
Written by DivinHeal Editorial Contributor, Samrat Nilesh, Embryologist | Medically Reviewed by Dr Indu Priya, Gynecologist(MBBS,MD) Published on: 2026-05-04
What Is a Transvaginal Ultrasound? A Complete Guide for Patients From UAE, UK and Nigeria
🔑 KEY TAKEAWAYS |
Been told you need a transvaginal ultrasound? You probably have questions. What is it? Does it hurt? What will it show? This guide answers all of that. It is written for patients from the UAE, UK, and Nigeria. Some of you are thinking about having the scan at a JCI-accredited hospital in India. Others are having it at home. Both groups will find what they need here.
What Is a Transvaginal Ultrasound and How Does It Work?
How the TVS Probe Works
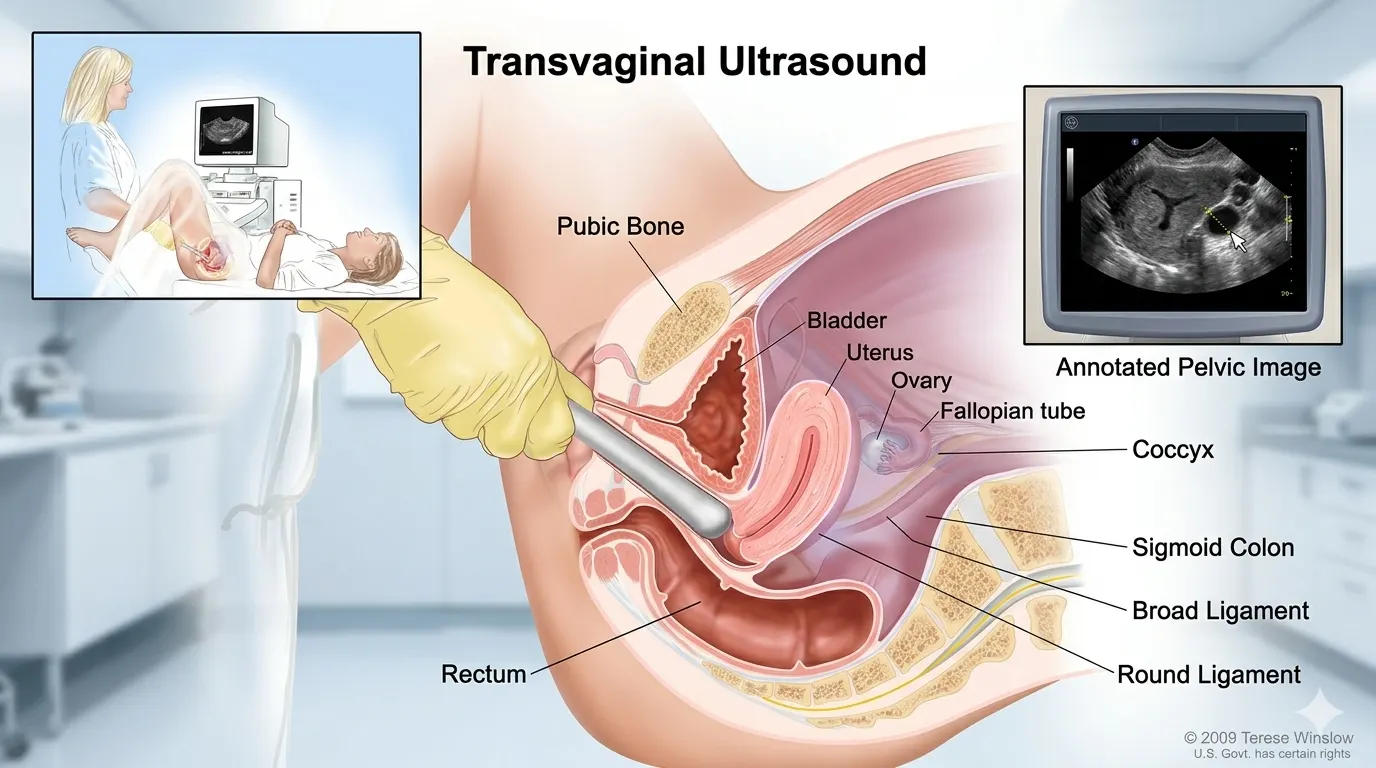
A transvaginal ultrasound (TVS) uses sound waves to make images of the female pelvic organs. Doctors also call it an internal ultrasound or endovaginal scan. A smooth, slender probe is used. It is about 2–3 cm wide — roughly the size of a tampon. The probe is covered with a clean, single-use sheath and coated in gel. The sonographer gently places it a few inches inside the vagina. The probe sends out sound waves. Those waves bounce off your internal organs and return as images on a screen. No radiation is used.
The probe is inside the body, just centimetres from the uterus and ovaries. This is why the images are much clearer than an external abdominal scan. An abdominal scan has to send sound waves through the belly wall first. The standard TVS makes 2D images. Many JCI-accredited Indian hospitals also offer advanced 3D and 4D TVS for complex cases. These include Apollo Hospitals Chennai, Medanta Gurgaon, and Fortis Memorial Research Institute Gurgaon.
The probe connects to an ultrasound machine and screen. The sonographer moves and slightly rotates the probe to get images from different angles. The scan takes about 15–30 minutes. You may feel mild pressure as the probe moves. Most patients do not find this painful.
Why Would a Woman Need an Internal Transvaginal Ultrasound?
Your doctor or gynecologist may recommend a TVS for several reasons:
- Unexplained pelvic pain or abnormal vaginal bleeding — including pain that is worse at certain cycle phases, or bleeding between periods or after menopause.
- Early pregnancy — to confirm the pregnancy is inside the uterus, detect a fetal heartbeat (from about 5–6 weeks), and measure gestational age more accurately than an abdominal scan.
- Suspected ectopic pregnancy — when a fertilized egg implants outside the uterus (most often in the fallopian tube). TVS is the main tool for finding this early, before rupture.
- Fertility assessment — to monitor follicle growth during an IVF cycle, check the uterine lining, and find structural reasons for difficulty conceiving.
- Gynecological conditions — to look into symptoms linked to PCOS, uterine fibroids, ovarian cysts, endometriosis, adenomyosis, or pelvic inflammatory disease (PID).
- Postmenopausal bleeding — to check the thickness of the uterine lining. Thickening can indicate a problem.
- IUD placement — to confirm that an intrauterine device is sitting in the right position.
A TVS is often ordered after an abdominal scan finds something that needs a closer look. It is not always the first scan — but it is the best choice when detailed pelvic images are needed.
Pelvic Ultrasound vs Transvaginal Ultrasound: Which Is More Accurate?
Neither scan is always better. They work in different ways and are used at different stages. The right one depends on what your doctor is looking for.
Feature | Transabdominal (Pelvic) Ultrasound | Transvaginal Ultrasound (TVS) |
How it's done | The Probe moved across the lower abdomen | A slender probe was gently inserted into the vagina |
Bladder preparation | Full bladder required — pushes bowel aside for clearer images | Empty or partially empty bladder — a full bladder may obscure details |
Image clarity | Good for larger structures (e.g., large fibroids, ovarian masses); less detailed for small structures | Excellent for small structures — endometrial polyps, early gestational sacs, follicles, early ectopics |
Accuracy for... | General pelvic survey; large structural abnormalities; advanced pregnancy | Early pregnancy; PCOS follicle monitoring; endometrial thickness; small fibroids/cysts |
Duration | 15–30 minutes | 15–30 minutes |
Which is more accurate? | More accurate for broad overview and larger pelvic structures | More accurate for small, detailed internal findings — the preferred tool for most gynecological diagnoses |
Source: RCOG (Royal College of Obstetricians and Gynecologists) Good Practice No. 14 — Ultrasound in Obstetrics and Gynecology; BMUS (British Medical Ultrasound Society) Ultrasound Safety Guidelines; NHS clinical guidance on pelvic ultrasound.
When Is a Transvaginal Ultrasound Preferred Over an Abdominal One?
TVS is the better choice when the target is small or deep inside the body. Think of an early gestational sac before 8 weeks. Or small ovarian follicles during a fertility cycle. Or an endometrial polyp just a few millimetres across. The TVS probe is very close to these organs. The images it produces cannot be matched by an abdominal scan.
An abdominal scan works better for a few situations. It is preferred for a first look at a large pelvic mass, where a wide view is more useful than a close-up. It is also preferred when a patient strongly does not want an internal scan. And it is the standard for routine pregnancy scans in the second and third trimesters, when the baby has grown beyond the pelvis.
For UK patients: the NHS refers patients for TVS when an abdominal scan is not clear enough. It is also the first scan for suspected ectopic pregnancy. This follows RCOG guidance. For UAE and Nigerian patients: your doctor in India will recommend the right scan for you. You do not need to decide in advance.
What Does a Transvaginal Ultrasound Show?
A TVS gives detailed images of the uterus (body and cervix) and both ovaries. It also shows the uterine lining. The fallopian tubes are only visible when something is wrong, such as fluid or a blockage. Here is what it can find in clinical practice:
Condition | What the TVS Reveals | Clinical Significance |
PCOS | Enlarged ovaries containing 12+ small follicles (string-of-pearls appearance); increased ovarian volume | Diagnostic criterion per ESHRE/ASRM Rotterdam Consensus (2003, updated 2018) |
Uterine Fibroids | Location (submucosal, intramural, subserosal), number, size, and vascularity | Guides treatment — submucosal fibroids affecting the uterine cavity are most relevant to fertility. |
Ovarian Cysts | Size, internal structure (simple/complex/septate), vascularity (Doppler); differentiates benign from potentially concerning | Simple unilocular cysts ≤5 cm are usually benign and monitored; complex or vascular cysts need further evaluation. |
Endometriosis | Endometriomas (chocolate cysts) on the ovaries; bowel endometriosis is less visible; deep infiltrating endometriosis (requires an experienced sonographer) | TVS has ~90% sensitivity for detecting ovarian endometriomas; laparoscopy requires direct diagnosis |
Early Pregnancy | Gestational sac from ~4.5 weeks; embryo + heartbeat from ~5–6 weeks; crown-rump length measure accurate | Confirms intrauterine pregnancy before rupture (ACOG, 2019), detects ectopic pregnancies |
Endometrial Thickness | Measures lining thickness; assesses texture (echogenicity) | Postmenopausal women: >4–5 mm warrants investigation for endometrial pathology; IVF monitoring for receptivity |
References:
ESHRE/ASRM Rotterdam Criteria for PCOS (2003, updated 2018);
ACOG Practice Bulletin No. 193 – Ectopic Pregnancy (2019);
RCOG Endometrial Assessment;
NICE Clinical Guideline CG154 – E
What Cancers Can a Pelvic Ultrasound Detect?
A TVS can spot features that may point to certain cancers. But it is not a cancer screening test on its own. A biopsy or surgical test is always needed to confirm cancer.
Ovarian cancer: TVS can identify complicated ovarian masses. Such masses may include solid tumors, internal masses, or increased blood flow detected by Doppler studies. This increases the suspicion of cancer, leading to further tests like CA-125 serum testing, CT scans, or consultations with an expert. The combination of TVS and CA-125 is utilized in the UK Collaborative Trial of Ovarian Cancer Screening (UKCTOCS).
Endometrial (uterine) cancer: TVS is the first-line test for postmenopausal bleeding — the most common symptom of endometrial cancer. A thickened uterine lining (above 4–5 mm in postmenopausal women) on TVS triggers a biopsy. TVS does not diagnose endometrial cancer directly. It tells doctors which patients need a biopsy.
Cervical cancer: TVS cannot see early cervical cancer. That is why cervical smear/Pap tests and HPV testing are the right screening tools. But advanced cervical cancer that has spread into the uterus may be visible on TVS.
What TVS cannot do: diagnose cancer on its own, or tell the difference between all benign and cancerous masses with certainty. It also cannot screen for ovarian cancer in the general population. This is not currently recommended for low-risk women — there is not enough evidence of benefit.
Is a Transvaginal Ultrasound Painful? Separating Fact From Fear
The most searched question about TVS is whether it hurts. For most patients, the answer is no. It is not painful — but it can feel mildly uncomfortable. Knowing what to expect helps reduce anxiety before the procedure.
What Does a TVS Actually Feel Like?
The probe is about the width of a finger. It is covered with a clean, single-use sheath and coated in gel. The sonographer inserts it slowly and gently — or you can insert it yourself. NHS guidance is clear on this: you can ask to insert the probe yourself. Many clinics now offer this as standard.
Once inside, you may feel mild pressure or fullness as the sonographer angles the probe to image different areas. This is not sharp pain. It is closer to the feeling of a speculum exam — but most patients say it is less uncomfortable. A 2022 patient study published in the Journal of Ultrasound in Medicine found that over 90% of patients tolerated the procedure well with minimal discomfort. For most people, the worry beforehand is worse than the procedure itself.
When is it more uncomfortable? A small number of patients may feel more discomfort. This includes patients with active pelvic inflammatory disease, endometriosis with adhesions, vaginismus, or a history of sexual trauma. Tell the sonographer before the probe is inserted. They can reposition, use a smaller probe, or switch to an abdominal scan. You are in control. You can ask for the scan to be paused or stopped at any point.
Patient Priya from Lagos recalls her visit to Apollo Hospitals Chennai: "For eight months, I postponed getting this scan done as I was afraid that it might be painful. However, the lady sonographer first made sure to explain everything to me, allowed me to insert the probe by myself, and before I knew it, it was all done. My images came out clear, and my doctor was able to diagnose right away." This example mirrors the sentiments of many other patients who visited Apollo Hospitals.
Composite patient story for illustration. Real patient experiences available from Divinheal coordinators on request.
Tips for a More Comfortable Transvaginal Ultrasound
- Talk to the sonographer before the probe is inserted. Tell them about any anxiety, past trauma, or physical conditions. They can adjust their approach, use a smaller probe, or let you insert it yourself.
- Try abdominal breathing. Breathe in slowly through the nose and out through the mouth during insertion. This helps the pelvic floor muscles relax. It reduces discomfort from muscle tension.
- Request a female sonographer. At all Divinheal partner hospitals — Apollo Chennai, Fortis Noida, Medanta Gurgaon, MAX Delhi, Artemis Gurgaon, and Paras Hospitals — female sonographers are available for gynecological scans. Request this when booking.
- Empty your bladder beforehand. A full bladder adds pressure to the pelvic area during the scan. Emptying it before the procedure makes things more comfortable.
- Tell the team about any latex allergy. Probe covers are usually made of latex. If you have a latex allergy, tell the reception team when booking so a latex-free cover is ready.
Can a Virgin Have a Transvaginal Ultrasound? What Unmarried Patients Need to Know
This is one of the most important — and most searched — questions for patients from the UAE, Nigeria, and other communities. For many, the distinction between married and unmarried patients carries cultural or social meaning. Both the clinical answer and the cultural guidance matter here.
Clinically: Can a Virgin Have a Transvaginal Ultrasound?
Yes, in most cases. The TVS probe (about 2–3 cm in diameter) is smaller than a tampon applicator. For women who use tampons, the probe causes no physical change. For women with an intact hymen, the decision is made case by case. Many can still have a TVS using the smallest available probe with a gentle technique. Others prefer not to, and this choice is always respected. The Fairfax Radiology Center (USA) notes that TVS may not suit some patients with an intact hymen. A transabdominal scan, CT, or MRI are valid alternative in such cases.
Main point: TVS doesn’t have anything to do with virginity from a medical perspective. Hymen is not an anatomical determinant of virginity. Insertion of a TVS probe with correct technique and with the patient’s consent does not make any statements regarding her sexual history. Our Indian partner hospitals treat it with the utmost professional confidentiality.
For UAE and Nigerian Patients: Unmarried Women and Cultural Context
In the UAE, this falls under the Dubai Health Authority and Abu Dhabi HAAD rules. In Nigerian clinical settings, the same applies. Gynecological scans, including TVS, are provided to unmarried patients for clinical reasons. This includes PCOS, pelvic pain, fertility checks, and early pregnancy. There is no legal barrier in India to performing TVS for unmarried patients.
For UAE patients concerned about privacy: in India, your medical records are kept strictly confidential under NABH and JCI patient rights standards. No information about your treatment is shared with anyone — including family members — without your written consent. You control who knows about your medical appointments.
Islamic Modesty Protocols: What Indian Hospitals Provide for UAE Patients
Divinheal partner hospitals are experienced in caring for patients from the UAE, Gulf, and South Asian Muslim communities. Here is what is available at JCI/NABH-accredited partner hospitals:
- Female sonographers: all partner hospitals provide female sonographers for all gynecological scans, including TVS. Request this when booking. It will be confirmed in writing before your appointment.
- No male medical personnel in the scan room: any additional staff (students, junior doctors) can only enter the room if you explicitly invite them. You have the right to an all-female clinical team throughout.
- Privacy draping: Full modesty draping is standard at JCI hospitals. You will be covered at all times except for the immediate area being examined.
- Arabic-speaking patient coordinators: Divinheal assigns an Arabic-speaking coordinator for all UAE patients. The coordinator is available before, during (outside the scan room), and after the appointment.
Sarah from London, who got her TVS done at Medanta Gurgaon after a 11 week long NHS waiting period, said about her experience: “The lady sonographer greeted me, elaborated on the process of the scan, and asked if I wanted to put the probe inside my vagina myself. It was completed in just 20 minutes, with the results available within 24 hours. NHS had instructed me to wait 11 weeks.”
Composite patient story. Real patient testimonials available from Divinheal coordinators on request.
Is a Transvaginal Ultrasound Safe During Pregnancy?
Yes. TVS is safe throughout pregnancy, including in the first trimester. The sound waves used carry no radiation. They pose no known risk to the embryo or fetus. ACOG, RCOG, and the World Health Organization (WHO) all confirm this. There are no documented cases of TVS causing miscarriage.
Why TVS Is Preferred in Early Pregnancy
In the first trimester (weeks 4–12), the embryo is too small and too deep in the pelvis for an abdominal scan to image it well. TVS can detect a gestational sac at about 4.5 weeks. It can show an embryo with a heartbeat at about 5–6 weeks. It can also measure crown-rump length (CRL) for accurate gestational age dating.
ACOG Practice Bulletin No. 193 (Ectopic Pregnancy, 2019) names TVS as the primary tool for suspected ectopic pregnancy. It can detect a tubal gestational sac before symptoms of rupture develop. Early detection of an ectopic pregnancy can be life-saving. A ruptured ectopic is a medical emergency. TVS at 5–6 weeks can find an ectopic pregnancy before the fallopian tube ruptures in most cases.
TVS Safety and Patient Anxiety During Pregnancy
Many expectant patients from Nigeria and the UAE worry that an internal scan might cause harm. This concern is understandable. Here is the direct answer. The TVS probe does not touch the cervix during a standard pregnancy scan. The probe rests in the vaginal vault. Images are captured using sound waves. No physical contact with the gestational sac, embryo, or uterine lining occurs. The scan cannot cause a miscarriage. Multiple large studies — including the FASTER trial (US, 2005) and ISUOG guidelines (2019) — confirm the safety of first-trimester TVS.
For patients who have experienced a previous miscarriage, the TVS is not a cause of concern. The emotional anxiety of the appointment is completely understandable. Indian partner hospital sonographers are trained to handle early pregnancy scans with care and sensitivity. You can always bring a companion to the appointment.
Transvaginal Ultrasound Cost: India vs UAE, UK, Nigeria and Australia
A TVS is one of the most affordable diagnostic scans available in India. The comparison below covers private-healthcare rates. NHS and public hospital scans in the UK and Australia are free or heavily subsidised for eligible patients — but wait times vary significantly.
Country | Local Currency | USD Equiv. | INR Equiv. | Notes |
India | ₹700–₹5,000 | $9–$30 | — | JCI/NABH-accredited hospitals; 3D/4D capability available |
UAE | AED 300–1000 | $82–$272 | ₹8,000–₹23,000 | Dubai/Abu Dhabi private clinic rate; hospital rates may be higher |
UK | £150–£350 | $160–$440 | ₹10,000–₹37,000 | NHS free for eligible patients; private clinic rates shown here |
Nigeria | ₦10,000–₦50,000 | $5–$18 | ₹500–₹2,000 | Availability of 3D/4D TVS varies by city and facility |
Australia | AUD $130–$500 | $100–$330 | ₹9,000–₹28,000 | Private clinic rates; Medicare may rebate a portion for clinically indicated scans |
Costs for India based on private hospitals and diagnostic centers in Delhi, Chennai, and Mumbai, JCI/NABH- accredited. Private clinics in the UK based on verified prices from top private imaging centers in the UK (2025–2026). Costs for the UAE are based on costs at Dubai and Abu Dhabi private hospitals and clinics. Costs for Nigeria based on rates in Lagos and Abuja diagnostic centers. Costs for are Australia based on costs at private imaging centers; a Medicare rebate may apply. Exchange rates are 1 USD = ₹83; 1 USD = AED 3.67; 1 USD = £0.79; 1 USD = AUD 1.52.
The savings for UAE and UK patients at India’s JCI-accredited hospitals are about 80–90% per scan. For a single TVS, the saving in absolute terms is modest. The real value shows when a patient is in India for a broader workup — a fertility consultation or IVF cycle. The TVS is bundled into the diagnostic package at very little extra cost.
For Nigerian patients: India’s main advantage over Nigeria is diagnostic capability, not cost. Advanced TVS features — 3D volumetric imaging of the uterine cavity, Doppler vascularity assessment of ovarian masses, sonoelastography for endometriosis — are standard at JCI partner hospitals. They may not be available locally. Maria from Lagos came to Fortis Memorial Research Institute, Gurgaon, for a fertility workup. She received a 3D sonohysterography (saline infusion TVS) to map her uterine cavity. This scan was not available at any clinic she had visited in Lagos.
Composite patient story for illustration. Real patient data available from Divinheal coordinators on request.
What is included in an Indian TVS package for international patients:
- Initial consultation with the gynecologist or radiologist
- The TVS scan (2D standard; 3D/4D if clinically indicated)
- A full written report with images in English, emailed to you within 24–48 hours
- Follow-up discussion of findings with the treating gynecologist.
- Visa assistance, airport transfer, and accommodation coordinated by Divinheal as part of the India visit planning
How to Prepare for a Transvaginal Ultrasound: Before, During, and After
What Is the Best Time to Do a TVS Test? Preparation and Timing
For most reasons — pelvic pain, abnormal bleeding, a pelvic mass — a TVS can be done at any point in your menstrual cycle. Timing matters more in specific situations:
When / Timing | Recommendation | Why |
Bladder | Empty or mostly empty your bladder just before the scan | A full bladder can compress pelvic structures, reducing image quality for TVS |
Clothing | Wear a two-piece outfit (top + skirt/trousers rather than a dress) | You'll undress from the waist down; two-piece clothing makes this much easier |
Hygiene | A normal shower or bath is sufficient. No special intimate hygiene preparation needed. | Standard cleanliness is all that is required. Shaving is not necessary or recommended. |
Eating/drinking | No fasting required. Eat and drink normally before the scan. | TVS is not affected by food intake, unlike abdominal scans for organs like the liver |
Best cycle timing | For routine gynecological assessment: any time in the cycle is acceptable. For PCOS follicle monitoring: Day 2–5. For IVF: specific protocol timing (clinic will advise). For endometrial assessment: Day 5–10. | Cycle timing affects what the scan can show — ovaries look different at different cycle phases. |
Latex allergy | Inform the clinic in advance if you have a latex allergy | Probe covers are usually latex; latex-free alternatives must be prepared in advance |
The timing guidance is based on the safety recommendations from BMUS (British Medical Ultrasound Society) and RCOG regarding gynecological ultrasonography. The timing of your IVF scans will be determined by your clinic according to your stimulation program.
What to Expect During Your First Internal Ultrasound
On arrival, you will be taken to a changing area and asked to undress from the waist down. A gown or drape is provided for your privacy. You will lie on an examination couch, usually on your back with your knees bent and slightly apart. Some centres use stirrups for the feet. Others do not — ask which position the clinic uses if you have a preference.
The sonographer introduces themselves and explains each step before they begin. This is the moment to mention any pelvic pain, past trauma, latex allergy, or a wish to insert the probe yourself. The probe — covered, lubricated, and at room temperature — is introduced slowly. You can ask the sonographer to pause at any stage.
As part of the scan procedure, the sonographer will carefully maneuver the transducer to visualize the uterus, ovaries, and endometrium. Sometimes, you will experience gentle pressure from the sonographer's free hand on your abdominal area to visualize structures. This is completely normal and will not hurt you. The lights might be dimmed for better visibility of the screen.
After the scan, wipe the lubricant with a paper towel and get dressed immediately. No recovery time is needed. Most patients return to normal activities straight away. The sonographer may share a first impression immediately after the scan. The full written report is usually ready within 24–48 hours. If you are on a Divinheal-coordinated visit, the report is emailed directly to you and your referring physician.
Managing Cramping After a Transvaginal Ultrasound
Some patients feel mild cramping after a TVS. It is similar to mild period pain. It is normal and clears up within a few hours without treatment. Paracetamol (1 g) or ibuprofen (400 mg with food, if tolerated) manages this well. A warm compress or hot water bottle on the lower abdomen also helps.
When should one consider seeking medical assistance? If one experiences intense pain following the procedure, he/she should consult the doctor. One should report any excessive vaginal bleeding other than spotting, a fever higher than 38°C, or any abnormal vaginal discharge. If there is cramping that does not resolve within 48 hours, one should seek medical help as well.
Your Divinheal Journey: Travelling From the UAE, UK or Nigeria to India for a Transvaginal Ultrasound
The TVS may also be performed as part of a more extensive examination process. It could be for fertility concerns, a gynecological examination regarding pelvic pain, or for further clarification of an ultrasound diagnosis. Divinheal schedules the entire visit, including the scan.
Step-by-Step Process for International Patients
Initial contact and records review: Provide your medical history, reports of recent scans, and symptoms briefly to Divinheal. Within 3 to 5 working days, you will be sent a list of specialist doctors available in JCI/NABH-certified hospitals along with an estimate of test costs.
Booking and visa: Divinheal issues the required hospital invitation letter for an Indian e-Medical Visa upon confirmation of the hospital and specialist. Citizens from the UAE, UK, and Nigeria normally get the e-Medical Visa in 5-10 working days. Companions will require an e-Visa for medical attendants.
Travel: In case of TVS, only consultation or brief diagnostic tests for gynecology, a duration of 2 to 4 days in India is sufficient. One-day duration is required for consultation and test, while one additional day is needed to go through reports and plan further steps if needed. Extra days can be included if you wish to take additional tests.
Country-specific notes:
- For UAE patients- direct flights connect Dubai and Abu Dhabi to Delhi, Chennai, and Mumbai (3–4 hours). Divinheal assigns an Arabic-speaking coordinator. All partner hospitals provide gynecological care through female medical teams.
- For UK patients — direct flights from London Heathrow to Delhi (8–9 hours) and Chennai (10 hours). NHS referral letters are accepted by Indian partner hospitals and can form the basis of your India consultation.
- For Nigerian patients — Divinheal provides dedicated visa documentation support and flight routing help from Lagos and Abuja. A dedicated coordinator is available via WhatsApp from the first enquiry through post-scan follow-up.
Ready to Book Your Transvaginal Ultrasound in India?
A Divinheal consultation starts with a review of your symptoms and any existing investigation results. Within 3–5 working days, a coordinator returns recommended specialists, hospital options, and a written cost estimate — in your preferred currency. No travel commitment is required at this stage.
Patients from Dubai, Abu Dhabi, London, Manchester, Lagos, and Abuja have used Divinheal to book transvaginal ultrasounds and full gynecological workups. They have been seen at Apollo Chennai, Medanta Gurgaon, Fortis Noida, MAX Delhi, Artemis Gurgaon, and Paras Hospitals. Contact a Divinheal coordinator to request your free gynecology consultation today.
⚠️ MEDICAL DISCLAIMER | |
Related Links
International Patient Visiting India
- ivf in vitro fertilization cycle in pune for bangladesh
- ivf in vitro fertilization cycle in hyderabad for bangladesh
- ivf in vitro fertilization cycle in india for uae
- ivf in vitro fertilization cycle in chennai for uae
- ivf in vitro fertilization cycle in chennai for bangladesh
- ivf in vitro fertilization cycle in bengaluru for bangladesh
- ivf in vitro fertilization cycle in mumbai for bangladesh
- ivf in vitro fertilization cycle in new delhi for bangladesh
- ivf in vitro fertilization cycle in india for bangladesh
Other Treatment related Information
- ivf in vitro fertilization cycle
- IVF (In Vitro Fertilization) Cycle Treatment in Haryana
- IVF (In Vitro Fertilization) Cycle Treatment in Pune
- IVF (In Vitro Fertilization) Cycle Treatment in Hyderabad
- Best IVF (In Vitro Fertilization) Cycle Hospitals in New Delhi
- Best IVF (In Vitro Fertilization) Cycle Hospitals in India
- Best IVF (In Vitro Fertilization) Cycle Hospitals in Chennai
- Best IVF (In Vitro Fertilization) Cycle Hospitals in Gurugram
- Best IVF (In Vitro Fertilization) Cycle Hospitals in Pune
- Best IVF (In Vitro Fertilization) Cycle Doctors in Gurugram
- Best IVF (In Vitro Fertilization) Cycle Doctors in New Delhi
Booking With DIVINHEAL
Get a free consultation to understand your treatment options
Related Links
International Patient Visiting India
- ivf in vitro fertilization cycle in pune for bangladesh
- ivf in vitro fertilization cycle in hyderabad for bangladesh
- ivf in vitro fertilization cycle in india for uae
- ivf in vitro fertilization cycle in chennai for uae
- ivf in vitro fertilization cycle in chennai for bangladesh
- ivf in vitro fertilization cycle in bengaluru for bangladesh
- ivf in vitro fertilization cycle in mumbai for bangladesh
- ivf in vitro fertilization cycle in new delhi for bangladesh
- ivf in vitro fertilization cycle in india for bangladesh
Other Treatment related Information
- ivf in vitro fertilization cycle
- IVF (In Vitro Fertilization) Cycle Treatment in Haryana
- IVF (In Vitro Fertilization) Cycle Treatment in Pune
- IVF (In Vitro Fertilization) Cycle Treatment in Hyderabad
- Best IVF (In Vitro Fertilization) Cycle Hospitals in New Delhi
- Best IVF (In Vitro Fertilization) Cycle Hospitals in India
- Best IVF (In Vitro Fertilization) Cycle Hospitals in Chennai
- Best IVF (In Vitro Fertilization) Cycle Hospitals in Gurugram
- Best IVF (In Vitro Fertilization) Cycle Hospitals in Pune
- Best IVF (In Vitro Fertilization) Cycle Doctors in Gurugram
- Best IVF (In Vitro Fertilization) Cycle Doctors in New Delhi
DivinHeal's Journey

Latest Articles
Frequently Asked Questions
Get answers to common questions about medical tourism, treatment procedures, and our comprehensive healthcare services.
Ready To Start Your Healing Journey?
Get Personalized Medical Treatment Options From India's Top Hospitals. Our Medical Experts Are Ready To Assist You Every Step Of The Way.










