faster rehabilitation. DivinHeal connects you to world-class neurosurgeons and state-of-the-art facilities specializing in these advanced procedures.
Procedures
Minimally Invasive Brain Tumor Surgery involves several precise steps: (1) Pre-operative planning with advanced imaging (MRI, CT) and neuro-navigation mapping to create a 'roadmap' of the tumor and surrounding critical structures. (2) Anesthesia administration, followed by the patient's head being carefully positioned and secured. (3) A small incision, often just a few centimeters, is made in the scalp, or an endoscope is introduced through a natural opening like the nostril. (4) Specialized instruments, including endoscopes with high-definition cameras, microscopic tools, and laser or ultrasonic aspirators, are used to access and remove the tumor. (5) Intraoperative monitoring (e.g., brain mapping, evoked potentials) may be employed to protect neurological function. (6) Once the tumor is removed, the surgical site is meticulously closed.
Benefits
<h2>Key Benefits of Minimally Invasive Brain Tumor Surgery</h2><ul><li><h3>Reduced Surgical Trauma</h3><p>Smaller incisions lead to less damage to surrounding healthy brain tissue, reducing post-operative pain and discomfort.</p></li><li><h3>Faster Recovery Time</h3><p>Patients typically experience shorter hospital stays and a quicker return to daily activities, facilitating a more efficient rehabilitation process.</p></li><li><h3>Minimized Risk of Complications</h3><p>Lower incidence of blood loss, infection, and other surgical complications compared to traditional open procedures.</p></li><li><h3>Enhanced Cosmetic Outcomes</h3><p>Smaller incisions often result in less noticeable scarring, which can be a significant benefit for patients.</p></li><li><h3>Precision and Accuracy</h3><p>Utilizing advanced navigation systems and imaging, surgeons can achieve highly precise tumor removal, protecting vital neurological functions.</p></li><li><h3>Improved Quality of Life</h3><p>By preserving neurological function and expediting recovery, this approach aims to significantly enhance the patient's post-treatment quality of life.</p></li></ul>
Recovery Information
<h2>Recovery and Life After Minimally Invasive Brain Tumor Surgery</h2><h3>Immediate Post-Operative Period</h3><p>After Minimally Invasive Brain Tumor Surgery, patients typically spend a few days in the hospital for close monitoring. The initial recovery phase focuses on managing pain, preventing complications, and assessing neurological function. You may experience some fatigue, headache, or mild neurological symptoms, which are often temporary.</p><h3>Recovery Timeline</h3><ul><li><strong>Hospital Stay:</strong> Typically 3-7 days, depending on the tumor's complexity and individual recovery.</li><li><strong>Initial Home Recovery:</strong> The first 2-4 weeks at home involve rest, avoiding strenuous activities, and gradually increasing mobility.</li><li><strong>Full Recovery:</strong> Complete recovery can range from several weeks to a few months, varying greatly with the type of tumor, extent of surgery, and individual patient factors. Ongoing physical, occupational, or speech therapy may be required to regain full function.</li></ul><h3>Long-Term Wellness & Support</h3><p>DivinHeal emphasizes comprehensive long-term care. This includes regular follow-up appointments with your neurosurgeon and oncologist, imaging studies to monitor for recurrence, and ongoing rehabilitation. Emotional support and counseling are also vital components of recovery, helping patients and their families adjust to life after brain tumor surgery. Our dedicated care coordinators will guide you through every step, ensuring continuous access to the best post-operative care and support resources.</p>

Paediatric Neurology
Treatment Price
$5000.00 USDPaediatric Neurology treatment aims to accurately diagnose neurological disorders in children, implement effective management strategies, and provide long-term care to improve their quality of life. Techniques include advanced diagnostic imaging, genetic testing, medication management, specialized therapies (physical, occupational, speech), and lifestyle interventions, often within a multidisciplinary team approach.
Paediatric Neurology treatment aims to accurately diagnose neurological disorders in children, implement effective management strategies, and provide long-term care to improve their quality of life. Techniques include advanced diagnostic imaging, genetic testing, medication management, specialized therapies (physical, occupational, speech), and lifestyle interventions, often within a multidisciplinary team approach.
Treatment Overview
Paediatric Neurology treatment aims to accurately diagnose neurological disorders in children, implement effective management strategies, and provide long-term care to improve their quality of life. Techniques include advanced diagnostic imaging, genetic testing, medication management, specialized therapies (physical, occupational, speech), and lifestyle interventions, often within a multidisciplinary team approach.
Procedures
Paediatric Neurology treatment typically involves a thorough clinical evaluation, including detailed medical history and neurological examination. Diagnostic procedures may include MRI or CT scans of the brain/spine, Electroencephalogram (EEG) for seizure disorders, Electromyography (EMG) and Nerve Conduction Studies (NCS) for neuromuscular conditions, and genetic testing. Based on the diagnosis, a treatment plan is formulated, which can involve antiepileptic drugs, immunomodulators, neuro-rehabilitation programs (physical, occupational, speech therapy), dietary interventions, and sometimes neurosurgical consultations for specific conditions like hydrocephalus or intractable epilepsy. The approach is highly individualized, focusing on optimizing neurological function and developmental potential.
Benefits
<h2>Benefits of Expert Paediatric Neurology Care</h2><ul><li><h3>Accurate and Timely Diagnosis</h3><p>Leveraging advanced diagnostic tools and expert interpretation to identify complex neurological conditions early.</p></li><li><h3>Personalized Treatment Plans</h3><p>Tailored medical management, therapies, and interventions designed for the child's specific condition and developmental stage.</p></li><li><h3>Improved Developmental Outcomes</h3><p>Therapeutic interventions aimed at maximizing a child's physical, cognitive, and social development.</p></li><li><h3>Enhanced Quality of Life</h3><p>Effective symptom management, seizure control, and reduction of neurological deficits lead to a better quality of life for the child and family.</p></li><li><h3>Access to Multidisciplinary Teams</h3><p>Holistic care involving neurologists, neurosurgeons, therapists, geneticists, and psychologists for comprehensive support.</p></li><li><h3>Hope and Reassurance for Families</h3><p>Compassionate care and clear communication provide families with support and understanding throughout their child's journey.</p></li></ul>
Recovery Information
<h2>Recovery and Long-Term Management in Paediatric Neurology</h2><p>Recovery in Paediatric Neurology is often a journey of ongoing management, rehabilitation, and developmental support rather than a single 'cure.' For conditions like epilepsy, recovery involves achieving seizure control and minimizing medication side effects. For developmental disorders, recovery focuses on achieving developmental milestones through intensive therapies.</p><ul><li><h3>Ongoing Medical Management</h3><p>Regular follow-ups, medication adjustments, and monitoring of the child's neurological status are essential.</p></li><li><h3>Rehabilitation Therapies</h3><p>Physical therapy, occupational therapy, and speech therapy are crucial for improving motor skills, daily living activities, and communication.</p></li><li><h3>Educational and Behavioral Support</h3><p>Specialized educational programs and behavioral interventions may be necessary to support learning and social development.</p></li><li><h3>Family Support and Counselling</h3><p>Providing resources, support groups, and psychological counseling for families navigating the challenges of a child's neurological condition.</p></li><li><h3>Lifestyle Modifications</h3><p>Implementing dietary changes (e.g., ketogenic diet for epilepsy) and promoting healthy sleep patterns and physical activity.</p></li></ul><p>DivinHeal's comprehensive care extends to coordinating post-treatment follow-ups and connecting families with long-term rehabilitation and support networks, ensuring sustained progress and well-being.</p>

Vagus Nerve Stimulation (VNS) Implant
Treatment Price
$10500.00 USDThe VNS Implant therapy aims to reduce the frequency and severity of seizures in patients with epilepsy who do not respond well to medication, or to alleviate symptoms of severe, chronic depression that has not improved with standard treatments. The device is typically placed under the skin in the chest, with an electrode wire tunnelled under the skin and wrapped around the left vagus nerve in the neck, delivering programmed electrical pulses to the brain to modulate neural activity.
The VNS Implant therapy aims to reduce the frequency and severity of seizures in patients with epilepsy who do not respond well to medication, or to alleviate symptoms of severe, chronic depression that has not improved with standard treatments. The device is typically placed under the skin in the chest, with an electrode wire tunnelled under the skin and wrapped around the left vagus nerve in the neck, delivering programmed electrical pulses to the brain to modulate neural activity.
Treatment Overview
The VNS Implant therapy aims to reduce the frequency and severity of seizures in patients with epilepsy who do not respond well to medication, or to alleviate symptoms of severe, chronic depression that has not improved with standard treatments. The device is typically placed under the skin in the chest, with an electrode wire tunnelled under the skin and wrapped around the left vagus nerve in the neck, delivering programmed electrical pulses to the brain to modulate neural activity.
Procedures
The Vagus Nerve Stimulation (VNS) Implant procedure is typically performed under general anesthesia and usually takes about 1 to 1.5 hours. It involves two main incisions: one in the upper left chest and another horizontally in the lower left side of the neck. Through the chest incision, a small pocket is created beneath the skin, where the VNS pulse generator (the battery and electronics) is placed. A lead wire from the pulse generator is then tunnelled under the skin up to the neck incision. In the neck, the left vagus nerve is carefully identified, and the lead wire is gently wrapped around it. The incisions are then closed, and the device is usually not activated until a follow-up appointment, typically 1-2 weeks later, to allow for initial healing. The device is then programmed wirelessly by a clinician to deliver specific electrical pulses.
Benefits
The primary benefits of a Vagus Nerve Stimulation (VNS) Implant include:<br/><ul><li><b>Seizure Reduction:</b> Significantly reduces the frequency and severity of seizures in patients with refractory epilepsy, with some experiencing long-term seizure freedom.</li><li><b>Improved Mood:</b> Provides sustained relief from symptoms of treatment-resistant depression, leading to enhanced emotional well-being and functionality.</li><li><b>Fewer Side Effects:</b> Generally associated with fewer systemic side effects compared to oral medications, as the stimulation is targeted.</li><li><b>Enhanced Quality of Life:</b> Patients often report better alertness, cognitive function, and overall quality of life due to reduced seizure burden or improved mood.</li><li><b>Programmable and Adjustable:</b> The device settings can be non-invasively adjusted by a clinician to optimize therapeutic effects and manage side effects.</li><li><b>Patient-Controlled Magnet:</b> Patients can use a magnet to deliver an additional burst of stimulation, which can abort or lessen the severity of a seizure or alleviate depressive symptoms.</li></ul>
Recovery Information
<h3>Vagus Nerve Stimulation (VNS) Implant Recovery Time and Tips</h3><p>Recovery from a VNS implant is generally straightforward. Most patients are discharged within 1-2 days post-surgery. The surgical sites (chest and neck) will heal over a few weeks. Initial recovery primarily involves managing mild pain or discomfort, which can be controlled with over-the-counter pain relievers.</p><h4>Immediate Post-Op Care:</h4><ul><li>Keep the incision sites clean and dry; follow wound care instructions.</li><li>Avoid strenuous activities, heavy lifting, or anything that might strain the neck or chest for several weeks.</li><li>Mild hoarseness, throat discomfort, or coughing may occur initially but usually subside.</li></ul><h4>Long-term Recovery and Device Management:</h4><ul><li>The VNS device is typically activated 1-2 weeks after surgery to allow for initial healing.</li><li>Subsequent programming sessions, often spanning several months, are crucial for optimizing the stimulation settings to achieve the best therapeutic results with minimal side effects.</li><li>Regular follow-up appointments with your neurologist or psychiatrist are essential for monitoring the device, checking battery life (which typically lasts 5-10 years), and assessing your ongoing response to therapy.</li><li>Patients learn to use a hand-held magnet for additional stimulation if needed.</li></ul><p>Adhering to your doctor's instructions and attending all follow-up appointments are key to a successful recovery and long-term management with your VNS Implant.</p>

epilepsy treatment
Treatment Price
$3500.00 USDEpilepsy Treatment Overview
Epilepsy management involves a multidisciplinary approach, starting with accurate diagnosis through neurological exams, EEGs, and imaging. Treatment goals typically include achieving seizure freedom or significantly reducing seizure frequency, optimizing medication regimens, and exploring advanced therapies like epilepsy surgery, Vagus Nerve Stimulation (VNS), or Deep Brain Stimulation (DBS) for suitable candidates. DivinHeal connects you with world-class neurologists and state-of-the-art facilities dedicated to effective epilepsy care.
Epilepsy Treatment Overview
Epilepsy management involves a multidisciplinary approach, starting with accurate diagnosis through neurological exams, EEGs, and imaging. Treatment goals typically include achieving seizure freedom or significantly reducing seizure frequency, optimizing medication regimens, and exploring advanced therapies like epilepsy surgery, Vagus Nerve Stimulation (VNS), or Deep Brain Stimulation (DBS) for suitable candidates. DivinHeal connects you with world-class neurologists and state-of-the-art facilities dedicated to effective epilepsy care.
Treatment Overview
<h2>Epilepsy Treatment Overview</h2><p>Epilepsy management involves a multidisciplinary approach, starting with accurate diagnosis through neurological exams, EEGs, and imaging. Treatment goals typically include achieving seizure freedom or significantly reducing seizure frequency, optimizing medication regimens, and exploring advanced therapies like epilepsy surgery, Vagus Nerve Stimulation (VNS), or Deep Brain Stimulation (DBS) for suitable candidates. DivinHeal connects you with world-class neurologists and state-of-the-art facilities dedicated to effective epilepsy care.</p>
Procedures
Epilepsy treatment involves a range of strategies tailored to the individual. The most common approach is pharmacotherapy, where anti-epileptic drugs (AEDs) are prescribed to control seizures by stabilizing brain electrical activity. If medications are ineffective, patients may be evaluated for epilepsy surgery, which aims to remove the seizure-generating part of the brain (resective surgery) or disrupt seizure pathways (e.g., corpus callosotomy). Neurostimulation devices like Vagus Nerve Stimulation (VNS), Deep Brain Stimulation (DBS), or Responsive Neurostimulation (RNS) involve implanting a device to deliver electrical impulses to the brain or nerves, helping to reduce seizure frequency. Additionally, dietary therapies like the ketogenic diet can be used, particularly in children. Each treatment is chosen based on the type of epilepsy, seizure frequency, location of seizure onset, and patient's overall health.
Benefits
<h2>Benefits of Effective Epilepsy Treatment</h2><ul><li><h3>Improved Seizure Control</h3><p>Significant reduction in seizure frequency and severity, often leading to seizure freedom.</p></li><li><h3>Enhanced Quality of Life</h3><p>Greater independence, improved daily functioning, and participation in social and professional activities.</p></li><li><h3>Reduced Risk of Injury</h3><p>Lower incidence of falls, accidents, and other seizure-related complications.</p></li><li><h3>Better Cognitive Function</h3><p>Minimizing the impact of seizures and some medications on memory, concentration, and learning.</p></li><li><h3>Emotional Well-being</h3><p>Reduced anxiety and depression associated with living with epilepsy, fostering hope and resilience.</p></li></ul>
Recovery Information
<h2>Epilepsy Treatment Recovery Time and Tips</h2><p>For most patients on medication, "recovery" refers to achieving stable seizure control and managing side effects. For those undergoing <a href="/epilepsy-treatment-surgery-cost-comparison">epilepsy surgery</a>, the <a href="/epilepsy-treatment-recovery-time-and-tips">recovery time</a> typically involves a hospital stay of 3-7 days, followed by several weeks to months for complete healing and adaptation.</p><ul><li><h3>Post-Surgical Care</h3><p>Follow your surgeon’s instructions for wound care, pain management, and activity restrictions. Gradual return to normal activities is advised.</p></li><li><h3>Medication Adherence</h3><p>Continue taking anti-epileptic medications as prescribed, even after surgery, as dosage adjustments may be gradual.</p></li><li><h3>Lifestyle Adjustments</h3><p>Prioritize adequate sleep, manage stress, avoid alcohol and recreational drugs, and identify personal seizure triggers.</p></li><li><h3>Follow-up Appointments</h3><p>Regular visits with your neurologist are essential for monitoring seizure control, medication efficacy, and overall neurological health.</p></li><li><h3>Support & Counseling</h3><p>Engaging with support groups or seeking emotional counseling can significantly aid in adapting to life with epilepsy.</p></li></ul>

vp shunt surgery
Treatment Price
$4500.00 USDThe primary goal of VP shunt surgery is to normalize intracranial pressure and prevent further brain damage caused by excess CSF. The procedure involves implanting a flexible tube (catheter) into a brain ventricle, connecting it to a pressure-regulating valve, and then tunneling another catheter under the skin to the peritoneal cavity. This system continuously drains CSF, alleviating symptoms of hydrocephalus and improving the patient's quality of life. DivinHeal connects you to top neurosurgeons for precise and safe VP shunt surgery treatment.
The primary goal of VP shunt surgery is to normalize intracranial pressure and prevent further brain damage caused by excess CSF. The procedure involves implanting a flexible tube (catheter) into a brain ventricle, connecting it to a pressure-regulating valve, and then tunneling another catheter under the skin to the peritoneal cavity. This system continuously drains CSF, alleviating symptoms of hydrocephalus and improving the patient's quality of life. DivinHeal connects you to top neurosurgeons for precise and safe VP shunt surgery treatment.
Treatment Overview
The primary goal of VP shunt surgery is to normalize intracranial pressure and prevent further brain damage caused by excess CSF. The procedure involves implanting a flexible tube (catheter) into a brain ventricle, connecting it to a pressure-regulating valve, and then tunneling another catheter under the skin to the peritoneal cavity. This system continuously drains CSF, alleviating symptoms of hydrocephalus and improving the patient's quality of life. DivinHeal connects you to top neurosurgeons for precise and safe VP shunt surgery treatment.
Procedures
VP shunt surgery is performed under general anesthesia. The neurosurgeon makes a small incision on the scalp, behind the ear, and another in the abdomen. A burr hole is drilled in the skull, and a ventricular catheter is carefully guided into one of the brain's ventricles. The valve is then secured under the skin behind the ear, connected to the ventricular catheter. Finally, a peritoneal catheter is tunneled under the skin, from the valve to the abdominal incision, where it's placed into the peritoneal cavity. The incisions are then closed. The entire system remains beneath the skin, invisible to the eye.
Benefits
<h2>Benefits of VP Shunt Surgery Treatment</h2><ul><li><strong>Symptom Relief:</strong> Effectively alleviates symptoms of hydrocephalus such as headaches, nausea, vomiting, vision problems, and cognitive impairment.</li><li><strong>Prevents Brain Damage:</strong> Reduces intracranial pressure, preventing progressive brain damage and preserving neurological function.</li><li><strong>Improved Quality of Life:</strong> Patients often experience a significant improvement in their daily functioning, mobility, and overall well-being.</li><li><strong>Long-Term Management:</strong> Provides a durable solution for chronic hydrocephalus, offering sustained relief for many years.</li><li><strong>Safety and Expertise:</strong> Performed by highly skilled neurosurgeons, with established safety protocols, particularly in DivinHeal's network of best hospitals for vp shunt surgery.</li></ul>
Recovery Information
<h2>VP Shunt Surgery Recovery Time and Tips</h2><h3>Immediate Post-Operative Period</h3><p>After VP shunt surgery, patients typically stay in the hospital for 3-7 days. During this time, vital signs are closely monitored, pain is managed, and the surgical site is observed for any signs of infection. Early mobilization is encouraged under medical supervision.</p><h3>Short-Term Recovery (Weeks 1-6)</h3><ul><li><strong>Wound Care:</strong> Keep the incision sites clean and dry. Follow specific instructions regarding dressing changes.</li><li><strong>Activity Restrictions:</strong> Avoid strenuous activities, heavy lifting, and contact sports to prevent damage to the shunt system.</li><li><strong>Head Position:</strong> Avoid sudden movements or positions that might strain the neck or head.</li><li><strong>Monitoring Symptoms:</strong> Be vigilant for any signs of shunt malfunction or infection (e.g., persistent headaches, fever, nausea, redness along the shunt path).</li></ul><h3>Long-Term Recovery and Living with a Shunt</h3><p>Full recovery and adjustment to living with a shunt can take several weeks to months. Regular follow-up appointments with a neurosurgeon are crucial to monitor shunt function and address any concerns. Patients with a VP shunt can generally lead normal, active lives, but specific precautions may be advised for certain activities. DivinHeal offers comprehensive support throughout your vp shunt surgery recovery, connecting you with rehabilitation services and follow-up care.</p>
Endovascular Thrombectomy for Stroke
Treatment Price
$12000.00 USDEndovascular Thrombectomy: Restoring Life-Saving Blood Flow to the Brain
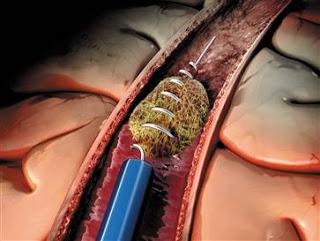
Endovascular Thrombectomy for Stroke is a revolutionary interventional neurovascular procedure aimed at rapidly removing large vessel occlusions (LVOs) in the brain, which are responsible for the most severe forms of ischemic stroke. The primary goal is to re-establish blood flow to the brain within the critical 'golden hour' window – often up to 24 hours in selected cases – minimizing brain damage and improving neurological recovery. This procedure involves threading a catheter through an artery, typically in the groin, up to the brain to physically extract or aspirate the clot, offering hope for significantly reduced disability.
Endovascular Thrombectomy: Restoring Life-Saving Blood Flow to the Brain
Endovascular Thrombectomy for Stroke is a revolutionary interventional neurovascular procedure aimed at rapidly removing large vessel occlusions (LVOs) in the brain, which are responsible for the most severe forms of ischemic stroke. The primary goal is to re-establish blood flow to the brain within the critical 'golden hour' window – often up to 24 hours in selected cases – minimizing brain damage and improving neurological recovery. This procedure involves threading a catheter through an artery, typically in the groin, up to the brain to physically extract or aspirate the clot, offering hope for significantly reduced disability.
Treatment Overview
<h2>Endovascular Thrombectomy: Restoring Life-Saving Blood Flow to the Brain</h2><p>Endovascular Thrombectomy for Stroke is a revolutionary interventional neurovascular procedure aimed at rapidly removing large vessel occlusions (LVOs) in the brain, which are responsible for the most severe forms of ischemic stroke. The primary goal is to re-establish blood flow to the brain within the critical 'golden hour' window – often up to 24 hours in selected cases – minimizing brain damage and improving neurological recovery. This procedure involves threading a catheter through an artery, typically in the groin, up to the brain to physically extract or aspirate the clot, offering hope for significantly reduced disability.</p>
Procedures
<h2>Endovascular Thrombectomy for Stroke: Step-by-Step Procedure Details</h2><p>The Endovascular Thrombectomy for Stroke procedure is a highly complex, time-sensitive intervention performed by specialized neurointerventionalists in a sterile neuro-interventional suite or cath lab:</p><ol><li><strong>Patient Preparation and Anesthesia:</strong> The patient is positioned, draped, and often sedated or given general anesthesia. The groin area is prepped and sterilized, and local anesthesia is applied at the puncture site (usually the femoral artery).</li><li><strong>Arterial Access:</strong> A small incision or puncture is made in the femoral artery. A guiding catheter and guidewire are inserted into the artery.</li><li><strong>Catheter Navigation to the Brain:</strong> Under continuous fluoroscopic (real-time X-ray) guidance, the guiding catheter is carefully advanced through the aorta, into the major arteries of the neck (carotid or vertebral arteries), and then into the cerebral arteries of the brain, precisely reaching the site of the blood clot.</li><li><strong>Clot Retrieval or Aspiration:</strong> Once the guiding catheter is positioned near the clot, a microcatheter is advanced through it, and one of two primary methods is typically employed:<ul><li><strong>Stent Retriever:</strong> A self-expanding mesh stent retriever is deployed through the microcatheter, extending across and beyond the clot. It is left in place for several minutes to allow the clot to integrate into the stent's mesh. Then, the stent and the captured clot are slowly and carefully retrieved into a larger aspiration catheter, effectively removing the blockage.</li><li><strong>Direct Aspiration:</strong> A large-bore aspiration catheter is advanced directly to the face of the clot. Powerful vacuum suction is then applied to aspirate (suck out) the clot fragments directly into the catheter. Sometimes, these methods are combined for optimal results.</li></ul></li><li><strong>Confirmation of Recanalization:</strong> After clot removal, angiography is performed again to confirm successful recanalization (restored blood flow) to the affected brain region and to check for any residual blockages, vessel damage, or complications.</li><li><strong>Closure of Access Site:</strong> Once successful recanalization is confirmed and the catheters are withdrawn, the access site in the groin is closed using a specialized closure device or manual compression.</li></ol><p>Throughout the procedure, the patient's vital signs, brain activity, and neurological status are closely monitored. The entire process typically takes 30 minutes to a few hours, depending on the clot's complexity and vessel anatomy, but every minute is critical for preserving brain tissue.</p>
Benefits
<h2>Key Benefits of Endovascular Thrombectomy for Stroke</h2><ul><li><h3>Significantly Improved Neurological Outcomes</h3><p>For eligible patients, Endovascular Thrombectomy for Stroke dramatically increases the chances of functional independence, leading to better long-term quality of life compared to conventional treatments alone.</p></li><li><h3>Reduced Long-Term Disability</h3><p>By rapidly restoring blood flow to brain tissue at risk, the procedure minimizes permanent brain damage, thereby reducing severe long-term disability, including motor, speech, and cognitive impairments.</p></li><li><h3>Higher Chance of Full Recovery</h3><p>Many patients who undergo timely Endovascular Thrombectomy for Stroke experience a significant reduction in stroke-related deficits, with a higher probability of returning to a near-normal, independent lifestyle.</p></li><li><h3>Minimally Invasive Approach</h3><p>This catheter-based procedure involves only a small incision, typically in the groin, resulting in less pain, fewer complications, and a faster initial recovery compared to traditional open surgical interventions.</p></li><li><h3>Life-Saving Intervention</h3><p>In cases of acute large vessel occlusion, Endovascular Thrombectomy for Stroke is often the only intervention capable of preventing severe, debilitating, or fatal outcomes, making it a critical, life-saving treatment.</p></li></ul>
Recovery Information
<h2>Endovascular Thrombectomy for Stroke: Recovery Time and Rehabilitation Tips</h2><ul><li><h3>Immediate Post-Procedure Monitoring (1-3 days)</h3><p>Patients typically spend 1-3 days in a specialized neuro-intensive care unit (NICU) or stroke unit for continuous neurological monitoring, blood pressure control, and management of any potential complications. Early signs of neurological improvement are closely observed.</p></li><li><h3>Hospital Stay (3-7 days)</h3><p>The total hospital stay usually ranges from 3 to 7 days, during which time early mobilization, swallowing assessments, and initial rehabilitation assessments begin to tailor a personalized recovery plan.</p></li><li><h3>Rehabilitation Phase (Weeks to Months)</h3><p>Depending on the extent of neurological deficit, patients may require intensive inpatient or outpatient rehabilitation, including physical therapy (PT), occupational therapy (OT), and speech therapy (ST). Early, consistent, and specialized rehabilitation is crucial for optimizing functional recovery and regaining lost abilities.</p></li><li><h3>Long-Term Follow-up & Prevention</h3><p>Regular follow-up appointments with neurologists are essential to monitor progress, manage stroke risk factors (e.g., hypertension, diabetes, high cholesterol), and adjust medications. Lifestyle modifications, including a healthy diet, regular exercise, and smoking cessation, play a vital role in preventing future strokes.</p></li><li><h3>Emotional & Psychological Support</h3><p>Recovering from a stroke can be emotionally challenging for both patients and their families. Access to support groups, psychological counseling, and resources for coping with post-stroke depression or anxiety can be invaluable. DivinHeal assists in connecting patients with comprehensive rehabilitation and long-term support services.</p></li></ul>
Deep Brain Stimulation (DBS)
Treatment Price
$15000.00 USDOverview of Deep Brain Stimulation (DBS)
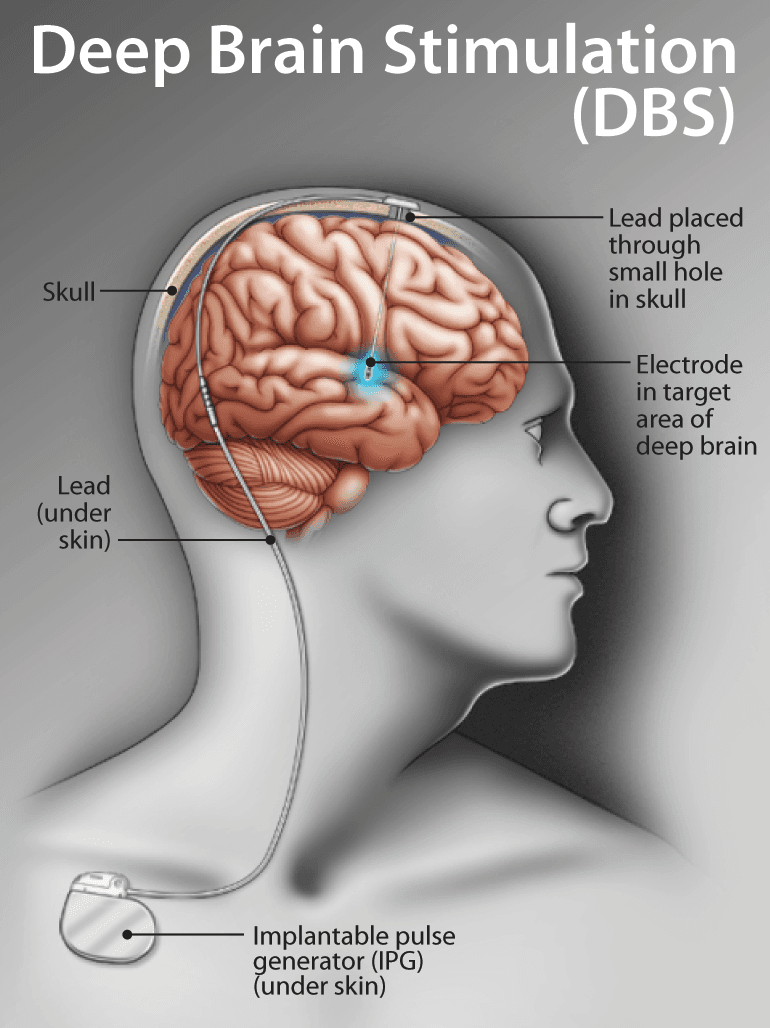
Deep Brain Stimulation (DBS) aims to modulate abnormal brain activity responsible for severe neurological symptoms. By delivering precisely targeted electrical pulses, DBS can significantly reduce tremors, rigidity, and dyskinesia, improving motor function and quality of life for patients unresponsive to medication. The procedure involves placing thin electrodes in specific brain regions, connected to a pulse generator implanted under the skin, typically near the collarbone.
Overview of Deep Brain Stimulation (DBS)
Deep Brain Stimulation (DBS) aims to modulate abnormal brain activity responsible for severe neurological symptoms. By delivering precisely targeted electrical pulses, DBS can significantly reduce tremors, rigidity, and dyskinesia, improving motor function and quality of life for patients unresponsive to medication. The procedure involves placing thin electrodes in specific brain regions, connected to a pulse generator implanted under the skin, typically near the collarbone.
Treatment Overview
<h2>Overview of Deep Brain Stimulation (DBS)</h2><p>Deep Brain Stimulation (DBS) aims to modulate abnormal brain activity responsible for severe neurological symptoms. By delivering precisely targeted electrical pulses, DBS can significantly reduce tremors, rigidity, and dyskinesia, improving motor function and quality of life for patients unresponsive to medication. The procedure involves placing thin electrodes in specific brain regions, connected to a pulse generator implanted under the skin, typically near the collarbone.</p>
Procedures
Deep Brain Stimulation (DBS) involves two main surgical stages. First, precise targeting: using advanced imaging (MRI, CT scans) and sometimes microelectrode recording (MER), the neurosurgeon identifies the exact brain region (e.g., subthalamic nucleus or globus pallidus internus) for electrode placement. The patient may be awake during part of this stage to allow for neurological testing. Second, electrode implantation: thin, insulated wires with multiple contacts (electrodes) are carefully inserted into the targeted brain areas. These electrodes are then tunneled under the skin and connected to an extension wire, which is in turn connected to the neurostimulator (IPG). The IPG, a small, battery-powered device, is typically implanted in a separate procedure under the skin in the chest area, similar to a cardiac pacemaker. Once activated, the IPG delivers continuous electrical pulses to the brain through the implanted electrodes, modulating abnormal brain activity.
Benefits
<h2>Benefits of Deep Brain Stimulation (DBS) Treatment</h2><ul><li><h3>Significant Symptom Control:</h3><p>Reduces tremors, rigidity, bradykinesia, and dyskinesia, offering relief when medications are no longer effective.</p></li><li><h3>Improved Quality of Life:</h3><p>Enhances motor function, independence, and ability to perform daily activities.</p></li><li><h3>Reduced Medication Dependency:</h3><p>Often allows for a reduction in daily medication dosage, minimizing drug-related side effects.</p></li><li><h3>Adjustable Therapy:</h3><p>Stimulation parameters can be non-invasively adjusted post-surgery to optimize symptom control over time.</p></li><li><h3>Reversible:</h3><p>Unlike ablative procedures, DBS is reversible, and the device can be turned off or removed if necessary.</p></li><li><h3>Sustained Efficacy:</h3><p>Provides long-term symptomatic relief for many patients.</p></li></ul>
Recovery Information
<h2>Deep Brain Stimulation (DBS) Recovery & Post-Procedure Care</h2><ul><li><h3>Immediate Post-operative Care:</h3><p>Typically involves a hospital stay of 3-7 days for monitoring and initial recovery. Patients may experience mild discomfort or swelling at incision sites.</p></li><li><h3>Device Programming:</h3><p>The neurostimulator is usually programmed a few weeks after surgery, allowing the brain to heal. This involves several outpatient visits to fine-tune stimulation settings for optimal symptom control.</p></li><li><h3>Physical & Occupational Therapy:</h3><p>Rehabilitation may be recommended to maximize functional gains, especially for patients with long-standing motor impairments.</p></li><li><h3>Long-term Management:</h3><p>Regular follow-ups with the neurologist are crucial for battery checks, programming adjustments, and overall symptom management. Battery replacement is typically needed every 3-5 years for non-rechargeable devices, or less frequently for rechargeable ones.</p></li><li><h3>Lifestyle Adjustments:</h3><p>Patients are advised to avoid strong magnetic fields and inform medical professionals about their DBS device during other medical procedures.</p></li></ul>

movement disorder treatment
Treatment Price
$7000.00 USDOverview of Movement Disorder Management
Effective movement disorder treatment aims to restore functional independence and reduce the impact of involuntary or impaired movements. Techniques span from precise medication titration and advanced rehabilitative therapies (physical, occupational, speech) to innovative surgical options like Deep Brain Stimulation (DBS) or focused ultrasound. DivinHeal ensures access to cutting-edge diagnostics and personalized treatment protocols delivered by leading specialists, focusing on improving patient outcomes and overall well-being.
Overview of Movement Disorder Management
Effective movement disorder treatment aims to restore functional independence and reduce the impact of involuntary or impaired movements. Techniques span from precise medication titration and advanced rehabilitative therapies (physical, occupational, speech) to innovative surgical options like Deep Brain Stimulation (DBS) or focused ultrasound. DivinHeal ensures access to cutting-edge diagnostics and personalized treatment protocols delivered by leading specialists, focusing on improving patient outcomes and overall well-being.
Treatment Overview
<h2>Overview of Movement Disorder Management</h2><p>Effective <b>movement disorder treatment</b> aims to restore functional independence and reduce the impact of involuntary or impaired movements. Techniques span from precise medication titration and advanced rehabilitative therapies (physical, occupational, speech) to innovative surgical options like Deep Brain Stimulation (DBS) or focused ultrasound. DivinHeal ensures access to cutting-edge diagnostics and personalized treatment protocols delivered by leading specialists, focusing on improving patient outcomes and overall well-being.</p>
Procedures
Movement disorder treatment involves a meticulously planned, multi-stage process. Initially, thorough diagnostic evaluations are conducted, including detailed neurological examinations, advanced imaging (MRI, CT, PET scans), and sometimes genetic testing to pinpoint the specific disorder and its severity. Following diagnosis, a personalized treatment strategy is formulated by a multidisciplinary team. This plan may include pharmacological interventions, where medications are carefully selected and titrated to manage symptoms like tremors, rigidity, and dyskinesia. For conditions like dystonia, targeted botulinum toxin injections may be administered to relax specific muscles. Rehabilitative therapies, such as physical therapy to improve gait and balance, occupational therapy for daily living activities, and speech therapy for communication or swallowing difficulties, form a cornerstone of treatment. In suitable cases, advanced neurosurgical procedures like Deep Brain Stimulation (DBS) are performed. This involves implanting electrodes in specific brain regions connected to a neurostimulator, which delivers electrical impulses to modulate abnormal brain activity. Focused ultrasound is another non-invasive surgical option for certain tremors. Throughout the entire process, continuous monitoring, dose adjustments, and patient education are integral to optimizing outcomes and enhancing the patient's quality of life.
Benefits
<h2>Key Benefits of Advanced Movement Disorder Treatment</h2><ul><li><h3>Significant Symptom Reduction</h3><p>Effective therapies aim to markedly reduce debilitating symptoms like tremors, rigidity, bradykinesia, and dyskinesias, restoring greater control over movements.</p></li><li><h3>Enhanced Quality of Life</h3><p>Patients experience improved ability to perform daily activities, leading to greater independence, social engagement, and overall well-being.</p></li><li><h3>Personalized Care Plans</h3><p>Treatment is meticulously tailored to each patient's specific diagnosis, symptom profile, and lifestyle, ensuring the most effective and least invasive approach.</p></li><li><h3>Access to Innovative Therapies</h3><p>Benefit from the latest advancements, including advanced pharmacological agents, precise botulinum toxin injections, and neurosurgical interventions like Deep Brain Stimulation (DBS) or Focused Ultrasound.</p></li><li><h3>Multidisciplinary Support</h3><p>A team of neurologists, neurosurgeons, therapists, and psychologists collaborate to provide holistic care, addressing both physical and psychological aspects of the disorder.</p></li><li><h3>Improved Prognosis & Disease Management</h3><p>Timely and appropriate treatment can slow disease progression in some conditions and effectively manage symptoms long-term, optimizing patient outcomes.</p></li></ul>
Recovery Information
<h2>Recovery and Rehabilitation After Movement Disorder Treatment</h2><p>The recovery process following <b>movement disorder treatment</b> varies significantly depending on the specific therapy undertaken. For medical management, recovery is often about symptom stabilization and adaptation to new medication regimens, which can be an ongoing process. Post-surgical interventions like Deep Brain Stimulation (DBS) typically involve a hospital stay of 3-7 days, followed by several weeks to months of adjusting stimulation parameters and engaging in rehabilitation.</p><h3>Key Aspects of Recovery:</h3><ul><li><h3>Rehabilitation Therapy</h3><p>Physical, occupational, and speech therapy are integral to recovery, helping patients regain strength, coordination, balance, and communication skills. These therapies are crucial for maximizing functional independence.</p></li><li><h3>Medication Management</h3><p>Ongoing optimization of medications is common, particularly for conditions like Parkinson's disease, requiring close monitoring by neurologists.</p></li><li><h3>Psychological Support</h3><p>Coping with a chronic movement disorder can be challenging. Psychological counseling and support groups are often recommended to address emotional well-being and aid adjustment.</p></li><li><h3>Lifestyle Modifications</h3><p>Adopting a healthy lifestyle, including regular exercise, a balanced diet, and adequate sleep, plays a vital role in long-term symptom management and overall health.</p></li><li><h3>Regular Follow-ups</h3><p>Consistent follow-up appointments with your neurologist and care team are essential for monitoring progress, adjusting treatments, and addressing any new concerns. DivinHeal facilitates these crucial follow-up connections, even after you return home.</p></li></ul>
Spinal Cord Stimulation
Treatment Price
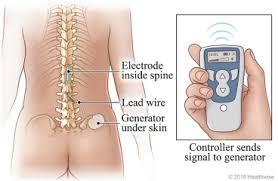
$12000.00 USDSpinal Cord Stimulation aims to alleviate chronic, intractable pain, especially neuropathic pain, by implanting a small device that delivers electrical impulses to the spinal cord. It's a reversible procedure that offers a significant improvement in quality of life for suitable patients after a successful trial period. DivinHeal connects you to world-class neurosurgeons and pain management specialists.
Spinal Cord Stimulation aims to alleviate chronic, intractable pain, especially neuropathic pain, by implanting a small device that delivers electrical impulses to the spinal cord. It's a reversible procedure that offers a significant improvement in quality of life for suitable patients after a successful trial period. DivinHeal connects you to world-class neurosurgeons and pain management specialists.
Treatment Overview
Spinal Cord Stimulation aims to alleviate chronic, intractable pain, especially neuropathic pain, by implanting a small device that delivers electrical impulses to the spinal cord. It's a reversible procedure that offers a significant improvement in quality of life for suitable patients after a successful trial period. DivinHeal connects you to world-class neurosurgeons and pain management specialists.
Procedures
The Spinal Cord Stimulation procedure involves two main stages: a trial period and permanent implantation. <h3>SCS Trial (Temporary Implant)</h3><p>This is a crucial diagnostic step. Under local anesthesia and often light sedation, the pain specialist inserts one or two thin, flexible leads (electrodes) into the epidural space near the spinal cord, typically through a needle. The leads are connected to an external stimulator worn on a belt. Patients go home with the trial stimulator for 5-7 days to evaluate its effectiveness in reducing pain during daily activities. If pain relief of 50% or more is achieved, the trial is considered successful, indicating a strong likelihood of long-term benefit from permanent implantation.</p><h3>Permanent SCS Implant</h3><p>If the trial is successful, the permanent system is implanted in a surgical procedure, usually under general anesthesia. The leads are carefully advanced into the epidural space and anchored to prevent migration. The neurostimulator (IPG), a small battery-powered device, is then implanted in a 'pocket' created under the skin, usually in the buttock or abdomen. The leads are tunneled under the skin and connected to the IPG. The incisions are closed, and the patient is typically monitored for a day or two. After implantation, the device is programmed wirelessly by the pain specialist to deliver optimal pain relief, with patients using a remote control to adjust settings as needed within prescribed parameters. Modern SCS devices offer various stimulation patterns, including tonic, burst, and high-frequency, tailored to individual patient needs.</p>
Benefits
<h2>Benefits of Spinal Cord Stimulation</h2><ul><li>Significant reduction in chronic neuropathic pain, often leading to improved quality of life and functionality.</li><li>Decreased reliance on oral pain medications, including opioids, reducing associated side effects and risks of dependency.</li><li>Improved ability to perform daily activities, engage in physical therapy, and return to work or hobbies.</li><li>The procedure is reversible; the device can be removed if desired without permanent changes to the spinal cord.</li><li>Adjustable therapy settings, allowing for personalized pain relief that can be fine-tuned over time.</li><li>Many patients experience improved sleep, mood, and overall well-being.</li><li>A successful trial period allows patients to experience the therapy's effectiveness before permanent implantation.</li></ul>
Recovery Information
<h2>Spinal Cord Stimulation Recovery Time and Tips</h2><h3>Immediate Post-Procedure</h3><p>After the permanent SCS implant, patients typically stay in the hospital for 1-2 days for monitoring and initial programming. There might be some soreness at the incision sites, managed with prescribed pain medication. During the temporary trial, patients are usually discharged the same day, with instructions for careful movement to prevent lead displacement.</p><h3>Long-Term Recovery and Rehabilitation</h3><ul><li><strong>Activity Restrictions:</strong> For 6-8 weeks post-implantation, patients are advised to avoid strenuous activities, heavy lifting, excessive twisting, or bending to allow the leads to anchor securely and prevent migration.</li><li><strong>Device Programming:</strong> Several follow-up appointments will be scheduled for fine-tuning the SCS device. The pain specialist will work closely with the patient to adjust stimulation settings to achieve optimal pain relief. This iterative process is key to long-term success.</li><li><strong>Physical Therapy:</strong> Often recommended to regain strength, flexibility, and function, complementing the pain relief provided by SCS. This helps integrate the reduced pain into improved mobility.</li><li><strong>Psychological Support:</strong> Chronic pain can have significant psychological impacts. Counseling or support groups can be beneficial in addressing the emotional aspects of living with chronic pain and adjusting to the SCS device.</li><li><strong>Long-Term Management:</strong> Regular follow-ups with the pain specialist are necessary to monitor the device, manage battery life, and address any changes in pain patterns or effectiveness. Battery replacement for non-rechargeable devices typically occurs every 5-10 years, while rechargeable systems require regular charging by the patient.</li><li><strong>Lifestyle Adjustments:</strong> Patients receive guidance on safely using their SCS device during everyday activities, including magnetic field precautions and device care.</li></ul>

neuromodulation therapy
Treatment Price
$8500.00 USDNeuromodulation Therapy Overview
What is Neuromodulation Therapy?
Neuromodulation therapy encompasses a range of medical devices and procedures designed to modulate nerve activity to restore function, reduce symptoms, or improve quality of life. These therapies involve implanting devices or using non-invasive techniques to deliver electrical impulses or pharmaceutical agents directly to nerve pathways.
Goals of Treatment
- Pain Management: Significantly reduce chronic neuropathic pain, back pain, and other intractable pain conditions.
- Movement Disorder Control: Manage symptoms of Parkinson's disease, essential tremor, and dystonia.
- Epilepsy Management: Decrease seizure frequency and severity in drug-resistant epilepsy.
- Other Applications: Treat conditions like urinary incontinence, obsessive-compulsive disorder (OCD), and depression.
Neuromodulation Therapy Overview
What is Neuromodulation Therapy?
Neuromodulation therapy encompasses a range of medical devices and procedures designed to modulate nerve activity to restore function, reduce symptoms, or improve quality of life. These therapies involve implanting devices or using non-invasive techniques to deliver electrical impulses or pharmaceutical agents directly to nerve pathways.
Goals of Treatment
- Pain Management: Significantly reduce chronic neuropathic pain, back pain, and other intractable pain conditions.
- Movement Disorder Control: Manage symptoms of Parkinson's disease, essential tremor, and dystonia.
- Epilepsy Management: Decrease seizure frequency and severity in drug-resistant epilepsy.
- Other Applications: Treat conditions like urinary incontinence, obsessive-compulsive disorder (OCD), and depression.
Treatment Overview
<h2>Neuromodulation Therapy Overview</h2><h3>What is Neuromodulation Therapy?</h3><p>Neuromodulation therapy encompasses a range of medical devices and procedures designed to modulate nerve activity to restore function, reduce symptoms, or improve quality of life. These therapies involve implanting devices or using non-invasive techniques to deliver electrical impulses or pharmaceutical agents directly to nerve pathways.</p><h3>Goals of Treatment</h3><ul><li><strong>Pain Management:</strong> Significantly reduce chronic neuropathic pain, back pain, and other intractable pain conditions.</li><li><strong>Movement Disorder Control:</strong> Manage symptoms of Parkinson's disease, essential tremor, and dystonia.</li><li><strong>Epilepsy Management:</strong> Decrease seizure frequency and severity in drug-resistant epilepsy.</li><li><strong>Other Applications:</strong> Treat conditions like urinary incontinence, obsessive-compulsive disorder (OCD), and depression.</li></ul>
Procedures
Neuromodulation therapy involves a detailed process tailored to the specific condition and patient needs. For invasive procedures like Deep Brain Stimulation (DBS) or Spinal Cord Stimulation (SCS), the general steps include: 1. **Pre-surgical Evaluation:** Comprehensive neurological and psychological assessments, detailed imaging (MRI, CT scans) to pinpoint target areas in the brain or spinal cord, and sometimes a temporary trial of stimulation for SCS to assess efficacy. 2. **Implantation of Leads/Electrodes:** Under local anesthesia and/or general anesthesia, small electrodes (leads) are precisely placed into the target brain region (for DBS) or epidural space near the spinal cord (for SCS). Intraoperative neurophysiological mapping or imaging guidance ensures accurate placement. For DBS, this may involve awake surgery to test symptom improvement. 3. **Implantation of Neurostimulator/IPG:** A small, battery-powered neurostimulator (Implantable Pulse Generator - IPG) is implanted, typically under the skin in the chest or abdomen. This device is connected to the leads via extension wires tunneled under the skin. 4. **Device Activation and Programming:** After surgical recovery, the neurostimulator is activated. A specialist uses an external programmer to adjust the stimulation parameters (e.g., amplitude, pulse width, frequency) to optimize symptom control with minimal side effects. This process often requires several programming sessions over weeks or months. Non-invasive neuromodulation, such as Transcranial Magnetic Stimulation (TMS), involves placing an electromagnetic coil against the scalp. The coil delivers magnetic pulses that painlessly stimulate nerve cells in a targeted area of the brain. Patients typically receive daily sessions over several weeks.
Benefits
<h2>Benefits of Neuromodulation Therapy</h2><p>Neuromodulation therapies offer life-changing benefits for patients who have exhausted other treatment options. The advantages extend beyond symptom control, significantly enhancing overall quality of life.</p><h3>Key Advantages of Neuromodulation</h3><ul><li><strong>Significant Symptom Reduction:</strong> Effective relief from chronic pain, reduction in tremor and rigidity for movement disorders, and decreased seizure frequency in epilepsy.</li><li><strong>Improved Quality of Life:</strong> Enhanced mobility, better sleep, reduced reliance on oral medications, and greater independence in daily activities.</li><li><strong>Targeted Therapy:</strong> Precise delivery of stimulation or medication to specific neural pathways, minimizing systemic side effects often associated with oral drugs.</li><li><strong>Reversible and Adjustable:</strong> Most neuromodulation devices can be turned off, removed, or adjusted externally, allowing for fine-tuning of therapy parameters to optimize outcomes over time.</li><li><strong>Long-term Relief:</strong> Provides sustained symptom control, offering a lasting solution for chronic conditions.</li><li><strong>Reduced Medication Burden:</strong> Often allows for a decrease in the dosage or number of oral medications, thereby reducing associated side effects.</li></ul>
Recovery Information
<h2>Neuromodulation Therapy Recovery Time and Tips</h2><p>The <a href="#section-recovery">neuromodulation therapy recovery time</a> varies depending on the type of procedure (invasive vs. non-invasive) and individual patient factors. DivinHeal provides comprehensive guidance to support your healing process.</p><h3>Recovery After Invasive Neuromodulation (e.g., DBS, SCS)</h3><ul><li><strong>Hospital Stay:</strong> Typically 2-5 days post-surgery for monitoring and initial device checks.</li><li><strong>Initial Recovery (1-2 weeks):</strong> Focus on incision care, pain management, and avoiding strenuous activities. Swelling or discomfort at the incision sites is normal.</li><li><strong>Device Programming (Weeks 2-6):</strong> Multiple follow-up visits are usually required for optimal programming of the neurostimulator to achieve the best therapeutic effect. This phase is crucial for personalized treatment.</li><li><strong>Full Recovery & Rehabilitation (3-6 months):</strong> Gradual return to normal activities. Physical therapy may be recommended to regain strength, flexibility, and coordination. Avoiding heavy lifting and impact sports during the initial months is advised.</li></ul><h3>Recovery After Non-Invasive Neuromodulation (e.g., TMS)</h3><ul><li><strong>Immediate Return to Activities:</strong> Patients can typically resume normal activities immediately after a session.</li><li><strong>Minimal Side Effects:</strong> Mild scalp discomfort or headaches are possible but usually resolve quickly.</li><li><strong>Course Duration:</strong> A series of daily treatments over several weeks is common for sustained benefits.</li></ul><h3>General Recovery Tips</h3><ul><li><strong>Follow Post-Operative Instructions:</strong> Adhere strictly to wound care, medication schedules, and activity restrictions.</li><li><strong>Stay Hydrated & Eat Well:</strong> Support healing with a healthy diet.</li><li><strong>Gentle Exercise:</strong> As advised by your medical team, incorporate light walking to promote circulation.</li><li><strong>Emotional Support:</strong> Seek counseling or join support groups, as adjusting to a new device or significant symptom change can be emotionally challenging.</li><li><strong>Regular Follow-ups:</strong> Essential for device monitoring, programming adjustments, and addressing any concerns.</li></ul>

laminectomy surgery
Treatment Price
$3500.00 USDLaminectomy aims to alleviate debilitating pain, numbness, or weakness caused by spinal cord or nerve root compression. By carefully removing a portion of the vertebral bone (lamina), surgeons create more space within the spinal canal, decompressing affected neural structures. This procedure is performed by highly skilled neurosurgeons or orthopedic spine surgeons, often using advanced imaging guidance for precision.
Laminectomy aims to alleviate debilitating pain, numbness, or weakness caused by spinal cord or nerve root compression. By carefully removing a portion of the vertebral bone (lamina), surgeons create more space within the spinal canal, decompressing affected neural structures. This procedure is performed by highly skilled neurosurgeons or orthopedic spine surgeons, often using advanced imaging guidance for precision.
Treatment Overview
Laminectomy aims to alleviate debilitating pain, numbness, or weakness caused by spinal cord or nerve root compression. By carefully removing a portion of the vertebral bone (lamina), surgeons create more space within the spinal canal, decompressing affected neural structures. This procedure is performed by highly skilled neurosurgeons or orthopedic spine surgeons, often using advanced imaging guidance for precision.
Procedures
Laminectomy surgery is typically performed under general anesthesia. The patient is usually positioned face down. The surgeon makes an incision along the midline of the back, over the affected vertebrae. The muscles are then carefully retracted to expose the bony structure of the spine. Using specialized instruments, the surgeon carefully removes part or all of the lamina from the vertebra. This creates an opening that relieves pressure on the spinal cord or nerve roots. Any bone spurs, thickened ligaments, or disc fragments that contribute to the compression are also removed. In some cases, if spinal instability is a concern after decompression, spinal fusion might be performed concurrently, though this is not always necessary for a standard laminectomy. After sufficient decompression is achieved, the muscles and tissues are repositioned, and the incision is closed with sutures or staples.
Benefits
<h2>Benefits of Laminectomy Surgery</h2><p>Laminectomy surgery offers significant advantages for individuals suffering from spinal cord or nerve compression:</p><ul><li><h4>Effective Pain Relief</h4><p>Substantial reduction or elimination of chronic back or neck pain, radiating pain (sciatica or radiculopathy), and leg/arm weakness or numbness caused by nerve compression.</p></li><li><h4>Improved Mobility and Function</h4><p>Restoration of normal neurological function, allowing patients to regain mobility, perform daily activities with greater ease, and return to an active lifestyle.</p></li><li><h4>Prevention of Further Neurological Damage</h4><p>Decompressing the spinal cord or nerves prevents progressive damage, which could otherwise lead to permanent weakness, paralysis, or bladder/bowel dysfunction.</p></li><li><h4>High Success Rates</h4><p>When performed for appropriate indications, laminectomy boasts high success rates in relieving symptoms and improving quality of life.</p></li><li><h4>Long-Term Solution</h4><p>For many patients, laminectomy provides a durable solution to spinal stenosis or disc-related nerve compression, offering lasting relief.</p></li></ul>
Recovery Information
<h2>Laminectomy Recovery Time and Tips</h2><p>Recovery from laminectomy surgery is a gradual process, but with proper care and adherence to post-operative guidelines, most patients achieve excellent outcomes. The typical <a href="#recovery">laminectomy surgery recovery time</a> varies based on the extent of the surgery, individual health, and commitment to rehabilitation.</p><ul><li><h4>Immediate Post-Operative Period (Hospital Stay: 2-5 days)</h4><p>Patients are encouraged to ambulate soon after surgery under nursing supervision. Pain management is crucial, and medications will be prescribed. Initial physical therapy may begin to teach safe movement.</p></li><li><h4>First Few Weeks (1-6 weeks post-surgery)</h4><p>Patients should avoid heavy lifting, twisting, or bending. Walking is encouraged, gradually increasing distance. Formal physical therapy usually starts to strengthen core muscles, improve flexibility, and restore proper posture. Driving may be restricted for several weeks.</p></li><li><h4>Long-Term Recovery (3-6 months and beyond)</h4><p>Full recovery can take several months. Continued adherence to physical therapy exercises is vital for long-term spinal health. Most patients can return to light activities or work within 2-6 weeks, with full return to strenuous activities potentially taking 3-6 months, depending on their occupation and progress.</p></li></ul><h3>Recovery Tips:</h3><ul><li><strong>Follow all post-operative instructions:</strong> This includes wound care, medication schedules, and activity restrictions.</li><li><strong>Engage in Physical Therapy:</strong> A tailored rehabilitation program is key to regaining strength and flexibility.</li><li><strong>Maintain a Healthy Lifestyle:</strong> Proper nutrition, hydration, and avoiding smoking can significantly aid healing.</li><li><strong>Listen to Your Body:</strong> Avoid activities that cause pain and gradually increase your activity level.</li><li><strong>Seek Emotional Support:</strong> Recovery can be challenging; connecting with family, friends, or support groups can be beneficial.</li></ul>

endoscopic brain surgery
Treatment Price
$12000.00 USDOverview of Endoscopic Brain Surgery
Minimally Invasive Neurosurgical Excellence
Endoscopic brain surgery represents a significant leap in neurosurgical care, allowing surgeons to navigate complex brain anatomy with precision and minimal disruption to surrounding healthy tissues. This advanced technique is ideal for treating various neurological conditions, from pituitary tumors and hydrocephalus to certain types of brain cysts and complex skull base lesions. At DivinHeal, we connect you with leading neurosurgical teams specializing in these state-of-the-art procedures, ensuring access to cutting-edge technology and compassionate care for optimal patient outcomes.
Overview of Endoscopic Brain Surgery
Minimally Invasive Neurosurgical Excellence
Endoscopic brain surgery represents a significant leap in neurosurgical care, allowing surgeons to navigate complex brain anatomy with precision and minimal disruption to surrounding healthy tissues. This advanced technique is ideal for treating various neurological conditions, from pituitary tumors and hydrocephalus to certain types of brain cysts and complex skull base lesions. At DivinHeal, we connect you with leading neurosurgical teams specializing in these state-of-the-art procedures, ensuring access to cutting-edge technology and compassionate care for optimal patient outcomes.
Treatment Overview
<h2>Overview of Endoscopic Brain Surgery</h2><h3>Minimally Invasive Neurosurgical Excellence</h3><p>Endoscopic brain surgery represents a significant leap in neurosurgical care, allowing surgeons to navigate complex brain anatomy with precision and minimal disruption to surrounding healthy tissues. This advanced technique is ideal for treating various neurological conditions, from pituitary tumors and hydrocephalus to certain types of brain cysts and complex skull base lesions. At DivinHeal, we connect you with leading neurosurgical teams specializing in these state-of-the-art procedures, ensuring access to cutting-edge technology and compassionate care for optimal patient outcomes.</p>
Procedures
Endoscopic brain surgery involves inserting a thin tube with a camera (endoscope) through a small incision in the skull or a natural opening like the nostril. The surgeon visualizes the brain's interior on a high-definition monitor. Specialized micro-instruments are then passed through the endoscope to perform the surgery, such as tumor removal, cyst drainage, or creating a new CSF pathway. The procedure is guided by real-time navigation systems for extreme precision, minimizing damage to surrounding healthy brain tissue.
Benefits
<h2>Benefits of Endoscopic Brain Surgery</h2><ul><li><h3>Minimally Invasive Approach</h3><p>Smaller incisions lead to reduced scarring, less tissue trauma, and decreased risk of infection compared to traditional open surgery.</p></li><li><h3>Faster Recovery Times</h3><p>Patients typically experience shorter hospital stays and a quicker return to daily activities, improving overall quality of life post-surgery.</p></li><li><h3>Enhanced Precision and Visualization</h3><p>The endoscope provides magnified, high-definition views of the surgical field, allowing neurosurgeons to operate with greater accuracy and minimize damage to healthy brain tissue.</p></li><li><h3>Reduced Pain and Discomfort</h3><p>Less invasive techniques generally result in less post-operative pain, requiring fewer strong analgesics.</p></li><li><h3>Improved Cosmetic Outcomes</h3><p>With smaller or hidden incisions (e.g., through the nostril), the cosmetic impact of the surgery is significantly reduced.</p></li><li><h3>Lower Risk of Complications</h3><p>Minimally invasive approaches are often associated with a lower incidence of certain surgical complications.</p></li></ul>
Recovery Information
<h2>Endoscopic Brain Surgery Recovery Time and Tips</h2><h3>A Smooth Path to Healing</h3><p>Recovery after endoscopic brain surgery is generally faster and less challenging than traditional open brain surgery. Most patients can expect a hospital stay of 3-7 days, depending on the complexity of the procedure and individual recovery progress. The initial recovery phase focuses on managing any discomfort, monitoring neurological function, and gradually increasing mobility.</p><h3>Key Aspects of Recovery:</h3><ul><li><b>Hospital Stay:</b> Typically 3-7 days for observation, pain management, and early mobilization.</li><li><b>Pain Management:</b> Mild to moderate pain or headache is common and managed with medication.</li><li><b>Activity Restrictions:</b> Avoid strenuous activities, heavy lifting, and sudden head movements for several weeks. Gradual return to light activities is encouraged.</li><li><b>Wound Care:</b> Keep incision sites clean and dry. Follow specific instructions for any nasal packing or external dressings.</li><li><b>Follow-up Care:</b> Regular follow-up appointments with your neurosurgeon are crucial to monitor healing and assess long-term outcomes. Imaging scans may be repeated.</li><li><b>Rehabilitation:</b> Depending on the condition treated and any neurological deficits, physical therapy, occupational therapy, or speech therapy may be recommended.</li><li><b>Emotional Support:</b> It's normal to experience emotional changes. DivinHeal can connect you with support resources and counseling to aid your mental well-being during recovery.</li></ul><p>Full recovery, including a return to all normal activities, can take anywhere from a few weeks to a few months. Adhering strictly to your medical team's advice is paramount for optimal healing and the best possible outcome.</p>

Peripheral Nerve Surgery (Carpal Tunnel / Ulnar Nerve)
Treatment Price
$1500.00 USDGoals of Peripheral Nerve Surgery
The primary goal of Peripheral Nerve Surgery is to alleviate symptoms caused by nerve compression, such as chronic pain, numbness, and muscle weakness, and to prevent further nerve damage. Techniques involve precisely releasing structures that are pressing on the nerve, such as ligaments or scar tissue, allowing the nerve to heal and function properly. These surgeries are typically performed on an outpatient basis or with a short hospital stay, utilizing either open incision or minimally invasive endoscopic methods.
Goals of Peripheral Nerve Surgery
The primary goal of Peripheral Nerve Surgery is to alleviate symptoms caused by nerve compression, such as chronic pain, numbness, and muscle weakness, and to prevent further nerve damage. Techniques involve precisely releasing structures that are pressing on the nerve, such as ligaments or scar tissue, allowing the nerve to heal and function properly. These surgeries are typically performed on an outpatient basis or with a short hospital stay, utilizing either open incision or minimally invasive endoscopic methods.
Treatment Overview
<h2>Goals of Peripheral Nerve Surgery</h2><p>The primary goal of Peripheral Nerve Surgery is to alleviate symptoms caused by nerve compression, such as chronic pain, numbness, and muscle weakness, and to prevent further nerve damage. Techniques involve precisely releasing structures that are pressing on the nerve, such as ligaments or scar tissue, allowing the nerve to heal and function properly. These surgeries are typically performed on an outpatient basis or with a short hospital stay, utilizing either open incision or minimally invasive endoscopic methods.</p>
Procedures
<h3>How Peripheral Nerve Surgery is Performed</h3><p><strong>General Steps for Carpal Tunnel Release:</strong></p><ol><li><strong>Anesthesia:</strong> Local anesthesia is typically used, often with sedation, meaning you'll be awake but relaxed and pain-free.</li><li><strong>Incision:</strong> In open surgery, a small incision (about 1-2 inches) is made in the palm of the hand. For endoscopic surgery, one or two smaller incisions (less than half an inch) are made in the wrist or palm.</li><li><strong>Ligament Division:</strong> The surgeon carefully cuts the transverse carpal ligament, which forms the roof of the carpal tunnel. This releases pressure on the median nerve.</li><li><strong>Closure:</strong> The skin incision(s) are closed with sutures or surgical tape, and a sterile dressing is applied.</li></ol><p><strong>General Steps for Ulnar Nerve Decompression:</strong></p><ol><li><strong>Anesthesia:</strong> Regional or general anesthesia may be used, depending on the complexity and patient preference.</li><li><strong>Incision:</strong> An incision is made on the inner side of the elbow over the cubital tunnel.</li><li><strong>Nerve Decompression:</strong> The surgeon identifies the ulnar nerve and carefully releases any compressing structures (e.g., thickened ligament, bone spurs).</li><li><strong>Optional Transposition:</strong> In some cases, the ulnar nerve may be moved from behind the bony prominence (medial epicondyle) to the front to prevent further compression or stretching. This is called anterior transposition.</li><li><strong>Closure:</strong> The incision is closed with sutures, and a dressing is applied.</li></ol><p>Both procedures aim to provide ample space for the nerve to heal and function without obstruction.</p>
Benefits
<h2>Benefits of Peripheral Nerve Surgery (Carpal Tunnel / Ulnar Nerve)</h2><ul><li><h3>Significant Pain Relief</h3><p>Patients often experience substantial reduction or complete elimination of pain, numbness, and tingling sensations shortly after surgery.</p></li><li><h3>Restoration of Nerve Function</h3><p>The surgery aims to relieve nerve compression, allowing the nerve to heal and restore normal sensation and muscle strength in the affected hand or arm.</p></li><li><h3>Improved Quality of Life</h3><p>By alleviating debilitating symptoms, patients can return to daily activities, work, and hobbies without discomfort, significantly enhancing their overall quality of life.</p></li><li><h3>Prevention of Further Nerve Damage</h3><p>Timely surgical intervention can prevent irreversible nerve damage and progressive muscle weakness that can result from prolonged compression.</p></li><li><h3>High Success Rates</h3><p>Both Carpal Tunnel Release and Ulnar Nerve Decompression procedures boast high success rates when performed by experienced surgeons.</p></li></ul>
Recovery Information
<h2>Recovery After Peripheral Nerve Surgery (Carpal Tunnel / Ulnar Nerve)</h2><h3>Immediate Post-Operative Period</h3><p>Immediately after surgery, your hand or arm will be bandaged, and you may experience some soreness. Pain medication will be prescribed to manage discomfort. You'll typically be discharged the same day or within 24 hours.</p><h3>First Few Weeks</h3><p>During the first week, it's crucial to keep the surgical site clean and dry. Light hand and wrist movements may be encouraged to prevent stiffness, but heavy lifting and strenuous activities should be avoided. Swelling and bruising are common and will gradually subside.</p><h3>Rehabilitation and Long-Term Wellness</h3><p>Full recovery for Carpal Tunnel Release typically takes 4-6 weeks, while Ulnar Nerve Decompression may take a bit longer, from 6 weeks to several months, especially if nerve damage was significant. Physical therapy, including nerve gliding exercises and strengthening, is often recommended to optimize recovery and restore full function. DivinHeal assists in coordinating these rehabilitation services, ensuring a smooth transition back to your normal activities. Adhering to your surgeon's advice and rehabilitation program is key for a successful long-term outcome.</p>

skull base surgery
Treatment Price
$12000.00 USDOverview of Skull Base Surgery
Addressing Complex Neurological Conditions
Skull base surgery aims to remove tumors, treat vascular abnormalities, repair cerebrospinal fluid (CSF) leaks, or alleviate compression on critical neurological structures located at the skull base. Due to the proximity to the brain and major nerves, these procedures require exceptional precision and a multidisciplinary team approach. Techniques range from traditional open surgery to advanced endoscopic and minimally invasive approaches, allowing surgeons to access deep-seated lesions with less disruption to surrounding healthy tissues. The primary goal is to achieve maximal resection of pathological tissue while ensuring the best possible functional outcomes and quality of life for the patient.
Overview of Skull Base Surgery
Addressing Complex Neurological Conditions
Skull base surgery aims to remove tumors, treat vascular abnormalities, repair cerebrospinal fluid (CSF) leaks, or alleviate compression on critical neurological structures located at the skull base. Due to the proximity to the brain and major nerves, these procedures require exceptional precision and a multidisciplinary team approach. Techniques range from traditional open surgery to advanced endoscopic and minimally invasive approaches, allowing surgeons to access deep-seated lesions with less disruption to surrounding healthy tissues. The primary goal is to achieve maximal resection of pathological tissue while ensuring the best possible functional outcomes and quality of life for the patient.
Treatment Overview
<h2>Overview of Skull Base Surgery</h2><h3>Addressing Complex Neurological Conditions</h3><p>Skull base surgery aims to remove tumors, treat vascular abnormalities, repair cerebrospinal fluid (CSF) leaks, or alleviate compression on critical neurological structures located at the skull base. Due to the proximity to the brain and major nerves, these procedures require exceptional precision and a multidisciplinary team approach. Techniques range from traditional open surgery to advanced endoscopic and minimally invasive approaches, allowing surgeons to access deep-seated lesions with less disruption to surrounding healthy tissues. The primary goal is to achieve maximal resection of pathological tissue while ensuring the best possible functional outcomes and quality of life for the patient.</p>
Procedures
Skull base surgery is an intricate procedure performed by a highly specialized surgical team, often involving neurosurgeons and ENT surgeons. The specific steps vary significantly based on the location and nature of the pathology. Generally, it involves: 1. Pre-operative Planning: Extensive imaging (MRI, CT, angiography) and navigation systems are used to map the exact location of the lesion and plan the most appropriate surgical approach (e.g., transnasal, transoral, transcranial, or transorbital). 2. Anesthesia: General anesthesia is administered, and the patient's vital signs and neurological functions are continuously monitored throughout the surgery. 3. Incision and Access: Depending on the chosen approach, an incision may be made externally (e.g., behind the ear, in the scalp, or a craniotomy) or access may be gained through natural orifices using endoscopic instruments (e.g., through the nose for pituitary tumors or clival chordomas). 4. Tumor Resection/Repair: Using microsurgical techniques, endoscopes, and specialized instruments, the surgeon carefully navigates through the delicate skull base structures to remove the tumor, repair a CSF leak, or address other pathologies. Intraoperative neuromonitoring is often used to protect critical nerves. 5. Reconstruction: After the lesion is addressed, the surgical site is meticulously reconstructed, often using grafts of tissue (e.g., fascia, fat, or synthetic materials) to seal defects and prevent complications like CSF leaks. 6. Closure: Incisions are closed, and dressings are applied. The patient is then transferred to a recovery unit for close monitoring.
Benefits
<h2>Benefits of Skull Base Surgery</h2><h3>Hope for Improved Health and Quality of Life</h3><ul><li><h3>Tumor Eradication or Reduction:</h3><p>Effective removal of benign or malignant tumors, leading to significant symptom relief and improved prognosis.</p></li><li><h3>Preservation of Neurological Function:</h3><p>Advanced techniques and intraoperative monitoring aim to protect critical nerves and brain structures, minimizing the risk of neurological deficits.</p></li><li><h3>Relief from Debilitating Symptoms:</h3><p>Alleviation of symptoms such as headaches, facial pain, vision or hearing impairment, and balance issues caused by compression or structural abnormalities.</p></li><li><h3>Repair of Defects:</h3><p>Successful repair of CSF leaks prevents serious complications like meningitis and restores normal brain fluid dynamics.</p></li><li><h3>Improved Quality of Life:</h3><p>By addressing the underlying pathology, patients often experience a significant improvement in their overall health, daily functioning, and long-term well-being.</p></li><li><h3>Access to Innovative Techniques:</h3><p>With DivinHeal, patients gain access to hospitals employing cutting-edge endoscopic and minimally invasive approaches, often leading to faster recovery and fewer complications.</p></li></ul>
Recovery Information
<h2>Recovery and Life After Skull Base Surgery</h2><h3>A Guided Path to Wellness</h3><p>Recovery from skull base surgery is a gradual process that varies significantly based on the type of surgery, the patient's overall health, and the extent of the condition treated. DivinHeal provides comprehensive guidance and support throughout your recovery journey.</p><ul><li><h3>Immediate Post-operative Period (Hospital Stay):</h3><p>Patients typically remain in the hospital for 5 to 10 days. Initial recovery focuses on pain management, monitoring for complications like CSF leaks or infections, and early mobilization. Neurological assessments are performed regularly.</p></li><li><h3>First Few Weeks Post-Discharge:</h3><p>Upon discharge, patients may experience fatigue, headaches, dizziness, or temporary changes in taste or smell. Physical therapy, occupational therapy, or speech therapy may be recommended to regain strength, balance, and function. Strenuous activities should be avoided.</p></li><li><h3>Long-Term Recovery (Months):</h3><p>Full recovery can take several weeks to many months. Regular follow-up appointments with the surgical team are crucial to monitor healing, assess neurological status, and plan for any further treatments like radiation or chemotherapy if indicated. Lifestyle modifications, including adequate rest, a healthy diet, and avoiding heavy lifting, are important.</p></li><li><h3>Emotional and Psychological Support:</h3><p>Dealing with a complex surgery and recovery can be challenging. DivinHeal can connect patients with resources for emotional counseling and support groups, fostering mental well-being alongside physical healing. Our dedicated care coordinators ensure continuous support and answer all your questions during this critical phase, aiming for optimal skull base surgery recovery time and tips to enhance your healing.</p></li></ul>

parkinson disease treatment
Treatment Price
$8000.00 USDTreatment for Parkinson's disease focuses on symptom control, slowing disease progression, and enhancing daily function. This includes pharmacotherapy (medications), advanced therapies like Deep Brain Stimulation (DBS), and supportive therapies such as physical, occupational, and speech therapy. DivinHeal connects you to world-class neurologists and neurosurgeons specializing in personalized Parkinson's care.
Treatment for Parkinson's disease focuses on symptom control, slowing disease progression, and enhancing daily function. This includes pharmacotherapy (medications), advanced therapies like Deep Brain Stimulation (DBS), and supportive therapies such as physical, occupational, and speech therapy. DivinHeal connects you to world-class neurologists and neurosurgeons specializing in personalized Parkinson's care.
Treatment Overview
<p>Treatment for Parkinson's disease focuses on symptom control, slowing disease progression, and enhancing daily function. This includes pharmacotherapy (medications), advanced therapies like Deep Brain Stimulation (DBS), and supportive therapies such as physical, occupational, and speech therapy. DivinHeal connects you to world-class neurologists and neurosurgeons specializing in personalized Parkinson's care.</p>
Procedures
Parkinson disease treatment is highly individualized. Pharmacological treatment involves regular oral medication, often starting with Levodopa, adjusted by a neurologist based on symptom severity and progression. Deep Brain Stimulation (DBS) is a surgical procedure: first, precise brain mapping is performed to identify target areas (e.g., subthalamic nucleus or globus pallidus internus). Electrodes are then stereotactically implanted and connected to an impulse generator (neurostimulator) placed under the skin in the chest, similar to a pacemaker. Post-surgery, the device is programmed and adjusted to deliver continuous electrical stimulation to alleviate motor symptoms.
Benefits
<p>The primary benefits of effective Parkinson disease treatment include significant symptom reduction, improved motor function (reducing tremor, rigidity, and bradykinesia), enhanced mobility and balance, and a substantial improvement in the overall quality of life. For suitable candidates, Deep Brain Stimulation (DBS) can dramatically reduce the need for high doses of medication, decrease dyskinesias, and provide more stable symptom control, leading to greater independence and participation in daily activities.</p>
Recovery Information
<p>Recovery from Parkinson disease treatment varies depending on the modality. For medication-based management, 'recovery' is an ongoing process of symptom control, with adjustments based on patient response. For Deep Brain Stimulation (DBS) surgery, initial hospital stay is typically 3-7 days. Full recovery and optimization of stimulation settings can take several weeks to months. Post-operative care involves regular follow-ups, medication adjustments, and ongoing physical, occupational, and speech therapy to maximize functional gains and adapt to new motor control. DivinHeal provides support for rehabilitation planning and follow-up care.</p>

stroke treatment
Treatment Price
$3500.00 USDA stroke is a medical emergency requiring immediate diagnosis and treatment to reduce brain injury and potential disability. Our approach involves rapid assessment to identify the type of stroke (ischemic or hemorrhagic), followed by swift, targeted interventions such as clot dissolution, surgical repair, or management of intracranial pressure. DivinHeal connects you with leading neurologists and advanced facilities for comprehensive stroke care, from acute management to long-term rehabilitation.
A stroke is a medical emergency requiring immediate diagnosis and treatment to reduce brain injury and potential disability. Our approach involves rapid assessment to identify the type of stroke (ischemic or hemorrhagic), followed by swift, targeted interventions such as clot dissolution, surgical repair, or management of intracranial pressure. DivinHeal connects you with leading neurologists and advanced facilities for comprehensive stroke care, from acute management to long-term rehabilitation.
Treatment Overview
A stroke is a medical emergency requiring immediate diagnosis and treatment to reduce brain injury and potential disability. Our approach involves rapid assessment to identify the type of stroke (ischemic or hemorrhagic), followed by swift, targeted interventions such as clot dissolution, surgical repair, or management of intracranial pressure. DivinHeal connects you with leading neurologists and advanced facilities for comprehensive stroke care, from acute management to long-term rehabilitation.
Procedures
Stroke treatment requires immediate medical attention. For ischemic stroke (clot), intravenous thrombolysis (e.g., tPA) is administered within 3-4.5 hours of symptom onset to dissolve the clot. For large vessel occlusions, mechanical thrombectomy, a surgical procedure to remove the clot using a catheter, may be performed up to 24 hours later. For hemorrhagic stroke (bleeding), treatment focuses on controlling bleeding and reducing intracranial pressure. This can involve surgical clipping or coiling of aneurysms, hematoma evacuation, or external ventricular drain placement. Post-procedure, patients are monitored in an ICU, vital signs are stabilized, and early rehabilitation is initiated to restore function and prevent complications.
Benefits
<h2>Key Benefits of Timely and Comprehensive Stroke Treatment</h2><ul><li><h3>Life-Saving Intervention</h3><p>Immediate treatment can dissolve clots or stop bleeding, preventing further brain damage and significantly increasing survival rates.</p></li><li><h3>Minimizing Disability</h3><p>Early and appropriate treatment, followed by intensive rehabilitation, can help restore lost functions, reduce long-term disability, and improve quality of life.</p></li><li><h3>Enhanced Functional Recovery</h3><p>With dedicated physical, occupational, and speech therapy, many patients regain independence in daily activities, mobility, and communication.</p></li><li><h3>Prevention of Recurrence</h3><p>Comprehensive stroke care includes identifying and managing risk factors, significantly lowering the chance of future stroke episodes.</p></li><li><h3>Improved Quality of Life</h3><p>By addressing physical, cognitive, and emotional challenges, treatment helps patients and their families adapt and lead fulfilling lives post-stroke.</p></li></ul>
Recovery Information
<h2>Stroke Recovery Time and Process Details</h2><p>Stroke recovery is a highly individualized and often lengthy journey, varying significantly based on the stroke's severity, location, the patient's age, and overall health. While the most rapid recovery often occurs in the first few months, improvements can continue for years.</p><h3>Immediate Post-Stroke Recovery (Hospital Stay)</h3><ul><li><strong>Acute Stabilization:</strong> The initial focus is on stabilizing vital signs, preventing complications like pneumonia or blood clots, and managing brain swelling. This typically lasts a few days to a week.</li><li><strong>Early Rehabilitation:</strong> As soon as the patient is stable, early mobilization and basic therapies begin, often within 24-48 hours.</li></ul><h3>Inpatient or Outpatient Rehabilitation</h3><ul><li><strong>Intensive Therapy:</strong> This phase can last weeks to months, involving a dedicated team of physical therapists (for movement and balance), occupational therapists (for daily activities), and speech-language pathologists (for communication and swallowing).</li><li><strong>Psychological Support:</strong> Many stroke survivors experience depression or anxiety; counseling and support groups are crucial for emotional well-being.</li></ul><h3>Long-Term Recovery and Lifestyle</h3><ul><li><strong>Ongoing Therapy:</strong> Recovery doesn't end after discharge. Continuous outpatient therapy, home exercise programs, and adaptive strategies are essential.</li><li><strong>Lifestyle Modifications:</strong> Adopting a healthy diet, regular exercise, quitting smoking, and managing chronic conditions (like hypertension or diabetes) are vital for preventing future strokes.</li><li><strong>Medication Adherence:</strong> Strict adherence to prescribed medications (e.g., blood thinners, blood pressure medication) is critical for long-term prevention.</li></ul><p>DivinHeal provides comprehensive support throughout this journey, connecting patients with leading rehabilitation centers and offering guidance for a sustained recovery.</p>

endoscopic third ventriculostomy
Treatment Price
$3500.00 USDEndoscopic Third Ventriculostomy (ETV) aims to restore the natural flow of cerebrospinal fluid (CSF) in patients suffering from obstructive hydrocephalus. Utilizing a neuro-endoscope, a small hole is precisely created in the floor of the third ventricle, diverting CSF directly into the subarachnoid space where it can be absorbed. This advanced technique often allows patients to avoid lifelong shunt dependency, offering a potentially curative solution with fewer risks compared to traditional shunt surgery. DivinHeal connects you to world-class neurosurgical facilities in India specializing in this delicate procedure.
Endoscopic Third Ventriculostomy (ETV) aims to restore the natural flow of cerebrospinal fluid (CSF) in patients suffering from obstructive hydrocephalus. Utilizing a neuro-endoscope, a small hole is precisely created in the floor of the third ventricle, diverting CSF directly into the subarachnoid space where it can be absorbed. This advanced technique often allows patients to avoid lifelong shunt dependency, offering a potentially curative solution with fewer risks compared to traditional shunt surgery. DivinHeal connects you to world-class neurosurgical facilities in India specializing in this delicate procedure.
Treatment Overview
Endoscopic Third Ventriculostomy (ETV) aims to restore the natural flow of cerebrospinal fluid (CSF) in patients suffering from obstructive hydrocephalus. Utilizing a neuro-endoscope, a small hole is precisely created in the floor of the third ventricle, diverting CSF directly into the subarachnoid space where it can be absorbed. This advanced technique often allows patients to avoid lifelong shunt dependency, offering a potentially curative solution with fewer risks compared to traditional shunt surgery. DivinHeal connects you to world-class neurosurgical facilities in India specializing in this delicate procedure.
Procedures
The endoscopic third ventriculostomy (ETV) procedure begins with the patient under general anesthesia. A small incision is made on the scalp, typically just behind the hairline. A burr hole, about the size of a dime, is created in the skull. A thin, flexible endoscope, equipped with a high-resolution camera and tiny working channels, is gently inserted through the burr hole and navigated through the brain's natural pathways into the ventricular system, specifically reaching the third ventricle. Once the endoscope is positioned in the third ventricle, the surgeon identifies the floor of the ventricle and, using specialized micro-instruments passed through the endoscope, creates a small opening (stoma) in the thin membrane. This opening provides a bypass for the blocked cerebrospinal fluid (CSF), allowing it to drain into the subarachnoid space around the brain, where it can be absorbed. The endoscope is then carefully withdrawn, the burr hole is covered, and the scalp incision is closed. The entire procedure typically takes 1-2 hours.
Benefits
<h2>Benefits of Endoscopic Third Ventriculostomy (ETV)</h2><ul><li><h3>Avoids Shunt Dependence</h3><p>One of the primary advantages of ETV is the potential to avoid a permanent ventriculoperitoneal (VP) shunt, eliminating risks associated with shunt malfunction, infection, and revision surgeries.</p></li><li><h3>Minimally Invasive</h3><p>ETV is performed through a small incision and burr hole, leading to less pain, smaller scars, and generally faster recovery compared to open surgery.</p></li><li><h3>Reduced Infection Risk</h3><p>Without a foreign body (shunt) implanted, the long-term risk of infection is significantly lower than with shunt surgery.</p></li><li><h3>Potentially Curative</h3><p>For appropriate candidates, ETV can offer a durable solution for hydrocephalus by restoring a more physiological CSF pathway.</p></li><li><h3>Improved Quality of Life</h3><p>Successfully treated patients often experience significant symptom relief, improved neurological function, and a better overall quality of life.</p></li></ul>
Recovery Information
<h2>Endoscopic Third Ventriculostomy Recovery Time and Tips</h2><ul><li><h3>Immediate Post-Operative Period (Hospital Stay)</h3><p>After ETV, patients typically stay in the hospital for 2-4 days. Monitoring for intracranial pressure, neurological status, and pain management are key. Most patients can usually resume light activities within 24-48 hours post-surgery.</p></li><li><h3>First Few Weeks (At Home)</h3><p>Patients are advised to avoid strenuous activities, heavy lifting, and bending for the first 2-4 weeks. Mild headaches, nausea, or dizziness are common but usually subside. Follow-up appointments with your neurosurgeon are crucial to monitor recovery and CSF flow.</p></li><li><h3>Long-Term Recovery & Wellness</h3><p>Full recovery, including a return to normal activities like work or school, typically takes 4-6 weeks. Maintaining a healthy lifestyle, avoiding head trauma, and attending all scheduled follow-up checks are important. Some patients may benefit from rehabilitation therapy if any neurological deficits were present pre-operatively. DivinHeal offers support for coordinating long-term follow-up and access to rehabilitation services.</p></li></ul>

hydrocephalus surgery
Treatment Price
$7000.00 USDUnderstanding Hydrocephalus Surgery
Hydrocephalus, often referred to as 'water on the brain,' is a serious condition characterized by an abnormal accumulation of cerebrospinal fluid (CSF) within the brain's ventricles. This buildup can exert harmful pressure on brain tissues, leading to a range of neurological impairments if left untreated.
The primary goal of hydrocephalus surgery is to divert or reduce the excess CSF, thereby normalizing intracranial pressure and protecting brain function. This is typically achieved through procedures like the implantation of a shunt system or an Endoscopic Third Ventriculostomy (ETV), tailored to the specific type and cause of hydrocephalus. DivinHeal connects you with top neurosurgery centers globally, ensuring access to cutting-edge techniques and compassionate care for effective hydrocephalus treatment.
Understanding Hydrocephalus Surgery
Hydrocephalus, often referred to as 'water on the brain,' is a serious condition characterized by an abnormal accumulation of cerebrospinal fluid (CSF) within the brain's ventricles. This buildup can exert harmful pressure on brain tissues, leading to a range of neurological impairments if left untreated.
The primary goal of hydrocephalus surgery is to divert or reduce the excess CSF, thereby normalizing intracranial pressure and protecting brain function. This is typically achieved through procedures like the implantation of a shunt system or an Endoscopic Third Ventriculostomy (ETV), tailored to the specific type and cause of hydrocephalus. DivinHeal connects you with top neurosurgery centers globally, ensuring access to cutting-edge techniques and compassionate care for effective hydrocephalus treatment.
Treatment Overview
<h2 id="overview">Understanding Hydrocephalus Surgery</h2><p>Hydrocephalus, often referred to as 'water on the brain,' is a serious condition characterized by an abnormal accumulation of cerebrospinal fluid (CSF) within the brain's ventricles. This buildup can exert harmful pressure on brain tissues, leading to a range of neurological impairments if left untreated.</p><p>The primary goal of hydrocephalus surgery is to divert or reduce the excess CSF, thereby normalizing intracranial pressure and protecting brain function. This is typically achieved through procedures like the implantation of a shunt system or an Endoscopic Third Ventriculostomy (ETV), tailored to the specific type and cause of hydrocephalus. DivinHeal connects you with top neurosurgery centers globally, ensuring access to cutting-edge techniques and compassionate care for effective hydrocephalus treatment.</p>
Procedures
Hydrocephalus surgery primarily involves either the insertion of a shunt system or an Endoscopic Third Ventriculostomy (ETV). For shunt insertion, the patient is placed under general anesthesia. A small incision is made on the scalp, and a small hole (burr hole) is created in the skull. A thin, flexible catheter (ventricular catheter) is carefully guided into one of the brain's ventricles. Another small incision is made, usually behind the ear, where a one-way valve is secured under the skin. A second catheter (distal catheter) is then tunnelled under the skin down to another part of the body, most commonly the abdominal cavity (ventriculoperitoneal or VP shunt), but sometimes to the heart (ventriculoatrial or VA shunt) or lung cavity (ventriculopleural shunt). The valve regulates the flow of excess cerebrospinal fluid (CSF) from the brain, diverting it to where it can be absorbed by the body. For ETV, a small incision is made on the scalp, and a burr hole is created. A specialized endoscope, equipped with a camera and light, is inserted through the burr hole and guided into the brain's ventricular system. The neurosurgeon uses the endoscope to visualize the floor of the third ventricle and create a tiny opening, allowing CSF to bypass any obstruction and flow into the surrounding subarachnoid space for natural absorption. Both procedures aim to reduce intracranial pressure and restore normal CSF dynamics.
Benefits
<h2 id="benefits">Benefits of Hydrocephalus Surgery</h2><ul><li><h3>Symptom Relief and Improved Quality of Life</h3><p>Successfully treated hydrocephalus significantly alleviates symptoms such as headaches, nausea, vision problems, balance issues, and cognitive decline, leading to a profound improvement in the patient's overall quality of life and functional independence.</p></li><li><h3>Prevention of Brain Damage</h3><p>By normalizing intracranial pressure, surgery prevents further pressure-induced damage to delicate brain tissues, which is crucial for preserving cognitive function and neurological health.</p></li><li><h3>Restored Normal Development (in children)</h3><p>For infants and young children, timely hydrocephalus surgery can prevent developmental delays and allow for more normal brain growth and cognitive development.</p></li><li><h3>Reduced Risk of Complications</h3><p>Effective CSF management reduces the long-term risks associated with untreated hydrocephalus, such as severe neurological deficits, seizures, and other life-threatening complications.</p></li><li><h3>Enhanced Cognitive Function</h3><p>Many patients experience improvements in memory, concentration, and other cognitive abilities post-surgery, especially in cases of NPH where cognitive decline is a prominent symptom.</p></li><li><h3>Mobility Improvement (for NPH)</h3><p>Patients with Normal Pressure Hydrocephalus often experience significant improvement in gait disturbances and balance after shunt insertion, restoring mobility and reducing fall risk.</p></li></ul>
Recovery Information
<h2 id="recovery-process">Hydrocephalus Surgery Recovery Time and Tips</h2><ul><li><h3>Immediate Post-Operative Period (Hospital Stay)</h3><p>After hydrocephalus surgery, patients typically remain in the hospital for 3 to 7 days. During this time, pain management is provided, and close monitoring for any signs of complications like infection or shunt malfunction is paramount. Early mobilization is encouraged under medical supervision.</p></li><li><h3>Initial Home Recovery (First Few Weeks)</h3><p>The <a href="hydrocephalus-surgery-recovery-time-and-tips">hydrocephalus surgery recovery time and tips</a> for home often involve avoiding strenuous activities, heavy lifting, and contact sports for several weeks to allow incision sites to heal and prevent strain on the shunt system. Headaches and fatigue are common and usually subside gradually.</p></li><li><h3>Long-Term Follow-up</h3><p>Regular follow-up appointments with the neurosurgeon are crucial. These appointments involve checking shunt function, reviewing imaging scans, and making any necessary adjustments to shunt programming. Lifelong monitoring of the shunt system is generally required.</p></li><li><h3>Potential for Rehabilitation</h3><p>Depending on the pre-existing neurological deficits, some patients may benefit from physical therapy, occupational therapy, or cognitive rehabilitation to regain strength, coordination, and improve cognitive function.</p></li><li><h3>Recognizing Shunt Malfunction or Infection</h3><p>Patients and caregivers must be educated on the signs of shunt malfunction (e.g., return of hydrocephalus symptoms, worsening headaches, nausea, lethargy) or infection (fever, redness/swelling along shunt tract) and instructed to seek immediate medical attention if these occur.</p></li><li><h3>Lifestyle Adjustments</h3><p>Most individuals with a shunt can lead normal, active lives. However, certain precautions, such as protecting the head from injury and informing medical personnel about the shunt during future procedures, are advised. DivinHeal provides comprehensive guidance for managing life with a shunt, ensuring continued well-being.</p></li></ul>

epilepsy surgery
Treatment Price
$5000.00 USDOverview of Epilepsy Surgery Treatment
A Path to Seizure Freedom
Epilepsy surgery is a highly specialized neurosurgical intervention designed for individuals with drug-resistant epilepsy, where seizures persist despite optimal trials of anti-epileptic medications. The primary goal is to precisely locate and remove or disconnect the brain region (seizure focus) responsible for generating epileptic seizures. This advanced treatment aims to significantly reduce seizure frequency and intensity, or even achieve complete seizure freedom, thereby dramatically improving the patient's quality of life.
Techniques range from resective surgeries, where a portion of the brain is removed, to disconnective procedures, and neuromodulation techniques such as Vagus Nerve Stimulation (VNS) or Deep Brain Stimulation (DBS), for cases where resection is not feasible or appropriate.
Overview of Epilepsy Surgery Treatment
A Path to Seizure Freedom
Epilepsy surgery is a highly specialized neurosurgical intervention designed for individuals with drug-resistant epilepsy, where seizures persist despite optimal trials of anti-epileptic medications. The primary goal is to precisely locate and remove or disconnect the brain region (seizure focus) responsible for generating epileptic seizures. This advanced treatment aims to significantly reduce seizure frequency and intensity, or even achieve complete seizure freedom, thereby dramatically improving the patient's quality of life.
Techniques range from resective surgeries, where a portion of the brain is removed, to disconnective procedures, and neuromodulation techniques such as Vagus Nerve Stimulation (VNS) or Deep Brain Stimulation (DBS), for cases where resection is not feasible or appropriate.
Treatment Overview
<h2>Overview of Epilepsy Surgery Treatment</h2><h3>A Path to Seizure Freedom</h3><p>Epilepsy surgery is a highly specialized neurosurgical intervention designed for individuals with drug-resistant epilepsy, where seizures persist despite optimal trials of anti-epileptic medications. The primary goal is to precisely locate and remove or disconnect the brain region (seizure focus) responsible for generating epileptic seizures. This advanced treatment aims to significantly reduce seizure frequency and intensity, or even achieve complete seizure freedom, thereby dramatically improving the patient's quality of life.</p><p>Techniques range from resective surgeries, where a portion of the brain is removed, to disconnective procedures, and neuromodulation techniques such as Vagus Nerve Stimulation (VNS) or Deep Brain Stimulation (DBS), for cases where resection is not feasible or appropriate.</p>
Procedures
Epilepsy surgery begins with extensive pre-surgical evaluation, including prolonged video-EEG monitoring, high-resolution MRI, and sometimes PET/SPECT scans, to precisely pinpoint the epileptogenic zone. Once localized, the patient undergoes general anesthesia. The neurosurgeon performs a craniotomy (opening in the skull) to access the brain. Depending on the type of surgery (e.g., temporal lobectomy, lesionectomy, hemispherectomy, corpus callosotomy), the identified seizure-generating tissue is carefully resected, or neural pathways are disconnected. Intraoperative monitoring, such as electrocorticography (ECoG), may be used to confirm the boundaries of the seizure focus and protect eloquent brain areas. For neuromodulatory procedures like VNS or DBS, a device is implanted, and electrodes are placed in specific brain regions or on the vagus nerve. The bone flap is then replaced, and the scalp is closed. The entire procedure is meticulously planned and executed by top neurosurgeons to maximize seizure control while minimizing neurological deficits, aiming for a high epilepsy surgery success rate.
Benefits
<h2>Benefits of Epilepsy Surgery Treatment</h2><h3>A New Horizon for Seizure Freedom and Quality of Life</h3><ul><li><strong>Significant Seizure Reduction or Freedom:</strong> The primary and most impactful benefit is a dramatic decrease in seizure frequency or, for many, complete cessation of seizures, greatly improving the epilepsy surgery success rate.</li><li><strong>Reduced Medication Dependency:</strong> Successful surgery often allows for a reduction in anti-epileptic drug dosages, minimizing side effects and improving overall health, leading to affordable epilepsy surgery solutions long-term.</li><li><strong>Improved Quality of Life:</strong> Freedom from seizures can lead to greater independence, improved social interactions, enhanced educational and employment opportunities, and better mental health, impacting every aspect of life after epilepsy surgery.</li><li><strong>Enhanced Cognitive Function:</strong> For some patients, reducing seizure burden can lead to improvements in memory, attention, and other cognitive abilities that were previously affected by epilepsy.</li><li><strong>Hope for a Brighter Future:</strong> Epilepsy surgery offers a definitive path towards a more predictable and fulfilling life, free from the constant fear and limitations imposed by recurrent seizures.</li><li><strong>Expert Care in India:</strong> Access to world-class neurosurgeons and state-of-the-art facilities at a fraction of the epilepsy surgery treatment cost found in Western countries, facilitated by DivinHeal's seamless care coordination.</li></ul>
Recovery Information
<h2>Epilepsy Surgery Recovery: What to Expect</h2><h3>A Smooth Path Back to Wellness with DivinHeal's Support</h3><ul><li><strong>Initial Hospital Stay:</strong> Typically 5-7 days, involving close monitoring in the ICU initially, followed by a move to a regular ward. Patients will be managed for pain, monitored for any neurological changes, and start their epilepsy surgery recovery journey.</li><li><strong>Immediate Post-Operative Period (Weeks 1-4):</strong> During this time, patients may experience headache, fatigue, nausea, or mood changes. It is crucial to follow medication schedules and activity restrictions (e.g., avoiding heavy lifting, driving). Physical and occupational therapy may begin to aid recovery.</li><li><strong>Intermediate Recovery (Months 1-3):</strong> Gradual return to normal activities. Cognitive rehabilitation or counseling may be recommended based on individual needs. Seizure medications are usually continued, with potential adjustments over time under strict neurological guidance. These are important epilepsy surgery recovery tips.</li><li><strong>Long-Term Recovery (Months 3+):</strong> Full recovery can take several months to a year. Regular follow-up appointments with neurologists and epileptologists are essential to monitor seizure control, adjust medications, and assess overall well-being. Lifestyle adjustments, stress management, and support groups play a vital role in long-term success.</li></ul><h3>Recovery Tips & Support:</h3><ul><li><strong>Follow Medical Advice:</strong> Adhere strictly to medication regimens and all post-operative instructions from your neurosurgeon.</li><li><strong>Rest and Gradual Activity:</strong> Allow your body ample time to heal; avoid strenuous activities initially and gradually increase your activity level.</li><li><strong>Rehabilitation:</strong> Engage actively in prescribed physical, occupational, or speech therapy to regain function.</li><li><strong>Emotional Support:</strong> Seek support from family, friends, and support groups. DivinHeal can help connect you with resources for emotional and psychological well-being.</li><li><strong>DivinHeal's Continuous Care:</strong> Our team provides ongoing assistance and follow-up coordination, ensuring you receive comprehensive support throughout your entire epilepsy surgery recovery time.</li></ul>

spinal fusion surgery
Treatment Price
$6500.00 USDOverview of Spinal Fusion Surgery
Spinal fusion aims to replicate the natural healing process of broken bones. During the procedure, a bone graft (either from your body, a donor, or synthetic material) is used to create a solid bridge between adjacent vertebrae. This graft material eventually fuses with the vertebrae, forming a single, stable bone segment. The goal is to alleviate chronic back pain, improve spinal stability, and restore function, enhancing a patient's quality of life.
Overview of Spinal Fusion Surgery
Spinal fusion aims to replicate the natural healing process of broken bones. During the procedure, a bone graft (either from your body, a donor, or synthetic material) is used to create a solid bridge between adjacent vertebrae. This graft material eventually fuses with the vertebrae, forming a single, stable bone segment. The goal is to alleviate chronic back pain, improve spinal stability, and restore function, enhancing a patient's quality of life.
Treatment Overview
<h2>Overview of Spinal Fusion Surgery</h2><p>Spinal fusion aims to replicate the natural healing process of broken bones. During the procedure, a bone graft (either from your body, a donor, or synthetic material) is used to create a solid bridge between adjacent vertebrae. This graft material eventually fuses with the vertebrae, forming a single, stable bone segment. The goal is to alleviate chronic back pain, improve spinal stability, and restore function, enhancing a patient's quality of life.</p>
Procedures
Spinal fusion surgery is performed under general anesthesia. The surgeon makes an incision (either in the back, abdomen, or side) to access the affected vertebrae. Depending on the approach, muscles may be moved aside. The damaged disc material (if applicable) is removed, and a bone graft material (autograft, allograft, or synthetic) is placed in the space between the vertebrae. Often, metal screws, rods, or cages are used to hold the vertebrae securely in place while the fusion occurs. Over several months, the bone graft grows, effectively 'welding' the vertebrae together into a single, solid bone. The incision is then closed.
Benefits
<h2>Benefits of Spinal Fusion Surgery</h2><ul><li><h3>Significant Pain Relief</h3><p>By stabilizing unstable or painful segments of the spine, spinal fusion can dramatically reduce chronic back or neck pain, especially when conservative treatments have failed.</p></li><li><h3>Improved Spinal Stability</h3><p>The procedure corrects instability caused by degenerative conditions, fractures, or deformities, preventing further damage and improving overall spinal integrity.</p></li><li><h3>Correction of Spinal Deformities</h3><p>Effective in treating conditions like scoliosis or spondylolisthesis, spinal fusion can correct abnormal spinal curvature and alignment, improving posture and function.</p></li><li><h3>Enhanced Quality of Life</h3><p>With reduced pain and improved stability, patients often experience a greater ability to participate in daily activities, work, and hobbies, leading to a better quality of life.</p></li><li><h3>Prevention of Further Nerve Damage</h3><p>By stabilizing the spine, spinal fusion can alleviate pressure on compressed nerves, preventing further neurological deficits and improving nerve function.</p></li></ul>
Recovery Information
<h2>Spinal Fusion Surgery Recovery Time and Tips</h2><p>Recovery from spinal fusion surgery is a gradual process that requires patience and adherence to medical advice. The initial hospital stay typically lasts 3-7 days, during which pain management and early mobilization are priorities.</p><ul><li><h3>Immediate Post-operative Period (Weeks 1-6)</h3><p>During this phase, activity will be restricted. You'll focus on light walking, avoiding bending, lifting, or twisting your spine. Pain management is crucial, and you'll receive guidance on medication and incision care. DivinHeal's care coordinators will ensure seamless post-operative support.</p></li><li><h3>Rehabilitation & Physical Therapy (Months 2-6)</h3><p>Once your surgeon clears you, a structured physical therapy program will begin. This is vital for regaining strength, flexibility, and proper body mechanics. Exercises will focus on core strengthening, gentle stretching, and improving endurance. Adherence to your physical therapy regimen is key for optimal spinal fusion recovery.</p></li><li><h3>Long-term Recovery & Lifestyle Adjustments (Months 6-12+)</h3><p>Full fusion can take 6-12 months, or even longer for some individuals. During this period, you will gradually return to more strenuous activities. Your surgeon will advise on specific restrictions. Long-term wellness aspects include maintaining a healthy weight, regular low-impact exercise, and practicing good posture. Emotional counseling can also be beneficial as you adapt to life after spinal fusion surgery.</p></li></ul>

avm brain surgery
Treatment Price
$8000.00 USDThe primary goal of AVM brain surgery is to eliminate the abnormal connection between arteries and veins, thereby reducing the risk of bleeding (hemorrhage) and associated neurological damage. Techniques include microsurgical resection for direct removal, endovascular embolization to block vessels, and stereotactic radiosurgery for targeted radiation. DivinHeal ensures access to leading neurosurgical centers equipped with advanced imaging and surgical technologies for precise and safe procedures.
The primary goal of AVM brain surgery is to eliminate the abnormal connection between arteries and veins, thereby reducing the risk of bleeding (hemorrhage) and associated neurological damage. Techniques include microsurgical resection for direct removal, endovascular embolization to block vessels, and stereotactic radiosurgery for targeted radiation. DivinHeal ensures access to leading neurosurgical centers equipped with advanced imaging and surgical technologies for precise and safe procedures.
Treatment Overview
The primary goal of AVM brain surgery is to eliminate the abnormal connection between arteries and veins, thereby reducing the risk of bleeding (hemorrhage) and associated neurological damage. Techniques include microsurgical resection for direct removal, endovascular embolization to block vessels, and stereotactic radiosurgery for targeted radiation. DivinHeal ensures access to leading neurosurgical centers equipped with advanced imaging and surgical technologies for precise and safe procedures.
Procedures
AVM brain surgery involves several specialized techniques tailored to the specific malformation. Microsurgical resection is the most common approach, where a neurosurgeon performs a craniotomy (opening in the skull) to directly visualize and meticulously disconnect and remove the AVM using a high-powered microscope and specialized instruments. Intraoperative angiography or Doppler ultrasound may be used to confirm complete removal. For some AVMs, endovascular embolization may be performed prior to or instead of surgery, where catheters are threaded through blood vessels to inject a glue-like substance that blocks off the AVM. Stereotactic radiosurgery (focused radiation) is another non-invasive option for smaller, deep-seated AVMs that are not amenable to direct surgery, aiming to gradually cause the AVM vessels to thrombose and close over time.
Benefits
<h2>Benefits of AVM Brain Surgery</h2><ul><li><h3>Reduced Risk of Hemorrhage</h3><p>The most significant benefit is the elimination or substantial reduction of the risk of life-threatening brain hemorrhage, which can cause severe stroke or death.</p></li><li><h3>Symptom Relief</h3><p>Surgical removal can alleviate AVM-related symptoms such as chronic headaches, seizures, and neurological deficits like weakness or sensory loss, improving the patient's quality of life.</p></li><li><h3>Definitive Treatment</h3><p>For many AVMs, microsurgical resection offers a definitive cure, removing the abnormal vessels entirely and preventing future complications.</p></li><li><h3>Enhanced Neurological Function</h3><p>By removing the AVM, pressure on surrounding brain tissue is relieved, potentially leading to improvement in neurological function that was previously compromised.</p></li><li><h3>Peace of Mind</h3><p>For patients and their families, successfully treating an AVM provides immense psychological relief from the constant worry of potential rupture.</p></li></ul>
Recovery Information
<h2>AVM Brain Surgery Recovery: What to Expect</h2><p>Recovery after AVM brain surgery is a gradual process and varies depending on the AVM's size, location, complexity of the surgery, and the patient's overall health. </p><h3>Immediate Post-Operative Period (Hospital Stay)</h3><ul><li>Patients typically remain in the ICU for a few days for close monitoring of neurological status, blood pressure, and intracranial pressure.</li><li>Hospital stay can range from 7 to 14 days, involving management of pain, swelling, and potential post-surgical complications.</li><li>Early mobilization and basic physiotherapy begin as soon as medically stable.</li></ul><h3>Long-Term Recovery (Weeks to Months)</h3><ul><li><strong>Physical Rehabilitation:</strong> Many patients require physical, occupational, and speech therapy to regain strength, coordination, and cognitive function. This can continue for several months.</li><li><strong>Managing Symptoms:</strong> Headaches, fatigue, and mood changes are common during recovery. Medications may be prescribed to manage seizures or other residual symptoms.</li><li><strong>Follow-up Imaging:</strong> Regular follow-up MRIs or angiograms are crucial to ensure complete AVM obliteration and monitor for any recurrence.</li><li><strong>Lifestyle Adjustments:</strong> Patients are advised to avoid strenuous activities, heavy lifting, and certain sports for a period, as recommended by the neurosurgeon. Emotional support and counseling can also be beneficial for psychological adjustment.</li></ul><p>DivinHeal provides comprehensive post-operative support, including coordination for rehabilitation services and follow-up consultations, ensuring a smooth and effective recovery journey.</p>

awake craniotomy
Treatment Price
$7000.00 USDOverview of Awake Craniotomy for Brain Tumors
Awake craniotomy aims for the maximal safe removal of brain tumors or lesions situated in eloquent (functionally critical) areas of the brain. By keeping the patient awake during key stages of the surgery, neurosurgeons can perform real-time mapping of brain functions, such as speech and motor control. This allows for precise tumor resection while preserving vital neurological functions, significantly reducing the risk of post-operative deficits and improving the patient's quality of life. This advanced technique leverages the brain's plasticity and the patient's direct feedback to achieve optimal surgical outcomes.
Overview of Awake Craniotomy for Brain Tumors
Awake craniotomy aims for the maximal safe removal of brain tumors or lesions situated in eloquent (functionally critical) areas of the brain. By keeping the patient awake during key stages of the surgery, neurosurgeons can perform real-time mapping of brain functions, such as speech and motor control. This allows for precise tumor resection while preserving vital neurological functions, significantly reducing the risk of post-operative deficits and improving the patient's quality of life. This advanced technique leverages the brain's plasticity and the patient's direct feedback to achieve optimal surgical outcomes.
Treatment Overview
<h2>Overview of Awake Craniotomy for Brain Tumors</h2><p>Awake craniotomy aims for the maximal safe removal of brain tumors or lesions situated in eloquent (functionally critical) areas of the brain. By keeping the patient awake during key stages of the surgery, neurosurgeons can perform real-time mapping of brain functions, such as speech and motor control. This allows for precise tumor resection while preserving vital neurological functions, significantly reducing the risk of post-operative deficits and improving the patient's quality of life. This advanced technique leverages the brain's plasticity and the patient's direct feedback to achieve optimal surgical outcomes.</p>
Procedures
1. Pre-operative Planning: Advanced MRI and fMRI scans are used to precisely map the tumor and eloquent brain regions. A multidisciplinary team plans the surgical approach. 2. Anesthesia and Craniotomy: The patient is initially sedated and a local anesthetic is administered. The skull is opened (craniotomy) to expose the brain while the patient is under mild sedation. 3. Awakening Phase: Sedation is lightened, and the patient is gently awakened. Communication with the surgical team begins. 4. Brain Mapping: The neurosurgeon, often with a neurophysiologist, uses direct electrical stimulation to map critical brain functions (e.g., speech, motor) while the patient performs specific tasks. This creates a 'safe zone' and 'no-go zone'. 5. Tumor Resection: Guided by the mapping, the surgeon meticulously removes the tumor or lesion, continuously interacting with the patient to monitor function and ensure preservation of critical areas. 6. Closure: Once maximal safe resection is achieved, the patient is sedated again, and the skull bone is replaced, and the scalp is closed. 7. Post-operative Monitoring: The patient is moved to a recovery area for close monitoring of neurological status and vital signs.
Benefits
<h2>Benefits of Awake Craniotomy Treatment</h2><ul><li><h3>Maximal Safe Tumor Resection</h3><p>The ability to map and monitor brain function in real-time allows neurosurgeons to remove as much of the tumor as possible without damaging critical areas, leading to better oncological outcomes.</p></li><li><h3>Preservation of Neurological Function</h3><p>Direct patient feedback during surgery helps protect vital functions such as speech, language, and motor skills, significantly reducing the risk of post-operative deficits.</p></li><li><h3>Improved Quality of Life</h3><p>By minimizing neurological damage, patients often experience a better quality of life post-surgery, maintaining their cognitive and physical independence.</p></li><li><h3>Enhanced Surgical Precision</h3><p>Intraoperative mapping provides unparalleled precision, guiding the surgeon to differentiate between healthy and pathological tissue in eloquent areas.</p></li><li><h3>Reduced Risk of Complications</h3><p>Real-time monitoring and patient cooperation help in avoiding critical areas, thereby lowering the chances of major neurological complications.</p></li><li><h3>Faster Recovery for Specific Functions</h3><p>For some patients, the precise preservation of functional areas can contribute to a quicker recovery of specific abilities post-surgery.</p></li></ul>
Recovery Information
<h2>Awake Craniotomy Recovery: What to Expect</h2><ul><li><h3>Immediate Post-Operative Period</h3><p>Immediately after awake craniotomy, patients are closely monitored in the ICU or a specialized neurosurgical ward. Initial recovery focuses on pain management, monitoring for complications, and ensuring neurological stability. Most patients will feel some pain or discomfort at the incision site, which is managed with medication.</p></li><li><h3>Hospital Stay and Early Rehabilitation</h3><p>The typical hospital stay for awake craniotomy is approximately 3 to 7 days. During this time, patients will begin gentle mobilization. Physical therapists, occupational therapists, and speech therapists will evaluate the patient's neurological function and initiate early rehabilitation tailored to any specific deficits that may arise or to reinforce existing strengths. The focus is on regaining strength, balance, and cognitive function.</p></li><li><h3>Home Recovery and Ongoing Therapy</h3><p>Upon discharge, continued recovery at home is crucial. The full recovery period can range from several weeks to several months, depending on the individual's overall health, the size and location of the tumor, and the extent of surgery. Patients will typically continue outpatient rehabilitation, including physical therapy, occupational therapy, and speech therapy, to maximize functional recovery and adapt to any changes.</p></li><li><h3>Long-Term Outlook and Follow-up</h3><p>Long-term recovery involves regular follow-up appointments with the neurosurgeon and oncologist, including imaging scans, to monitor for tumor recurrence. Lifestyle modifications, emotional support, and continued engagement in rehabilitative exercises are vital for sustained well-being. DivinHeal ensures coordinated follow-up care and access to support networks for a holistic recovery journey.</p></li></ul>

Spinal Cord Tumor Surgery
Treatment Price
$12000.00 USDOverview of Spinal Cord Tumor Surgery
Spinal Cord Tumor Surgery focuses on safely excising tumors while minimizing damage to delicate neural structures. The primary goals include relieving spinal cord compression, preserving neurological function, alleviating pain, and obtaining tissue for definitive diagnosis. Techniques vary depending on the tumor's location (intramedullary, intradural-extramedullary, or extradural), size, and relationship to the spinal cord. Advanced imaging, intraoperative neuro-monitoring, and microsurgical techniques are integral to successful outcomes.
Overview of Spinal Cord Tumor Surgery
Spinal Cord Tumor Surgery focuses on safely excising tumors while minimizing damage to delicate neural structures. The primary goals include relieving spinal cord compression, preserving neurological function, alleviating pain, and obtaining tissue for definitive diagnosis. Techniques vary depending on the tumor's location (intramedullary, intradural-extramedullary, or extradural), size, and relationship to the spinal cord. Advanced imaging, intraoperative neuro-monitoring, and microsurgical techniques are integral to successful outcomes.
Treatment Overview
<h2>Overview of Spinal Cord Tumor Surgery</h2><p>Spinal Cord Tumor Surgery focuses on safely excising tumors while minimizing damage to delicate neural structures. The primary goals include relieving spinal cord compression, preserving neurological function, alleviating pain, and obtaining tissue for definitive diagnosis. Techniques vary depending on the tumor's location (intramedullary, intradural-extramedullary, or extradural), size, and relationship to the spinal cord. Advanced imaging, intraoperative neuro-monitoring, and microsurgical techniques are integral to successful outcomes.</p>
Procedures
Spinal Cord Tumor Surgery typically begins with the patient under general anesthesia. The surgeon makes an incision over the affected area of the spine. A laminectomy, removing part of the vertebral bone, is often performed to access the spinal cord. Using specialized microsurgical instruments and intraoperative neuro-monitoring to safeguard delicate nerves, the neurosurgeon carefully dissects and removes the tumor. For intramedullary tumors, an incision into the spinal cord may be necessary. For tumors adhering to the spinal cord or nerves, meticulous dissection is required. Once the tumor is removed, the spinal cord is visually inspected, and the incision is closed layer by layer.
Benefits
<h2>Benefits of Spinal Cord Tumor Surgery</h2><ul><li><h3>Neurological Preservation</h3><p>The primary benefit is the potential to preserve or improve neurological function by decompressing the spinal cord and nerve roots.</p></li><li><h3>Pain Relief</h3><p>Surgical removal often alleviates pain, numbness, weakness, and other debilitating symptoms caused by tumor compression.</p></li><li><h3>Definitive Diagnosis</h3><p>Surgery provides tissue for histopathological analysis, allowing for accurate diagnosis and guiding further treatment strategies.</p></li><li><h3>Improved Quality of Life</h3><p>Successful surgery can significantly enhance a patient's quality of life by restoring function and reducing symptoms.</p></li><li><h3>Prevention of Progression</h3><p>Removes the tumor, preventing further growth and potential irreversible neurological damage.</p></li></ul>
Recovery Information
<h2>Spinal Cord Tumor Surgery Recovery Time and Tips</h2><p>Recovery from Spinal Cord Tumor Surgery is a gradual process and varies significantly depending on the tumor's location, size, patient's overall health, and the extent of neurological deficits pre-surgery. Typically, the initial hospital stay is 5-10 days, followed by several weeks to months of rehabilitation.</p><h3>Immediate Post-operative Period (Hospital Stay)</h3><ul><li><strong>Pain Management:</strong> Controlled with medication.</li><li><strong>Mobility:</strong> Gradual mobilization under medical supervision.</li><li><strong>Monitoring:</strong> Close observation for neurological changes or complications.</li></ul><h3>Rehabilitation Phase (Weeks to Months)</h3><ul><li><strong>Physical Therapy:</strong> Essential for restoring strength, balance, and mobility.</li><li><strong>Occupational Therapy:</strong> Helps patients regain independence in daily activities.</li><li><strong>Emotional Support:</strong> Counseling can be vital for coping with the emotional impact of recovery.</li><li><strong>Lifestyle Modifications:</strong> Adherence to physician's instructions regarding activity levels, lifting restrictions, and wound care.</li></ul><p>Full recovery of strength and sensation can take anywhere from 3 months to over a year. Regular follow-up appointments with your neurosurgeon and neuro-oncologist are crucial to monitor recovery and detect any potential recurrence.</p>

Neuro Rehabilitation Program
Treatment Price
$5000.00 USDOverview of Neuro Rehabilitation Programs
Neuro rehabilitation aims to restore function, reduce impairments, and improve the overall well-being of individuals affected by neurological disorders or injuries. This multidisciplinary program leverages advanced techniques to facilitate brain plasticity and nerve recovery, helping patients regain independence in daily activities. DivinHeal connects you with top-tier rehabilitation centers specializing in personalized care plans, ensuring access to cutting-edge therapies and compassionate support.
Overview of Neuro Rehabilitation Programs
Neuro rehabilitation aims to restore function, reduce impairments, and improve the overall well-being of individuals affected by neurological disorders or injuries. This multidisciplinary program leverages advanced techniques to facilitate brain plasticity and nerve recovery, helping patients regain independence in daily activities. DivinHeal connects you with top-tier rehabilitation centers specializing in personalized care plans, ensuring access to cutting-edge therapies and compassionate support.
Treatment Overview
<h2>Overview of Neuro Rehabilitation Programs</h2><p>Neuro rehabilitation aims to restore function, reduce impairments, and improve the overall well-being of individuals affected by neurological disorders or injuries. This multidisciplinary program leverages advanced techniques to facilitate brain plasticity and nerve recovery, helping patients regain independence in daily activities. DivinHeal connects you with top-tier rehabilitation centers specializing in personalized care plans, ensuring access to cutting-edge therapies and compassionate support.</p>
Procedures
A Neuro Rehabilitation Program typically involves a multi-disciplinary team delivering various therapies. Upon admission, a comprehensive assessment is conducted by neurologists, physiatrists, physical therapists, occupational therapists, and speech-language pathologists. Based on this, an individualized treatment plan is created. Daily therapy sessions include targeted exercises for motor skill recovery, balance, coordination, and strength (Physical Therapy). Patients also engage in activities to relearn daily living skills, fine motor control, and adaptive strategies (Occupational Therapy). Communication and swallowing difficulties are addressed through speech therapy. Cognitive rehabilitation focuses on memory, attention, and problem-solving. Psychological counseling supports emotional well-being. The program often integrates advanced technologies like robotics, virtual reality, and biofeedback. Progress is regularly assessed, and the treatment plan is adjusted to maximize functional outcomes. Discharge planning includes recommendations for home exercises, adaptive equipment, and continued outpatient therapy.
Benefits
<h2>Benefits of a Neuro Rehabilitation Program</h2><ul><li><h3>Improved Physical Function</h3><p>Regain strength, balance, coordination, and mobility, leading to greater independence.</p></li><li><h3>Enhanced Cognitive Abilities</h3><p>Improve memory, attention, problem-solving skills, and overall cognitive function.</p></li><li><h3>Better Communication Skills</h3><p>Overcome speech and language difficulties, enhancing social interaction and expression.</p></li><li><h3>Increased Independence in Daily Life</h3><p>Master activities of daily living (ADLs) such as dressing, eating, and personal hygiene.</p></li><li><h3>Reduced Complications</h3><p>Minimize risks like muscle atrophy, contractures, and pressure sores.</p></li><li><h3>Emotional and Psychological Well-being</h3><p>Receive support for depression, anxiety, and adjustment challenges, fostering mental resilience.</p></li><li><h3>Better Quality of Life</h3><p>Achieve a higher level of functional independence and participation in meaningful activities, leading to a more fulfilling life.</p></li></ul>
Recovery Information
<h2>Neuro Rehabilitation Program Recovery Time and Tips</h2><h3>Expected Recovery Timeline</h3><p>The Neuro Rehabilitation Program recovery time is highly individual, varying significantly based on the underlying condition, severity of injury, individual progress, and intensity of the program. Acute inpatient rehabilitation typically lasts from 2 to 6 weeks, followed by outpatient therapy that can continue for several months or even years. Significant improvements are often seen within the first 3-6 months, but progress can continue for much longer due to neuroplasticity.</p><h3>Tips for Optimal Recovery</h3><ul><li><strong>Adherence to Therapy:</strong> Consistently follow your personalized Neuro Rehabilitation Program therapies and techniques, both during supervised sessions and at home.</li><li><strong>Healthy Lifestyle:</strong> Maintain a balanced diet, stay hydrated, and ensure adequate sleep to support brain healing and overall energy levels.</li><li><strong>Regular Exercise:</strong> Incorporate recommended physical activities to maintain strength, flexibility, and cardiovascular health.</li><li><strong>Cognitive Engagement:</strong> Engage in mentally stimulating activities like puzzles, reading, and learning new skills to boost cognitive function.</li><li><strong>Emotional Support:</strong> Seek counseling or join support groups to address emotional challenges, anxiety, and depression. DivinHeal can connect you with appropriate resources.</li><li><strong>Family Involvement:</strong> Encourage family members to understand and participate in the recovery process, providing a supportive home environment.</li><li><strong>Patience and Persistence:</strong> Recovery from neurological conditions is a marathon, not a sprint. Celebrate small victories and remain persistent despite setbacks.</li><li><strong>Follow-up Care:</strong> Regularly attend follow-up appointments with your medical team to monitor progress and adjust your Neuro Rehabilitation Program as needed.</li></ul>
Hospitals Offering this treatment
India offers premium medical procedures at affordable prices. Discover our most popular treatments, delivered by the country's finest doctors.

Hisar Intercontinental Hospital
Saray Mah. Siteyolu Cad. No:7, Umraniye, 34768, Istanbul, Turkey
Hisar Intercontinental Hospital

Medical Park Group, Istanbul
Fahrettin Kerim Gokay Cad. Tıbbiye Cd., Kadikoy, Istanbul, Turkey
Medical Park Group, Istanbul

Emsey Hospital, Pendik, Istanbul
Çamlık, Selçuklu Cd. No:22, 34912 Pendik/İstanbul, Türkiye
Emsey Hospital, Pendik, Istanbul


American Hospital, Istanbul
Guzelbahce Sk. No:20, 34365, Nisantasi, Istanbul, Turkey
American Hospital, Istanbul

Memorial Hospitals Group
Burhaniye, Nagehan Sokağı No:4/A D:1, 34676 Üsküdar/İstanbul, Türkiye
Memorial Hospitals Group

Florence Nightingale Hospital Istanbul
Abide-i Hürriyet Cd No:166, 34381 Sisli, Istanbul
Florence Nightingale Hospital Istanbul

Medicana International Hospital, Istanbul
Halit Ziya Turkkani Mah. Medikal Park Cd. No:1, Beylikdüzü, İstanbul
Medicana International Hospital, Istanbul

Okan University Hospital Istanbul
Icmeler Mah. Aydınlıyolu Cd. No:2, 34947 Icmeler-Tuzla, Istanbul
Okan University Hospital Istanbul

Kolan International Hospital, Istanbul
Kaptanpasa Mah. Okmeydan Kavsagi, Darulaceze Cd. No:14, 34384 Sisli, Istanbul
Kolan International Hospital, Istanbul
Meet Our Doctors
Meet our team of highly qualified and experienced medical professionals dedicated to providing the best healthcare services.

Brig. Dr. H.S. Bhatoe
Director - Neuro Surgery, Max Hospital, Saket & Patparganj
Neuro Surgery
New Delhi
50+ Years
Experience
Apolo Delhi
Hospital
1500
Fees

Dr. Abhideep Chaudhary
Chairman & HOD, HPB Surgery and Liver Transplantation
HPB Surgery, Liver Transplantation, Surgical Gastroenterology, Robotic Surgery, Biliary Sciences
New Delhi
20+ Years
Experience
Max Hospital,Gurgaon
Hospital
1500
Fees

Dr. Aditya Gupta
Chairperson - Neurosurgery & CNS Radiosurgery & Co-Chief - Cyberknife Centre, Artemis Hospitals, Gurgaon
Neurosurgeon
Haryana
32+ Years
Experience
Artemis Hospital
Hospital
1500
Fees

Dr. Ajay Lall
Principal Director - Pulmonology
Pulmonology
New Delhi
40+ Years
Experience
Max Hospital,Gurgaon
Hospital
1500
Fees

Dr. Alok Joshi
Director
Neurosciences
New Delhi
14+ Years
Experience
Apolo Delhi
Hospital
1500
Fees

Dr. Amit Shrivastava
Director
Neurology
New Delhi
20+ Years
Experience
Apolo Delhi
Hospital
1500
Fees

Dr. Anil Sharma
Director
Neurology
New Delhi
30+ Years
Experience
Apolo Delhi
Hospital
1500
Fees

Dr. Anita Sethi
Director
Neurology
New Delhi
28+ Years
Experience
Apolo Delhi
Hospital
1500
Fees

Dr. Anjali Vaish
Consultant - Physiotherapy and Rehabilitation Centre
Physiotherapy and Rehabilitation Centre
New Delhi
10+ Years
Experience
Artemis Hospital
Hospital
1500
Fees

Dr. Arun Saroha
Director & HOD
Neurosurgery
New Delhi
30+ Years
Experience
Apolo Delhi
Hospital
1500
Fees
Booking With DIVINHEAL
Get a free consultation to understand your treatment options
Frequently Asked Questions
Get answers to common questions about medical tourism, treatment procedures, and our comprehensive healthcare services.