Centres Of Excellence
Our Centres of Excellence bring together multidisciplinary teams to deliver precise diagnosis, advanced treatments, and superior outcomes across a wide spectrum of medical specialties.

OVERVIEW
Gastroenterology Treatment: Comprehensive Care for Digestive Health
Gastroenterology treatment focuses on the intricate health of the digestive system. At DivinHeal, we connect you with leading gastroenterologists and state-of-the-art facilities across India, offering a spectrum of care from diagnostic endoscopy to advanced surgical interventions. Our goal is to provide effective, compassionate, and affordable Gastroenterology treatment, ensuring optimal outcomes and a swift return to health for conditions ranging from common digestive complaints to complex gastrointestinal diseases.
PROCEDURE
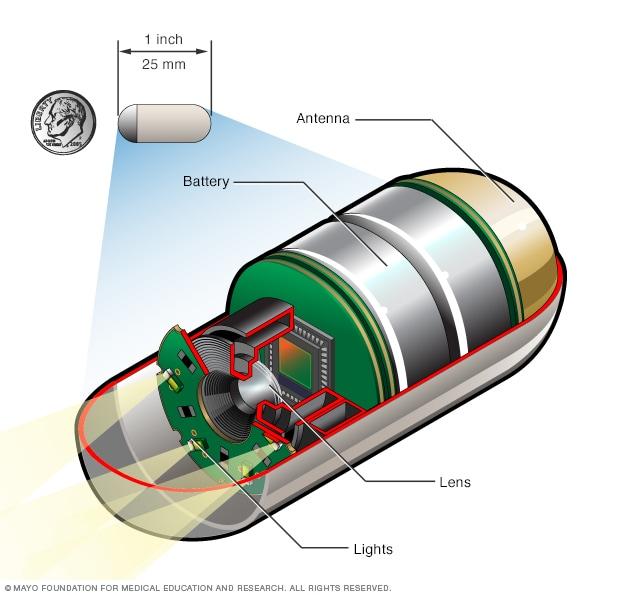
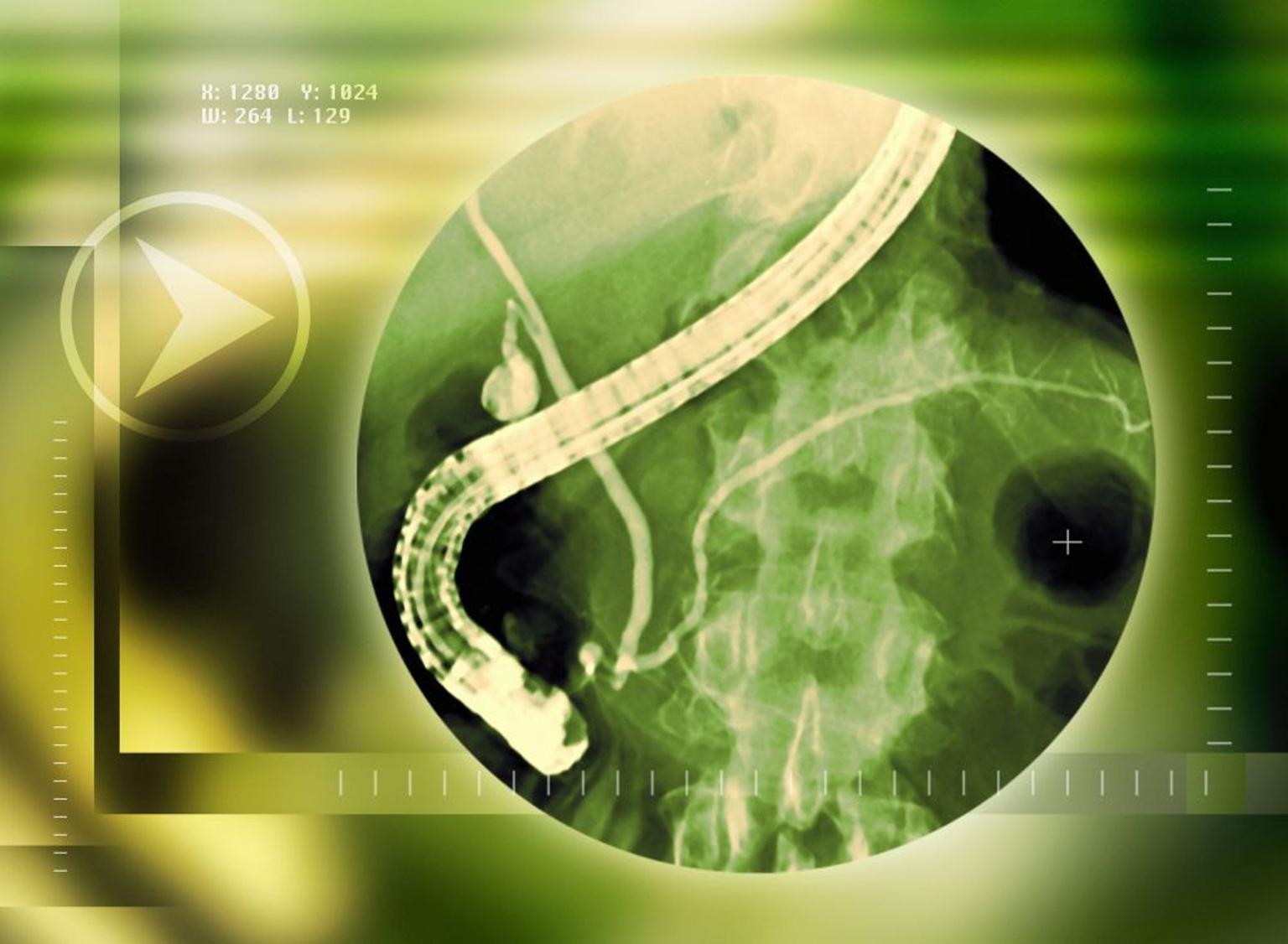
Gastroenterology procedures range from non-invasive diagnostic tests to complex surgical interventions. Diagnostic procedures often include upper endoscopy (EGD), colonoscopy, sigmoidoscopy, capsule endoscopy, endoscopic ultrasound (EUS), and endoscopic retrograde cholangiopancreatography (ERCP) to visualize and sample tissues within the digestive tract. Therapeutic endoscopic procedures can involve polyp removal, stricture dilation, stent placement, or bleeding control. Medical management typically includes pharmacotherapy with anti-inflammatory drugs, immunosuppressants, biologics, or acid suppressants. Surgical interventions may range from minimally invasive laparoscopic procedures (e.g., cholecystectomy, appendectomy, anti-reflux surgery) to open abdominal surgeries for complex conditions like large tumor resections, bowel resections for IBD, or liver and pancreatic surgeries. For gastrointestinal cancers, Gastroenterology chemotherapy and radiation therapy, alongside Gastroenterology targeted therapy, may be integral parts of a multimodal treatment plan, aiming for disease control and improved prognosis.
BENEFITS
Benefits of Advanced Gastroenterology Treatment
Improved Digestive Function
Effective management and resolution of conditions leading to better digestion and nutrient absorption.
Pain & Symptom Relief
Alleviation of chronic abdominal pain, discomfort, bloating, and other debilitating GI symptoms.
Enhanced Quality of Life
Freedom from daily digestive struggles, allowing patients to enjoy food and activities without fear or discomfort.
Prevention of Complications
Early diagnosis and intervention can prevent progression of diseases, reduce risk of cancer, and avoid emergency situations.
Access to Innovative Therapies
Benefit from the latest advancements in medical, endoscopic, and surgical Gastroenterology diagnosis and therapy options.
RECOVERY
Gastroenterology Recovery Time and Tips
The Gastroenterology recovery time varies significantly depending on the specific procedure performed and the patient's overall health. Simple diagnostic endoscopies might involve only a few hours of recovery, while complex abdominal surgeries could require several weeks to months for full recuperation.
Post-Procedure Care
Adhere strictly to your physician's instructions regarding diet, medication, and activity levels. This often includes a gradual reintroduction of foods, pain management, and avoiding strenuous activities.
Lifestyle Modifications
Many GI conditions benefit from long-term lifestyle changes, including a balanced diet, regular exercise, stress management, and adequate hydration.
Follow-up Appointments
Regular follow-up with your gastroenterologist is crucial to monitor progress, adjust medications, and address any lingering concerns. DivinHeal assists in coordinating these appointments.
Emotional Support
Coping with chronic digestive conditions can be challenging. We encourage seeking support from family, friends, or support groups, and can help connect you with counseling services if needed for comprehensive Gastroenterology recovery.
WHAT WE TREAT
Conditions Treated in Gastroenterology
Inflammatory Bowel Disease (IBD)
Including Crohn's Disease and Ulcerative Colitis, managed through medication, dietary adjustments, and sometimes surgery.
Gastroesophageal Reflux Disease (GERD)
Treatments range from lifestyle changes and medication to advanced endoscopic or surgical interventions.
Peptic Ulcer Disease
Management of stomach and duodenal ulcers caused by H. pylori infection or NSAID use.
Liver Diseases
Such as hepatitis (viral, autoimmune), fatty liver disease, cirrhosis, and liver cancer, requiring specialized medical and interventional care.
Pancreatic Disorders
Including pancreatitis (acute and chronic), pancreatic cysts, and pancreatic cancer, often involving complex diagnosis and multidisciplinary treatment.
Gallstone Disease
Medical management or surgical removal of the gallbladder (cholecystectomy).
Celiac Disease & Malabsorption Syndromes
Dietary management and medical therapy to improve nutrient absorption.
Colorectal Polyps & GI Cancers
Early detection, endoscopic removal of polyps, and comprehensive Gastroenterology chemotherapy and radiation therapy, surgery, and Gastroenterology targeted therapy for various gastrointestinal cancers (esophageal, stomach, colorectal, liver, pancreatic).
Irritable Bowel Syndrome (IBS)
Symptom management through diet, lifestyle, and medication.
PREPARATION
Preparation for Gastroenterology treatment is highly individualized. For endoscopic procedures like colonoscopy, bowel preparation with laxatives is necessary. For upper endoscopies, an overnight fast is required. Prior to any surgical procedure, patients typically undergo comprehensive pre-operative assessments, including blood tests, imaging scans, and cardiac evaluations. Medication review is crucial; patients may be advised to stop blood thinners or certain diabetes medications before some procedures. Detailed instructions regarding diet, fasting, and medication adjustments will be provided by your medical team well in advance to ensure optimal safety and efficacy.
RISKS
While Gastroenterology treatments are generally safe, potential risks exist, varying by procedure. Common risks associated with endoscopic procedures include bleeding, infection, and rarely, perforation of the digestive tract. Surgical risks can include bleeding, infection, adverse reactions to anesthesia, wound complications, and damage to surrounding organs. For medical therapies, side effects can range from mild (nausea, fatigue) to more severe allergic reactions or immunosuppression. For treatments involving Gastroenterology chemotherapy and radiation therapy, common risks include hair loss, fatigue, nausea, and increased infection risk. Your medical team will discuss specific risks relevant to your chosen Gastroenterology diagnosis and therapy options and take all precautions to minimize them.
JOURNEY
Your Gastroenterology Treatment Journey with DivinHeal
Initial Consultation & Diagnosis
Your journey begins with a thorough evaluation by a top gastroenterologist. This involves a detailed medical history, physical examination, and advanced diagnostic tests such as endoscopy, colonoscopy, capsule endoscopy, MRI, CT scans, or specialized blood tests to accurately pinpoint the cause of your digestive issues. DivinHeal facilitates seamless appointments and secure transfer of medical records.
Personalized Treatment Planning
Based on your diagnosis, a multidisciplinary team collaborates to devise a personalized Gastroenterology diagnosis and therapy options plan. This may include medical management with medication, advanced endoscopic procedures, or surgical intervention. Your care coordinator ensures you understand every aspect of your treatment.
Treatment & Hospital Stay
Whether it's a medical regimen, an outpatient endoscopic procedure, or inpatient surgery, you'll receive care at one of India's best hospitals for Gastroenterology. Our partner hospitals boast cutting-edge technology and highly experienced medical staff, ensuring safety and efficacy. DivinHeal provides end-to-end support, from visa and travel arrangements to hospital admission and discharge.
Recovery & Follow-up
Post-treatment, our team assists with your Gastroenterology recovery time and tips. This includes coordinating follow-up appointments, providing guidance on diet and lifestyle modifications, and arranging for any necessary rehabilitation or ongoing medical management. We ensure a smooth transition back to your daily life, emphasizing long-term wellness.
OUTCOMES
Expected outcomes include significant relief from digestive symptoms, improved organ function, and a better overall quality of life. Long-term prognosis often involves successful management or resolution of conditions, enabling patients to return to normal activities with enhanced well-being.
Related Links
Doctors For Treatment in Similar Locations
- Best Gastroenterology Doctors in Bengaluru
- Best Gastroenterology Doctors in Chennai
- Best Gastroenterology Doctors in Gurugram
- Best Gastroenterology Doctors in Hyderabad
- Best Gastroenterology Doctors in India
- Best Gastroenterology Doctors in Mumbai
- Best Gastroenterology Doctors in New Delhi
- Best Gastroenterology Doctors in Pune
Best Hospital Near by for treatment
- Best Gastroenterology Hospitals in Bengaluru
- Best Gastroenterology Hospitals in Chennai
- Best Gastroenterology Hospitals in Gurugram
- Best Gastroenterology Hospitals in Hyderabad
- Best Gastroenterology Hospitals in India
- Best Gastroenterology Hospitals in Mumbai
- Best Gastroenterology Hospitals in New Delhi
- Best Gastroenterology Hospitals in Pune
Related Treatments
Hospitals Offering this treatment
India offers premium medical procedures at affordable prices. Discover our most popular treatments, delivered by the country's finest doctors.
Meet Our Doctors
Meet our team of highly qualified and experienced medical professionals dedicated to providing the best healthcare services.
Booking With DIVINHEAL
Get a free consultation to understand your treatment options
Frequently Asked Questions
Get answers to common questions about medical tourism, treatment procedures, and our comprehensive healthcare services.